
430.6K
Downloads
164
Episodes
Here at The VBAC Link, our mission is to improve birth after Cesarean by providing education, support, and a community of like-minded people. NO matter what way you choose to birth, we want to support you during your journey in helping you know your options for birth. Welcome to our circle; we are so glad you are here!
Episodes

Wednesday Dec 30, 2020
157 Home Birth and Hospital Birth, Risks vs Benefits
Wednesday Dec 30, 2020
Wednesday Dec 30, 2020
It’s an ongoing and classic debate-- home birth versus hospital birth. Trying to decide where to have your VBAC is one of the toughest decisions to make. There are LOTS of opinions out there to navigate. Julie and Meagan sit down with you today to share some pros and cons (and some myth busters!) of each based on their personal experiences as doulas, as well as the most current evidence-based research out there.
This discussion is only the beginning.
We include tons of resources with even more information about these topics to help you continue your research and get closer to making your informed decision. We hope this episode leaves you feeling empowered and more confident in your birth choices no matter where you end up birthing.
Additional links
How to VBAC: The Ultimate Preparation Course for Parents
VBAC Link Blogs:
Home Birth After C-section (HBAC)
What to Write in a VBAC Birth Plan
13 Tips to Prepare for an Empowering Birth
Evidence-Based Birth® article: What is Home Birth?
Episode sponsor
This episode is sponsored by our signature course, How to VBAC: The Ultimate Preparation Course for Parents. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course. Together, Meagan and Julie have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head over to thevbaclink.com to find out more and sign up today.
Full transcript
Note: All transcripts are edited to eliminate false starts and filler words.
Meagan: Hello, hello. It’s Meagan and Julie with The VBAC Link, and today, you just have us. Lucky you. We’re so excited to be with you today.
Julie: Woohoo!
Meagan: We’re going to actually be talking on a very, very sensitive topic in a lot of areas because this can be one of those lovely debates out there. We’re talking hospital birth versus home birth. Definitely, something that we know some people are passionate about on both sides. That is great, and we love that, but today we want to talk about all the evidence on both sides, the pros and the cons, and how to determine what’s best for you.
Julie: Absolutely. I’m excited. We actually have a blog about this, I think. I’m looking it up right now.
Meagan: We do. We do.
Julie: Home birth versus hospital? I know we have one on Natural Birth versus Epidural. We have Writing a Home Birth Plan; we have an HBAC one, Natural Birth versus Epidural. I don’t think we have a hospital versus home birth. We have Laboring at Home.
Meagan: We don’t?!
Julie: We need to write one.
Meagan: Oh, Laboring at Home. Yeah.
Julie: Yeah. So basically, during this episode, we’re going to talk about a lot of things that we cover in our blog, so go to our blog right now and search for “home birth.” It’s going to bring up results Laboring at Home, What to Write in a VBAC Birth Plan-- that’s for a hospital or home birth. We have-- let’s see.
Meagan: Home Birth After Cesarean. We’ve got lots of stories on the podcast.
Julie: Uh-huh. We’ve got Natural Birth versus Epidural, lots of podcast stories, How to Write a Home Birth Plan, all sorts of things. And then, we’re going to tell our content writer who tells us what to do about blogs that we need a home birth versus hospital birth blog.
Meagan: Yeah, we do. We totally do.
Review of the Week
Julie: We do. Maybe there will be one there by the time this episode airs. Alright, but should I read a review?
Meagan: You should read a review.
Julie: Alright. I’ve got one from Google. We haven’t read a Google review in a long time. So, if you didn’t know that, you can review us on Apple Podcasts, you can review us on Google by just searching for The VBAC Link, and you can review us on Facebook. We love reading and having reviews from all three of those platforms. It keeps us going when the times get tough.
This review from Google is from Anne McLaughlin. She says, “These ladies are an absolute joy to listen to on their podcast! I feel so fortunate to have found them on my journey to what will hopefully be a 2VBAC with twins! When I had my 1st VBAC, I felt educated, as I had read through books and websites. Now, I feel empowered! Thanks to Julie and Meagan, I feel more confident advocating for myself and asking the right questions. I recommend you to all of the mamas I come across in other VBAC groups and often refer to specific episodes I've listened to. Thank you for all that you do, you Women of Strength, you!”
No, thank you, you Woman of Strength, you! Do you know what? I just saw in our Facebook community a twin birth posted.
Meagan: Oh, really? Really, that’s awesome.
Julie: I’m going to go stalk her and see if it was that same one. I’m actually in it right now.
Meagan: Yeah. That would be fun if it was. It would be super fun.
Julie: Anne McLaughlin.
Meagan: We’re stalking you, Anne.
Julie: Let’s see. Nope. She might not be in our community.
Meagan: Speaking of, if you didn’t know, we do have a community, and no, we don’t usually stalk you.
Julie: Only if you leave a review. Don’t put your real name on it.
Meagan: Only if you leave a review. So, it’s on Facebook, and if you search The VBAC Link Community, you will find us. Now, we do have questions that you have to answer, and we are kind of strict on it. So, you have to answer all three or—
Julie: Two. There are only two now.
Meagan: Oh yeah. There are two now. You have to answer both, or you don’t get added in. Sorry. We love you, but we really want to protect our group and keep everyone safe.
So, if you are not with us in that community, definitely check it out on Facebook, The VBAC Link Community. I promise you’re going to love it because these people in this group are just incredible. I am honestly learning from them. Do you find that, Julie? You see a post, and you’re like, “I actually didn’t know that was a thing,” and I go and research it.
Julie: Yes, or I make a statement and then somebody else says, “Actually, blah blah blah,” and I am like, “Do you know who I am? I own this community.” Then I go and research it, and I was like, “Oh crap. I was wrong.”
Meagan: Oh, that’s funny. That’s funny.
Julie: Okay, I found it. Anne McLaughlin in our Facebook group. I am looking at her story. Oh, shoot, wait. Let’s see—growth scans. Oh no, this is on October 26th. Dang, it. September no. Oh well. We will have to see. I’m going to be looking while we are talking, so if I interrupt the episode, you will know. Because she’s new, she should have been due-- or maybe she is still pregnant. I don’t know.
Episode sponsor
Julie: Do you want a VBAC but don’t know where to start? It’s easy to feel like we need to figure it all out on our own. That’s what we used to do, and it was the loneliest and most ineffective thing we have ever done. That’s why Meagan and I created our signature course, How to VBAC: The Ultimate Preparation Course for Parents, that you can find at thevbaclink.com. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course.
Together, Meagan and I have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head on over to thevbaclink.com to find out more and sign up today. That’s thevbaclink.com. See you there.
Hospital birth versus home birth
Julie: Anyways, we’re going to be done talking about Ms. Anne right now, and we’re going to talk about hospital birth versus home birth.
Meagan: Let’s do it.
Meagan: This is something as individuals-- we’ve both had a hospital birth and, well, you had a home birth. I had a birth center, which is kind of like a home birth, right?
Julie: Yeah, pretty much.
Meagan: Yeah. I mean, out-of-hospital birth. So I definitely know the difference from my personal perspective on birth, but then I have also attended many births as a doula in hospital. In fact, I would say the majority of my clients deliver in hospital, which is something that a lot of people don’t realize. A lot of people think doulas are only supporters for natural, unmedicated birth, and I’m just going to myth bust that one right there.
Julie: Boom.
Meagan: It’s not. It’s not. And really, I would say, 85 to 90% of our clients are in hospitals. I definitely have seen a lot of hospital birth, and then I’ve definitely seen home birth. I’m excited to talk about the things that I’ve seen and the differences on both.
Julie: I’m excited, too. We both have, I think, things that rub us the wrong way that we see some providers do constantly. I want to preface this before we get into it, that these are just experiences that we’ve seen in the birth room, at-home birth, hospital birth, and birth center birth. It’s not to be replaced by advice from your provider. It doesn’t necessarily mean that your provider’s doing anything wrong if they do things that we see that we don’t necessarily like. Some of us like some things that the other one doesn’t like. It’s going to be a fun conversation.
I actually found Anne‘s post. She had her babies. They were a TOLAC turned elective Cesarean. So she had a repeat Cesarean after an induced TOLAC. It looks like she chose a Cesarean. She hasn’t written up their birth stories yet, but they look beautiful and well and nice, chunky 8 pounds, 7 ounces and 7 pounds, 7 ounces twins.
Meagan: Wow, twins. Those are nice sized babies for twins.
Julie: I know, right? Nice chunky little boys.
Meagan: That’s cool. That’s awesome.
Julie: Well, now, you know.
Meagan: Congrats, Anne. Yes.
Julie: Alright. I don’t know how to get started.
Meagan: Well, first of all, I want to talk about home birth in general.
Julie: Do it.
Meagan: A lot of people are very, very scared of home birth, right? Because of that fear that is placed upon us. I say the word “uterine rupture”-- two words. Uterine rupture. That is a very scary thing to think of. Doing it at home, and the thought of not being right next to an OR can be scary and intimidating. Really, really hard to comprehend. Is it safe? Is home birth safe after all? There is something on our blog, so I’m jumping into home births first versus hospital. I don’t necessarily suggest one or the other, generally. This is very much a personal decision, but I just want to share this.
It says, “Homebirth in general, and especially home birth after Cesarean, also known as HBAC, is growing in popularity. In 2013, 1.4% of U.S. births took place outside of a hospital. Laboring at home is common, but many women also decide to stay home for the birth itself. Surprisingly, 64.4% of these occurred at home.”
64.4. That’s a pretty high number. That is really high. I mean, that was in 2013, so that was years ago. But still, it’s actually more common than you may think, and it’s more safe than you think.
So, okay. I’m going to go backwards. I want to talk about-- how do you know? How do you know what to do or where to go? How to decide? How do you know what to decide to do?
One, I think it’s really important to write a pros and cons list for yourself because everyone is different. Everyone is going to see different pros and different cons. Some peoples’ pros are going to be those other peoples’ cons. So write a pros and cons list.
Be honest with that pros and cons list. If money is a factor, write it down. Money. Insurance will cover it, right? If fear is a factor or a con, then write it down. Fear. Then, let’s break those down. Okay. What is the fear surrounding? What brings this fear? Then, let’s educate on those topics and see if that fear still stays. If that fear still stays and you were like, “Nope. I still feel very comfortable at the hospital,” stay at the hospital. If you’re like, “Oh, well actually, I didn’t know that it was not like that,” then that may change your mind for a home birth.
This is something that I’ve stuck with for so long. Honestly, ever since Blyss Young with-- I don’t know if you guys know Dr. Stu’s Podcast, but Blyss Young-- she said this, and I just can’t even let go of it. I can’t because it’s too good.
It’s the analogy of like, okay. For our weddings, we pick out the flowers. We pick out the venue. We go to places. We get comfortable. We pick out the colors. We are picking out the destination, and everything included, right? And then, for some reason, when it comes to birth, which is another very big day of our lives, we let our insurance companies tell us exactly what we’re going to do. I loved that when she said it, I was like, “Whoa. I never even thought of it like that.”
So, yes. Money can be a factor, but don’t let someone tell you who you can deliver with, where you can deliver, and how you can deliver if that’s not something you’re comfortable with. You may be like, “I don’t care really where I go; I just want to have a baby.” And that’s okay, too. But just keep that in mind.
So, writing a pros and cons list, really understanding the facts, and then following your intuition. I know Julie, and I talk about it all the time but follow your intuition. It’s huge. If your intuition says, “I shouldn’t be there,” then don’t go there, wherever “there” is. Right? And it’s hard to differentiate fear versus intuition. But usually, if you are feeling scared, that’s not your intuition. Right, Julie? It’s fear creeping in. So, talk about that.
Julie: Yeah. I want to touch on that. I feel like sometimes we don’t explain enough about what intuition is. I actually made a post yesterday because I wrote about a blog about how to have an empowering birth experience.
Your intuition doesn’t have to be a warm and fuzzy, feel-like-you-get-wrapped-in-a-big-hug, and be 100% confident in your decision. Intuition can look a lot of ways. The decisions that you make because of your intuition or the things that your intuition is telling you can cause a fear in you. In that case, that would be an indication that you need to do some processing and make sure that you enter into whatever decision you made with confidence as much as you can.
But sometimes, depending on yourself, acting on your intuition can look like asking questions when something doesn’t feel right to you. It can look like taking a look at the big picture rather than what’s happening at this exact moment. Or checking in with what you’re saying to yourself.
Your self-talk, sometimes self-talk, we confuse with intuition. Let’s check-in. Do you say things to yourself like, “Oh my gosh, I’m going to have such a hard time finding a provider.” Well, how can we turn that into a more productive statement? Like, “Alright. I know that I can find the right provider for my birth. I know that I can do the work necessary.” Things like that. Asking for reassurance from others sometimes.
I know for me-- oh my gosh, Meagan can attest to this, but I need reassurance big time. If I am making decisions, and I’m trusting my gut, and I’m taking a leap; I need people to tell me that it’s the right choice. Even if they think that I am completely off my rocker, right?
Meagan: Yeah, no. Totally, yeah.
Julie: I need it. Words of affirmation is my love language. Reassurance is a big thing. Reassurance that I’m trusting myself and that I’m making the right decision based on the things that I know and feel. Not second-guessing yourself. If it was the right decision when you made it, can I keep trusting that that’s the right decision? Also, trust that if changes need to be made, then you will know when and if they do need to be made.
Forgiving yourself can be part of trusting your intuition because sometimes we have to forgive ourselves for not knowing what we didn’t know or making decisions that we didn’t know we could’ve made differently when they happened.
And allowing yourself to feel negative emotions. Oh my gosh, please, please, please, can we say that again? Allowing yourself to feel negative emotion. Sometimes people think, “Oh, only positive vibes. Good vibes only when I’m preparing for my birth.” But if you do not allow yourself to feel and process those emotions and then send them off to their own little wherever-negative-emotions-go land, then you’re going to be doing yourself a great disservice because they can come up and appear while you’re in labor and birth. It can negatively impact the physiologic process of your birth.
Then, just being kind and loving to yourself. Sometimes that is simply what your intuition needs you to do. Just stop and slow down. Take a break and be kind to yourself.
But, yeah. I like that. I think that it’s important to clarify that intuition doesn’t just look like a still voice while you’re in a quiet and dark room.
Meagan: Right, right. And not allowing all of the outside static to impact it. Because I feel like it kind of just jumbles around, and you’re like, “Wait, what? Now, what am I feeling? Is that intuition? Is that opinion? Is that fair? I don’t know? Oh, what is it?” Do you know what I mean? There is so much. So, yeah. I love that. Perfect.
Let’s talk about hospital birth. What are the pros of hospital birth? Let’s talk about them. Pros and cons.
Julie: Well, I think the biggest pro of hospital birth is probably the biggest pro of home birth too, is making sure that it’s a space you’re comfortable in. Because some people just don’t feel comfortable, and they never will feel comfortable giving birth at home, right? If you’re not comfortable, then what happens? Everything locks up, and your physiologic process is destroyed. The obvious pros of hospital birth really are if you have an emergency that needs immediate attention, then your baby can be out of your body in 1-2 minutes with a crash Cesarean. I think that immediate access to emergency resources and care is probably the biggest pro about hospital birth.
Meagan: Yeah, just having access to that care. Comfortability. Also, I don’t know. I think in some ways there is a pro of having more-- now this could be the pro and a con in both ways, but more resources. Does that make sense? So, say you’re going. You’re 9 centimeters, and there is this lip or whatever. There are other things you can do at home, but sometimes a drop of Pitocin really does help. Or, say you are pushing for hours and hours, and you have a provider that is right there that can help assist with vacuum or forceps. Does that make sense? So, those are little pros that we wouldn’t really think that they are pros because they are not something we want to think of a pro, but it’s there. If we are home and we’ve been pushing for a long time, we have to get in the car and transfer. Or get in an ambulance and transfer. Sorry, I’m getting deep into the not super--
Julie: I know. I feel like we’re kind of all over the place. I don’t know; I just think that with home birth and hospital birth, a pro to one person could be a con to another person.
Meagan: Exactly. That’s what I’m saying. It’s so hard.
Julie: I think you hit it right exactly on the head when you said, “You’ve got to make your own pro and con list.” I’ve been looking-- if you can hear my mouse clicks in the background-- I’ve been looking for the home birth studies that have been recent. The Canadian home birth study. It’s really interesting.
I’m going to go and talk about a couple of different resources about home birth, actually. Evidence-Based Birth® wrote an article about home birth safety. Here we go. Sorry. I’m just clicking back and forth really fast. So, here’s the thing. The Evidence Based® article was written in 2012. There have been studies that have come out in 2015 and 2017 that haven’t been updated in the study yet. But she has a couple of good references and information in here that I think is important to talk about, just about home birth generally, because she sums it up in a way that would take me 30 minutes to say because you know how long-winded I am.
Now, I want to say before I go into it that ACOG does not recommend home birth for a VBAC. With that being said, me and Meagan have both had out-of-hospital births with VBAC. The reason ACOG doesn’t recommend it is because there’s not enough data on the safety of home birth for women with a prior Cesarean. There’s just no evidence to prove whether it’s safe or not, and so ACOG considers it an absolute contraindication, just having a VBAC.
However, all these studies support that if a woman is low-risk, she could be a good candidate for a home birth. Being a low-risk includes that you are pregnant with a single baby, and you’ve made an informed choice to birth at home, baby is head-down at term-- although, I would kind of disagree with that one. Breech home birth can be done safely with a provider that is trained and experienced in breech birth. And if you have a back-up plan in place. That’s actually one of the things.
At birth, as long as the baby isn’t born before the 37-week mark, the mom has no serious medical conditions like heart disease, kidney disease, blood clotting disorders, type 1 diabetes, gestational diabetes managed with insulin, preeclampsia or excessive bleeding, no placenta previa obviously, and as long as parent goes into spontaneous labor-- although I think that’s also a gray area because there are certain things you can do to nudge and encourage labor to begin that aren’t medical things.
What I think the biggest thing is, is that people think that having a home birth midwife, which-- we don’t advocate for unassisted home birth, especially for VBAC. We think it’s important for everybody to have a provider that they can trust, and that is an expert in their type of birth. However, we realize that in some areas of the country and even the world, that’s not an option for you. I’m just going to leave that right there. We can go back to referencing your intuition and the pros and cons list for that.
Homebirth midwives are actually highly educated people that have gone through extensive trainings and attended hundreds of births. I know I am a midwife student right now. I am a student midwife and-- oh my gosh, the number of requirements, courses, educational pieces and information you have to learn, and hands-on experience you have to have. You have to have a mentor that will guide you, help teach you, and educate you. It is an exhaustive process to become a practicing midwife.
Midwives have lots of supplies on hand and bring lots of things to home birth. I’m just going to go over the list because sometimes people don’t think about these things. They have a handheld Doppler to monitor the baby, sterile instruments for cutting the cord, vitamin K and eye ointment for the baby, suction devices like the squeegee-little-bulb-thing to remove mucus from the infant’s nose or mouth. Oxygen tanks too-- they are required by law to have two oxygen tanks with them and adult and infant resuscitation equipment. They are required to be trained in neonatal resuscitation and CPR. There are so many things in the birth kit.
Midwives can do interventions at birth, as well. The interventions they can do is obviously monitor baby with her Doppler, monitor a woman’s progress of labor, perform cervical exams, provide physical and emotional support during labor-- although we absolutely recommend having a doula with you because the midwife can’t do both jobs at once-- being a midwife and a doula. They can perform all the newborn exams required by the state that your OB/GYNs and nurses do in the hospital. They can suture any tears after birth; they can recognize complications and transfer a patient to the hospital if they need to. Most of the time, complications are recognized earlier than they would be in a hospital just because you have a midwife there with you 100% of the time, and they can transfer you before the situation becomes emergent. They can also administer oxygen and emergency medications. Some certified midwives can carry Pitocin, Methergine, and other things like that to help in case of an emergency or hemorrhage.
Meagan: They have a lot of holistic things too.
Julie: Yes. Yeah, a lot of herbal things.
Meagan: They have a lot of herbal and holistic things that can help you avoid having those medications--
Julie: --that decrease your chances for having those things. Yep. They can also start IVs and administer IV fluids. Like I said, it depends if you are a Certified Midwife, or a Direct-Entry Midwife, or what your accreditation is. Each state varies by law on whether or not midwives can carry certain medications. But I think another reason people are kind of hesitant about home birth is not wanting to clean up the mess. That’s what my husband said.
Meagan: Yes, it’s dirty. Yes. Dirty. yes, yes, yes.
Julie: But midwives do such a really good job cleaning up the mess. In fact, my house was cleaner after my midwives left than before I went into labor on my three home births. Isn’t that funny? I’m like, “You guys should come back.”
Meagan: I believe it, though. I know that team. I know that team. They clean very well. Yeah.
Julie: “Are you going to clean at my newborn exam? The two-day postpartum visit?” Yeah. They do all the newborn checks and screenings things as if you were at a hospital. So those are some common myths about home birth.
Meagan: Yeah. Definitely myths there for sure. I love that you were talking about-- these midwives are not just some random people off of the street. They are trained. They’re qualified. And, I also want to encourage, when you are interviewing these midwives, ask them their credentials. Ask them their experience.
Julie: And their training.
Meagan: And other training. That’s going to help you. Also, I would say one of the pros of home birth versus hospital is the type of care. Now, I don’t want to say that hospital staff gives less care, or poor care, or anything like that. It’s not what I’m saying. It’s the quality of time that is put into the care. It’s not because these providers in the hospital don’t want to. It’s because they can’t. They can’t. It’s very rare, and there are people out there, but it’s very rare for a provider to be able to sit down and spend one hour with you, and answer your questions, talk about your pregnancy, talk about how you’re doing, talk about your plans and where you’re at in this journey. It’s just unlikely for them to be able to do that.
So, that is something that is huge, that was huge for me and my decision to deliver out of the hospital. Because I loved that I could go in and ask my doctor a couple of questions in my prenatal, it felt good to have a list, take it in, ask questions, and then leave and come up with more questions. But I can’t tell you how many times it was like, “Oh, well, this doctor is downstairs at birth, so you’ll have to keep your questions until next time.” Or, I’d ask a question, and he’d look at me like, “What?”
Julie: Yeah, or they’re like, “Well, the doctor is just five minutes away, so we can call him in whenever you’re ready, or you have a question.” And then they’re like, “Well, let me go check with what your doctor has to say about that,” and it’s just harder.
Meagan: Or like, you call him. You call into the office, “Hey, I have this question.” And like you said, “Oh, let me get a hold of your doctor.” And then the nurse calls you back, not your provider. But guess what? I had a question. I sent my midwife a text message. She texted me right back. She called me. “Let’s talk about this. Hey, okay. This is what I want you to do.”
Every single time I would go into a visit, she would sit down, and we would just kickback. It was like two friends at a coffee shop; only we didn’t have a table and coffee. Do you know what I mean? It was just natural.
That’s a pro that I could say. You can’t just text your doctor. You can’t just call your doctor, and rarely if you call your doctor, you get your doctor. So that was a really big pro for me is that established, individualized care. And then, guess what? I knew exactly who was going to help me get this baby here the day that I went into labor. One of the cons in the hospital is, you just don’t know these days. Usually, providers work in a group of 5+, right? You just get who you get. You may love them, and you may not have a great relationship, or you may have never met them. For me, and especially for VBAC, I feel it is so powerful to have had that relationship with the provider the entire time.
Julie: I think with that relationship too is, you learn to have trust in your provider more, and your provider learns to have trust in you more.
Meagan: Totally.
Julie: They know your specific needs more.
Meagan: Yes.
Julie: We need to wrap it up, but I feel like this episode might be more like clearing up myths about home birth rather than the pros and cons of hospital birth.
Meagan: Yeah, maybe. Yeah.
Julie: This is the thing about hospital birth. I want to just say; we are both 100% for you choosing your birth location with confidence and a provider that you are comfortable with. At hospital birth, you are just going to have to keep your eye out for more interventions being offered to you and know what those interventions are and when or when they may or may not be necessary. That’s really, really important.
But then again, there are some homebirth midwives that are really heavy on the interventions, like with herbs and oils, and things like that. I would ask, no matter where you are, what interventions are standard when they would decide something as an emergency, and for home birth, what their transfer plan looks like, what their transfer rate is.
With that being said, a high transfer rate doesn’t necessarily mean that a midwife isn’t a good midwife; it means that they are confident in their abilities with what they can and cannot handle. They are, I would say, overly cautious and would rather transfer before things become an emergency and be in the midst of an emergency, have to transfer, and possibly endanger the health and life of mom or baby. So, yeah. Pros and cons.
Meagan: Definitely. Yeah. I would say, maybe pros and cons. That’s what this episode is more pros and cons, and just the differences.
Julie: I’ve seen really, really awesome hospital births and hospital birth providers, and I’ve seen providers with their fingers in moms’ vaginas for two hours while they push. All I want to do is scream, “Get your hands out of the mom’s vagina!” They’re like, “Oh yeah, that’s a great push. That’s another great push. That’s another great push.” And I’m like, “Oh my gosh, if they’re great pushes, then why are we still just keeping our hands in vaginas?”
Meagan: And what are we doing to the pelvic floors?
Julie: Yes. What are we doing to the pelvic floor? Then there’s other times when having some fingers in to see how and where mom is pushing can be beneficial. But homebirth midwives can do that too.
Meagan: I think it’s more guidance. Because I’ve seen it at home birth, too, I think it’s more guidance for the parent, right? So like, “Hey, do you feel this right here? “I want you to focus all your individual strength right here. And then they’re out.
Julie: Yeah. Yeah. But you don’t have to keep them in for two hours. That kills me. It kills me every time. I think I’ve got to do some processing for that.
Alright. Well, we encourage you to look at the pros and cons of both hospital birth and home birth. You can find them on our blog like we mentioned at the beginning of this episode. Also, we go way in-depth about hospital birth, home birth, and other birthing locations and providers in our prep course for parents, which you can find at thevbaclink.com/shop. So, go ahead. We highly encourage you to take our course. It’s going to make you feel more empowered and more confident in your birth choices, no matter where you end up birthing.
Closing
Would you like to be a guest on the podcast? Head over to thevbaclink.com/share and submit your story. For all things VBAC, including online and in-person VBAC classes, The VBAC Link blog, and Julie and Meagan’s bios, head over to thevbaclink.com. Congratulations on starting your journey of learning and discovery with The VBAC Link.
Wednesday Dec 23, 2020
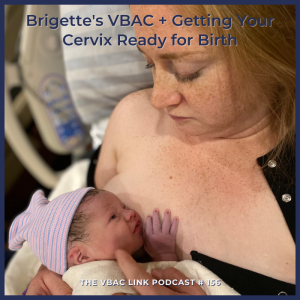
156 Brigette's VBAC + Getting Your Cervix Ready for Birth
Wednesday Dec 23, 2020
Wednesday Dec 23, 2020
Brigette, who is also one of Julie’s very own clients, shares her inspiring VBAC story of how she went from being only 1 centimeter dilated upon arrival to the hospital to 10 centimeters dilated, pushing, and a beautiful baby boy in only five hours.
In Julie’s words, Brigette’s “VBAC rocked my world. It’s one of those things where in your mind you know certain things work, line up, then the magic happens. But then, when you actually are there witnessing it and doing it, it is magical. I don’t know what other way to describe it. It’s super cool, super empowering. I left that birth all smiles, really, really excited for Brigette.”
Also, joining us today as Julie’s co-host is Tara Van Dyke, one of our VBAC Link Certified Doulas. Together, Julie and Tara discuss how to best prepare the cervix for labor, as well as some information about the cervix that most people overlook.
Additional links
Spinning Babies Abdominal Lift
How to VBAC: The Ultimate Preparation Course for Parents
Episode sponsor
This episode is sponsored by our signature course, How to VBAC: The Ultimate Preparation Course for Parents. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course. Together, Meagan and Julie have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head over to thevbaclink.com to find out more and sign up today.
Full transcript
Note: All transcripts are edited to eliminate false starts and filler words.
Julie: Welcome to The VBAC Link Podcast. This is Julie today. I am missing Meagan with all my heart, but don’t worry, because I have two wonderful people with me here today-- one of our VBAC doulas to co-host and one of my own clients sharing her VBAC story that I’m so excited to hear. I’m going to introduce both of them in just a second, but Meagan-- this is going to be really funny, the way it plays out in the schedule because this episode is coming out in the middle of our three recordings. This is technically the second one that you’re hearing with Meagan absent, but it’s three weeks after the first one that posted, and then there’s another one in two weeks that’s not going to have Meagan on it either.
So, just bear with me. I’m missing my security blanket, Meagan. But luckily I have one of our VBAC doulas and one of my clients here to fill in that warm and snuggly that Meagan always helps me with when we’re recording.
First, I’m going to introduce our co-host, Tara Van Dyke. She is in Chicago, Illinois. The only thing I know about Chicago is that the airport is really big. I had to run from one end of the terminals clear to the other ones and wait for the little tram thing to come. This was when I was in the military. It was between Basic Training and AIT I think. I had this rucksack, or not rucksack, duffel bag on my back and combat boots just hoofing it. I was in way better shape. No way I would have made it now. But like, back then. It was quite the sprint.
But Tara, her business is With U Parenting. A really fun fact about her is that she goes skydiving on all of her milestone birthdays and she takes her kid's skydiving on their 18th birthday. I think that’s the cool mom. You’re definitely the cool mom, Tara.
Tara: Thank you. I do it because I love it.
Julie: I went skydiving once when I lived in Hawaii. It was 10 years ago and it was super fun. But I’m really excited. What a fun thing to do. So, milestone birthday. What is that, like every five years?
Tara: Well, it started on my 30th. There have been a few since then, just to give you a hint.
Julie: A few?
Tara: A few, yeah.
Julie: 31 and 32.
Tara: My kids were little then and I didn’t know the side effect of them all watching me do it was that they would all be crazy about doing it, too. So, it’s been a big family tradition that I take them on their 18th birthday. All four of them have reached that milestone now, so I need to find another reason to keep going.
Julie: I’ll pretend like I’m turning 18 again, and then I’ll come to Chicago and we can go together. And Meagan, too. And maybe Brigette, later on down the road.
Tara: Totally. Yeah.
Brigette: Yes.
Julie: It will be fun. Okay, skydiving. Oh my gosh. This story is just about as exciting as the time I went skydiving. Maybe even a little bit more so. My very, very own client, Brigette. I say my favorite client, but I call all my clients my favorite client. Sooner or later they’re going to start calling me out and be like, “I’m pretty sure you called her your favorite client.”
But I really do love my clients so much. They really do get to be like my family and friends. Tara, I’m sure you can relate. It really just makes my heart happy whenever one of my clients wants to share their story.
Review of the Week
Julie: Before we get into Brigette’s story, I’m going to have Tara, the master skydiving, best mom ever, read a Review of the Week for us.
Tara: Okay, I’ve got it. There is a review from koalababy21 on Apple Podcasts and she says, “Amazing. I am so happy I found this podcast! I had a scheduled C-section with my first daughter because she was measuring large. I wish I had found this podcast before I agreed to it! Next baby, I’m definitely trying for a VBAC. This podcast has made me feel so empowered and informed. Thank you, ladies!”
I love when people are planning their VBAC before they’re pregnant.
Julie: I know. Me too. We’ve had— in fact, I think it was our very first or our very second course when we were doing in-person courses before the coronavirus. She wasn’t even pregnant yet. Her C-section baby was four months old and she came to our in-person course because she wanted to be that prepared ahead of time. And I’m like, “You rock. You rock.”
That’s definitely awesome. Yes, thank you so much for the review. We love reviews, as you know. We love hearing how we are helping you. It really keeps us going and keeps this podcast rocking and rolling for you.
Episode sponsor
Julie: Do you want a VBAC but don’t know where to start? It’s easy to feel like we need to figure it all out on our own. That’s what we used to do, and it was the loneliest and most ineffective thing we have ever done. That’s why Meagan and I created our signature course, How to VBAC: The Ultimate Preparation Course for Parents, that you can find at thevbaclink.com. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course.
Together, Meagan and I have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head on over to thevbaclink.com to find out more and sign up today. That’s thevbaclink.com. See you there.
Brigette’s story
Julie: Brigette, I had no idea. How did I not know that you met your husband in Belgium?
Brigette: Yes, technically the Netherlands, but it was on our mission. We both served a mission up there and that’s how it happened.
Julie: Oh, okay.
Brigette: Yeah. I like to get that little hook out there, you know?
Julie: Yeah, the Netherlands, and Belgium. That’s really cool. You love to travel. I love to travel too, but you know what puts a damper on that? Children.
Brigette: COVID? COVID and children.
Julie: One day. Maybe that’s what will make me the cool mom, is on their 18th birthday, I’ll take them to whatever country they want. That would be so cool, right? Actually, that would be really expensive.
Tara: It does get more expensive.
Julie: Maybe I’d better find something else. I’ve got 11 years to figure it out, so I think I’m good. But she is the wife of a former Marine and she loves cooking, baking, and taking care of her babies. She loves being outside. She has two boys-- two years old and three weeks old.
And, you guys. Her VBAC rocked my world. It’s one of those things where in your mind you know certain things work, line up, then the magic happens, but then, when you actually are there witnessing it and doing it, it is magical. I don’t know what other way to describe it. It’s just super cool, super empowering. I left that birth all smiles, really, really excited for Brigette. But before I start telling her story for her, I will turn the time over to her.
Brigette: Thank you. It’s so crazy to hear you say what you said about it. I was just excited to have you as my doula. It’s cool to be here on the podcast, and then have you talking about it like that. It’s fun being on this other side having already had the birth and I can just reflect on it now.
I have to just say, I was totally that person that before I got pregnant, I was researching all the things. After I had my first C-section, I didn’t really know what a VBAC was actually, to be honest. I didn’t know that it was a thing. I just thought I was going to have to have a C-section with all the rest of my kids and just super bummed about it, but I actually searched VBAC something, I can’t remember, on-- I think it was on Instagram, and you guys popped up. I was like, “Oh, wow. This has a lot of information.” So I just delved into it and read everything on your guys’ blog posts, and listened to all of your podcasts to and from all of my appointments, at home, on walks, and everything. So, really cool.
But anyways, to start off. I had my first C-section in 2018. It was with my first son that was born in August 2018. I had a really healthy pregnancy. I want to say that I did plan for my birth, but in all reality, I didn’t really seriously plan for it. I just kind of looked up videos and Googled things and stuff, and thought I was prepared for it.
And thought I was prepared for the hospital experience I guess I should say because no one really prepares you for that. No one tells you what it’s going to be like with doctors and nurses, and just finding a doctor that’s going to be the type of doctor that you want to help you get the birth that you want.
I totally just was-- I just went to a clinic that was in my small little town that we lived in Arizona that was close by because we were kind of far away from the big city. So I was like,” Oh sure. I’ll just go there.” They were great. They were really good. But, I think I kind of just settled with that location-wise and it turned out to be just a little bit of a bummer.
Fast forward to actually having the baby. I was 40 weeks and 1 day. I thought that I was having contractions one night. I just thought that they were building up to contractions, I should say. They were Braxton Hicks. They weren’t painful or anything, but they were kind of tight and getting a little bit intense. I laid down and they went away. I was able to sleep through the night and then the next morning my husband was like, “Let’s go on a walk. Let’s see if we can get anything going.”
So we went on a walk and walked the curb. I thought that I felt a little bit of water-- fluid coming out. I didn’t feel a gush or anything, but I was like, “Oh, I wonder if that was my water. I’ve heard that it can trickle out.” So we were like, “Okay. Let’s go home and see if more comes out.”
A little bit later, nothing happened. But I had tested positive for GBS in this pregnancy, so they were like, “As soon as you think your water broke, make sure you come to the hospital so that we can get you started on the antibiotics.” So I called the hospital and they were like, “Yeah, might as well just come in and get checked.” And so that’s what we did. We kind of took our time to get there. They checked me. I was also 2 centimeters dilated before, at my last appointment.
When I got there, they checked me. While we were waiting for the results-- we were just in triage-- all of a sudden, a ton of beeping happened and the baby’s heart rate went down. It decelerated to like 60 bpm. Everyone comes rushing in and puts oxygen on me, flipping me over, like, five times to try to get his heart rate found, or just trying to get it back to see if it went back to normal and it did after a minute or so. it went back to normal.
They permitted me and they told me that I was going to be induced that night. I was like, “Okay, sure. I am all for it. I want this baby out of me.” I didn’t really know much about the cascade of interventions.
So that was like around 3:00 p.m., and around 11:00 is when I actually got Cervidil inserted into my cervix by the doctor that was on-call. I hadn’t even met her once, to be honest. That was kind of-- yeah. She was great, but yeah. I didn’t really know her, because my other doctor wasn’t there. So as soon as she-- I just remember, as soon as she inserted the Cervidil, I swelled up down there in my lady bits. It was like golf-ball-sized swelling.
Julie: Miserable. Miserable.
Brigette: It was so painful. Yes. I couldn’t sit upright because I couldn’t sit on that, and so the birth ball was out of the picture. I couldn’t really walk around much because it hurt to walk around. So I was really just stuck on the bed, which is not ideal at all when it comes to this. You know, you want to be walking around and able to be bouncing or doing a side-lying position and I wasn’t really able to do anything to help baby come down.
Then, they put me on Pitocin, and contractions started happening. They were like, “Well, if the contractions are very intense right at the front, then we will take the Cervidil out,” and they were. It was insane. All night I was up contracting, so they eventually took the Cervidil out and I-- every single time they checked me, it was super painful and I didn’t realize why. It was just because he was super high up. Nobody really told me that.
Anyways, I just wish I would have known that. But I got checked again by a new nurse that came in and she was super gentle. It didn’t hurt when she checked me, which was strange, but I was only 3 centimeters at this point. I opted for the epidural because I think that the contractions were a minute apart and they were insane still, even though they took out the Cervidil. I was trying to breathe through them, like low and controlled breaths, but I wasn’t able to do it any longer. I was only 3 centimeters and I got an epidural.
I didn’t know what else to do. I didn’t have anyone else there to help me now. I rested the rest of the day and I took a small little nap. That night they upped my Pitocin a little bit more. Eventually, the epidural wore off and I was up the next night again, all night.
Oh, I forgot to say. Before I got the epidural, I had eaten the breakfast that they brought in. Before I got the epidural, my nurse was like, “Did you eat breakfast? Okay good, because this is the last thing you’re going to eat until after you have this baby.” I was like, “Oh my gosh.” “Yeah, also, you can’t really drink any water.” And I was like, “Okay.” I took her word for it and she was great. I really liked this nurse, but I just thought that’s how it was.
I got the Pitocin later that night, or, they upped it. I can’t remember to how much. I labored all night again and then the next morning I finally got dilated to a 10, but he was still very high up. I don’t remember what station he was at or anything. But the doctor-- they had switched shifts so there was a new doctor on shift and before she had to even come in, she heard what was happening. She hadn’t even come in to talk to me or anything and the nurses came back and they were like, “Dr. So-and-so wants you to have a C-section. She heard what was happening and she wants you to just have a C-section. She thinks it would be best.” And I was like, “Are you serious? I got this far…”
Julie: Without even coming to talk to you or see you. That’s what really bugs me. Sorry, I’m going to interrupt you for a minute. That’s one thing that really bugs me about our modern obstetric care is, we rely more on what we can see on a monitor than what a person’s body is telling us or by getting a feel for the situation by actually being present. You know? Anyways, rant over. Go on.
Brigette: No, totally. It really made me frustrated because-- just the fact that she didn’t even take the time to come in and talk to me and see how I was feeling. She was just like, “You need to have a C-section.” I told the nurses, I was like, “No. I’m going to try to have this baby vaginally. I’m going to try as long as I can. I want to push to see if I can get him to come down.” They were like, “Good. Yeah, I think that’s what you should do.”
I pushed for like an hour, and he did come down a little bit. He budged just a little bit. They could see his hair. They could see his head and stuff. My husband was able to see his head and see how much hair he had. But then the doctor came in and she was-- this part’s really annoying and frustrating too. She was standing over in the corner just kind of watching, and just looking. Not supportive whatsoever. Not even there helping me push or anything. She was just standing over there watching and she’s like, “Yeah, it looks like he’s like having some head trauma. His head looks a little red and stuff. I don’t know if you want to put him through this much longer.” And I was of course like, “I don’t want to hurt my baby.”
Of course, I don’t know if that would have been bad for him, but babies’ heads can shift I’ve learned. The plates can move around for them to come out vaginally. I just didn’t want to put him in any danger, or pain, or trauma. I prayed about it and I opted for the C-section.
The C-section was fine. I was shaking a ton, which sounds like it is pretty normal. I healed really well-- good, I guess. I don’t know. I had a good recovery with my C-section, but I still-- just the emotional aspect of it was hard for me. Every time I had a friend who had a vaginal birth-- this is probably selfish of me. But I was just like, “Why couldn’t I have had that? Why couldn’t my body have done what it was supposed to do to have this baby come out of me this way?” It was just hard. I would cry every time I thought about it for at least five months after.
Eventually, I kind of got over it and I was just like, “Okay, I’m going to have a VBAC with my next baby.” Which is what I did. But anyways...
Julie: Boom. That’s what you did. That’s right.
Brigette: So, I just kind of took notes on my phone. Everything I learned about VBACs, and prep for it and everything before I was even pregnant like I said. We moved from Arizona to Utah. We thought we were going to live here just for a little bit before we go to California for military things, but that got changed because of COVID. I was in the process of trying to find a doula and a midwife over in this area in California where we were going to move, and I wasn’t able to find anyone that was VBAC experienced or anything. That scared me, so I was really happy that we stayed here in Utah because then I got Julie. Was so great.
Julie: You had a really good doula.
Brigette: It’s funny because I had actually— what’s that?
Julie: I said, “You had a really good doula.”
Brigette: I had a really good doula, yes. I’m so glad.
Julie: Just kidding. No, but really though. I think we were a great fit.
Brigette: Yes, for sure. That’s the thing. You want to find someone who’s a great fit for you, and you were.
Actually, I messaged you guys about finding a midwife because I was-- I just didn’t even know where to start and I wanted to find a midwife. I wanted to go with a midwife this time because I had heard really good things about midwives. You guys had referred me to a midwife in Salt Lake. Am I allowed to say her name?
Julie: Yeah, you totally can. We just don’t like to bad-mouth providers, but since we really love her and I know you’re not going to say anything negative about her, then definitely. Definitely.
Brigette: Well, we love her, yes. Her name is Kira Waters. It sounds like Julie has had actually a few births with her before mine. She actually didn’t even end up being at my birth, but she was still great to be able to ask all my questions to you and then I was able to hire Julie as my doula, which I was so excited for. I keep saying that.
I really was, just because it was cool to be listening to your podcast and every time I’d listen, I’d be like, “She’s going to my birth!” Not everyone will get to have you. People are all around the world, or around the country, and I’m sure that they have great doulas too, but I was lucky to have you.
Anyway, so, fast forward to this birth, I had a good pregnancy and I had actually tested positive for GPS as well with this one, which I was really worried about, but ended up being just fine. It wasn’t that big of a deal besides that I had to be on antibiotics because my plan was just to labor as long as I could at home.
I was 38 weeks and 3 days. I had just put my son down for a nap and was taking a nap myself. I woke up to a really strong contraction right at 4:00 p.m. I was like, “Oh, I wonder if that’s just my bladder telling me I need to go to the bathroom,” because sometimes that would happen with Braxton Hicks. So, I went to the bathroom and I actually had a little bit of bloody show— may be TMI.
But, the day before, I also thought that I had lost my mucus plug and so, once I saw the bloody show, I literally looked at myself in the mirror and I was like, “My body knows what it’s doing. This is happening. I’m going to go into labor on my own,” which is what I wanted the whole time. I’m sure everyone wants that, or most people, you know?
Tara: That’s the best moment. Isn’t it? That’s awesome. It did it on its own.
Brigette: Yes. Yes, for sure. Because then you’re not-- yeah. It’s just good. So I was like, “Okay. Well, let’s just see if I have any more contractions.” I was already laying down, so I-- I don’t remember what I did after this. But anyways, I had another contraction 15 minutes later, and then it was 6 minutes later, then it was 10 minutes, and then it eventually just got more normal, like 5 minutes apart, 5 minutes apart. Then it was 4, and then 3.
Then it was 2 minutes apart and they were starting to get to where I couldn’t really talk through them. I had to stop and breathe through them. My husband had just gotten home from work and my son had woken up from his nap. We were kind of just chaos-- didn’t really know what we were doing. I was cleaning the kitchen. I had chicken on the table that was dripping off to the floor that was raw chicken because I was going to make freezer meals. I wasn’t planning on going into labor, and so I had to clean that up through all of these contractions.
So, I texted my midwife and she was like, “It sounds like it’s labor. You can go in. I would go in once you feel like you need support and help with labor.” I texted Julie and was just keeping her filled in. She was like, “Okay, I’m going to take a nap so that I am charged up to go at your birth.” I was like, “Okay, I’m not going to bug her. I’m just going to labor.” That’s what I did. Then, she texted me and she was like, “How’s it going?” I was like, “We are on our way to the hospital. I didn’t want to call you and wake you up because I knew that you were sleeping.”
She was like, “How are your contractions? Do you feel like you are having to vocalize through them?” I was like, “No, not really, but I’m definitely breathing through them really hard. Or, I don’t know. Just trying to have the controlled breathing.” You were like, “Okay. Well, I guess just let me know what you want me to do,” because-- I think you said that you could stay at your in-laws’ up there or something.
Julie: Yep.
Brigette: I just said, “Okay. I’ll let you know how it goes after the drive there,” because we had a 40-minute drive to the hospital. I was laboring in the back seat. It’s funny because right after I hung up the phone with you, all of a sudden I was like, “Okay, I can’t be quiet anymore. This is what she means. This is what vocalizing is.” My husband was like, “Okay.”
I remember at one point he was driving through that crappy Lehi traffic or whatever it’s called--
Julie: It’s awful.
Brigette: Yes. It’s so bad. It was 60, I think, that you had to go, and I was like, “I need you to go at least 70.” I looked at him in the rearview mirror and he was like, “Okay.” I was like, “You need to go faster,” just because it was going to be a long drive there.
I finally got there, and I told Julie to come to the hospital because I was like, “This is getting really, really hard. I want you to be there.” They checked me in, and I was 1, maybe 1.5 centimeters, and I was crushed. I was like, “Oh my gosh, are you kidding me? It feels like I should be at least like a 4 or a 5 right now because these contractions are on top of each other.: They were only lasting 30 seconds, but they were very strong contractions that were about 1.5 to 2 minutes apart I think.
Julie got there, and she was-- as soon as I saw her, I was relieved because it wasn’t just me and my husband in that room with the nurses knowing that I was only dilated to a 1 or whatever.
She was like, “This is what we can do. We can do abdominal lifts or we can do Walcher’s.” She explained to me what they were and abdominal lifts— I don’t know if you want to explain what they are, Julie, because you are the expert here.
Julie: Yeah. I remember I just pulled in the parking lot to the hospital when you texted me, or your husband, that you were at 1 and I was like, “She’s a 1? Like, how?” You had been working so hard and so soon as I got in, I’m like, “Alright. It’s time to get to work because something is preventing this baby from engaging,” just knowing how hard you were working.
Abdominal lifts are a Spinning Babies® technique and so, before you attempt to do them, definitely lookup on their website, spinningbabies.com, so that you can learn the proper techniques. Your pelvis has to be tucked a certain way. You have to pull a certain way. If you do it wrong, it could-- I mean I guess it could just not do anything, but it also could cause some issues if baby’s head is wonky or something like that.
But basically, you get behind the laboring person and you lift right at the very bottom of their belly. You lift upwards and then slightly backwards toward their spine. The pregnant person has their pelvis tilted in a posterior pelvic tilt, so their back is flat. That helps the baby engage, and get into the pelvis, and the cervix open, and all of those good things.
But they really suck. They’re hard.
Brigette: They were hard, but after we-- because we did 10 of them in a row, during 10 contractions I should say, but after-- I was like, “These contractions are painful anyways. I want to do something to help get him in a better position.” It was totally worth it because I got checked again, like 30 minutes later and I was 3 or 4 centimeters. We were all just like, “Yeah! This is going. Okay. Let’s do it!”
Julie: That was a great moment. Boo-yah. High-fives all around.
Brigette: Yes, for sure. Yeah. At this point, I was not able to relax at all between these contractions because they were so close together still. They were like, “Well, this is what you can do. You can get a dose of Fentanyl” or, I think that was my only option really. I was like, “Okay. I just kind of want anything at this point.” They were like, “Oh, it’s going to make you feel a little bit high, but won’t really drown out your pain at all, or very much.” Which is exactly what happened. I felt super loopy and on the bed, but I could still feel the exact pain from every contraction, so I don’t know if I would suggest that. It was a little bit of a distraction for me, so maybe that helped. I don’t know.
I was on the bed and she had me doing a side-lying position-- like where you’re laying on your side with one knee up to try to get baby in a better position, which sounds maybe comfortable, but it wasn’t at all because-- it just wasn’t my choice position for contractions. But that helped too, because then-- I can’t remember how much later it was. Not much later, probably 45 minutes I think, maybe? I was 6 or 7 centimeters dilated.
Then I was like, “Okay. I would like to get the epidural so that I can rest, so that baby doesn’t get super high heart rates or whatever.” I just needed the rest. That was my thought going into my VBAC was, I wasn’t against getting an epidural, but I wasn’t against going unmedicated. I just wanted to get my VBAC, however, that really needed to happen. If I felt like I needed to get my body rest so that it could progress more quickly, then I would opt for the epidural. That’s what I did.
I should say, my midwife wasn’t there. She was actually out of town. None of us expected me to go into labor this early, at 38 weeks and 3 days. So another midwife was there, and she was awesome. Her name was Marnae. She was just as supportive as Kira was, and wanted me to have my VBAC, and didn’t rush me to anything. She came in and brought my waters. That really helped baby come down because I could feel the pressure of his head coming down, which was cool to be able to feel that, even with the epidural.
Eventually, I got to complete. I pushed for 30 minutes and out came this beautiful baby boy. I did tear a little bit. I got a second-degree tear, but recovery has been fine. A little bit painful, but manageable for sure. I did a ton of daily birth prep from 34 to 35 weeks. Every single day, I went through my list and I think that really helped me. I don’t know if it really helped me or if I was just lucky to go into labor this soon, but yeah. That’s my story.
Tara: Yay, that’s amazing.
Brigette: I don’t know if I missed anything.
Julie: Do you know what I think is just so funny? Reflecting back on that day, it was a little bit of a crazy day for me, but I didn’t want to tell you that. I never tell clients. Even if I am really struggling with something huge, which I wasn’t that day. It was just a difficult day. But I’ll turn on heavy metal music and scream on my way to the hospital. Then, I’ll ground myself, breathe it out, and leave everything in the car, so that I can come into the birth space with a clear mind and no negative energy.
But when you were in the parking lot, I had just finished my clearing routine and I was like, “I’m okay. I’m ready to go in,” and then I got the text that you were 1 cm, I was like, “Dang it. I need to do a little more clearing.”
Brigette: More hard rock music.
Tara: What was the timeline then, from the time you got admitted until the time the baby was born?
Julie: Yeah, do you have the notes?
Brigette: It was 9:00 when I got there. It was 9, like straight up 9. He was born at 2:45-ish in the morning.
Julie: Yeah, not long at all. Girl, you dilated 10 centimeters in less than five hours.
Tara: That’s incredible.
Brigette: My first contraction was at 4:00 p.m. that day.
Tara: Yeah, but that’s when a 1 is not really a 1. You were doing good work. Your body was doing a lot more than you thought.
Julie: Yeah. Absolutely. I’m just looking back at our text messages that day because I told my husband-- huh? What was that?
Brigette: Oh, I was just saying that you had told me to do the Miles Circuit. I think that helped too during labor.
Julie: Yeah. It’s so fun. You said you had lost your mucus plug and I’m like, “Woohoo! Your body is getting ready. In my mind, I had another client and her due date was four days before you had your baby. She didn’t give birth until eight days later. It was so weird. In my mind, I am like, “There is an order to things. She’s losing her mucus plug. That’s great.” I lost my mucus plug for three weeks with my third baby.
Brigette: Your body’s getting ready. You told me that a couple of times and I was like, “Okay.”
Julie: I’m like, “Your body is getting ready. That’s really good.” Because in my mind, I’m like, “This poor mama who’s four days past her due date is definitely going to go because you’re a VBAC and your first baby didn’t come until after 40 weeks.” I was so sure, but then you said you were starting to have bloody show and contractions. I’m like, “Hey, cervical changes.”
Then you’re like, “Are you moving today?” Because that was when I moved and we had just gotten done. It was right before we moved. Yeah. So anyways, it was just so fun going through all of that. But she did. She had her baby two weeks early. It’s just so funny because you just never know when these babies are going to come. Tara, am I right?
I think my first back to back birth was with clients that were due 13 days apart and I went straight from one birth to another. It’s nuts. Tara, I just called you Tara again.
Tara: That’s okay. Yeah, that’s okay. Definitely. I’ve had clients due more than a month apart who have given birth close to the same day and vice versa. You never know. But that’s so nice when it goes earlier than you expect. That’s amazing.
Preparing your cervix for birth
Julie: Yeah. I love it. We are running out of time, but we want to talk about cervixes a little bit. Your cervix did some really cool things— or some really, I don’t know. It probably was not cool when it swelled up like a balloon in your first pregnancy.
But, cervixes are pretty cool. They are pretty amazing organs. I think we don’t give them enough credit for what they do. Why don’t you tell everyone-- I just want, straight from your mouth, what did you do? Because I know you had done some certain things to get your cervix ready so that you could have your best chances of having a vaginal birth.
Brigette: Yeah. One thing that I did-- well, I did a lot of things, but something that I definitely suggest doing is going to see a chiropractor to make sure everything‘s aligned and stuff. I really think that that helped. I was seeing a chiropractor once a week starting at 36 weeks. I know some people go more often than that. That’s what I chose to do and then I also started drinking red raspberry leaf tea. I was eating 6 to 10 dates a day. I was drinking as much water as I could. I actually was eating pineapple and the center of it. I can’t remember what it’s called. It’s like the hard part, you know? I guess it has bromelain in it or something that is supposed to help your uterus. I don’t really know. I did it.
Julie: Bromelain. I didn’t know that it helped your uterus. I think it improves digestion. I’m not quite sure actually. Never mind.
Brigette: I don’t know what it does. Yeah. I don’t know, but I was like, “Okay. Well, I’m going to try it. It’s not going to hurt me. It’s just pineapple.” And then I did the Miles Circuit every day starting at 36 weeks. Almost every day. It wasn’t every single day. I did most of these every single day.
I would do the Forward-leaning Inversion on the couch. I’d have my husband help me. Julie came over and showed me how to do it and showed him how to come up out of it. We would do that before we would go on walks at night. I would do the Forward-leaning Inversion and then make sure baby was in a good position so that when I was walking, it was helping him come down better. So we would go on walks, at least a mile, almost every day.
Then also, on my birth ball, I would sit on my birth ball for everything. Folding laundry, watching a show. Just playing with my son, my toddler, I was doing hip circles on it, and the pelvic tilts, like forward and back, and figure eights. I would do that a lot. That’s pretty much what I did. We didn’t-- this is maybe also TMI. I was not down for having sex very often, so I don’t think that was a big player of it.
Tara: I don’t think there’s any TMI on this show.
Julie: Yeah, seriously. There’s not TMI.
Brigette: True. That’s true. This is all about birth. But, yeah. Some people like, “I think I had good success with that,” but I, no. That wasn’t really on my list.
Tara: Pineapple core all the way.
Julie: Yeah. Do you know what? Sometimes, I’ve seen with my clients and Tara, maybe you can relate too, and then I’m going to have you share a little bit in just a second. Sometimes you can’t say whether it’s that certain thing that made the difference, or whether the act of just having something to do put your mind at ease or put your mind towards like, “Hey, I’m doing something that will help,” that actually gets your mind psychologically ready.
Maybe it’s both. I mean, I’m sure it’s both. There have been lots of benefits shown with the dates and the sex— obviously, semen is a prostaglandin— and the pineapple core, and all of those things. Yeah, bromelain, I think that’s the pineapple. I think that’s an ingredient in pineapple, right Tara?
Tara: Yeah, an enzyme. Yeah.
Julie: So anyways. Tara, go ahead. Your last two cents. Anything about the cervix. You can say anything about the cervix and then for anyone who is in Chicago, let them know how they can contact you because you are an awesome VBAC doula.
Tara: Well, I have a lot to say about the cervix. But I thought it was very interesting, Brigette, in your first birth, that you said those cervical checks were so painful and that partly was because the baby was high, but also it can be when your cervix is posterior. A lot of people don’t realize that the cervix starts out pointing towards our back and then it moves forward as labor progresses. It moves back and forward during our menstrual cycle too. So if they have to reach up and behind baby’s head essentially to find your cervix, way in the back, that’s super painful.
Brigette: Okay, that makes sense. I remember them telling me that too.
Tara: Yeah. So, one of the reasons that it might have been less painful that third time or whatever was because maybe it had moved forward and it was easier for the nurse to find, although sometimes there are nurses that are just really good at that— being gentle. Yeah. I think that’s really interesting about the cervix.
I love that Julie is talking about the psychology. You know, it’s doing the things, but it’s also what’s in our head about doing the things. I think that is a fascinating mix of the psychology of not trying too hard because I think when we-- when we are trying too hard, we also can work against our body‘s natural rhythms, but it sounds like what you did worked for you.
Also, being all in. You were all in.
Brigette: Yeah, for sure. I was. I was making sure that I wasn’t stressing myself out about it. I enjoy doing these things and so, just the release of oxytocin too probably helped calm my nerves. Yeah. So, anyways. I agree.
Julie: Absolutely. Well, it was so lovely to chat with you ladies today. Tara, throw down your website right now. What is the best way for people to get a hold of you?
Tara: Yes. My website is withuparenting.com and that’s U, just the letter U because it’s all about being together, being with each other. We can’t promise what’s going to happen or promise outcomes, but we can promise you won’t be alone and that you’ll have somebody with you. So, that’s the idea behind my business. My email is withuparenting@gmail.com.
Julie: I love that. That is a great sentiment. I would talk about it for longer, but since we are out of time, Tara, thank you so much for helping me co-host today and Brigette-- I just love your little family. I am so glad you are hanging around in Utah and not in California. I just appreciate both of you so much.
Tara: Thank you. Congratulations, Brigette.
Brigette: Thank you so much.
Wednesday Dec 16, 2020
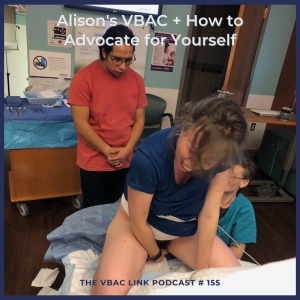
155 Alison's VBAC + How to Advocate for Yourself
Wednesday Dec 16, 2020
Wednesday Dec 16, 2020
With her first birth, Alison pushed for five hours. She was nauseous, dehydrated, and exhausted. Her doctors were adamant that she would not be able to birth her baby vaginally. Alison trusted their medical advice and went for a Cesarean.
An analyst by trade, Alison couldn’t stop analyzing every detail of that birth. She wished she had known more. She wished she had asked more questions.
When she became pregnant again, Alison knew much more, but she still had concerns and doubts. But she kept moving forward, learning and trusting her intuition.
Her second birth was fast, furious, and unique in its own way. Ultimately, she did what she knew her body was able to do.
Did you know that you have rights in the birth space? And that as scary as it sometimes feels, we have the right to ask questions?
We talk about what those rights are, what questions to ask, and how to help you feel more in control of your birth environment.
Additional links
How to VBAC: The Ultimate Preparation Course for Parents
The VBAC Link on Apple Podcasts
Episode sponsor
This episode is sponsored by our signature course, How to VBAC: The Ultimate Preparation Course for Parents. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course. Together, Meagan and Julie have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head over to thevbaclink.com to find out more and sign up today.
Full transcript
Julie: Good morning, Women of Strength. We are so excited today to have our friend Alison with us. Alison is from Philadelphia, Pennsylvania. I’ve been to Philadelphia, actually. But every time I hear the word “Philadelphia,” I don’t know. I want to see if I’m the only one. Whenever I hear the word “Philadelphia,” I want to bust out The Fresh Prince of Bel-Air song. “West Philadelphia born and raised, on the playground was where I spent most of my days, chillin’ out maxin’, relaxin’ all cool…” Right? Am I the only one?
Alison: In case you were wondering, I am actually located in West Philadelphia. I should have specified.
Julie: Fresh Prince. We’ll call you Fresh Princess Alison Grant. But seriously, now that song is going to be stuck in your head all day. You’re welcome. Let me know if you bust out singing that song every time you hear “Philadelphia” or if it’s just me. I might be the weird one.
Alright. So, Alison here from Philadelphia. She’s a mom of two. She works as an analyst, which is probably why she has analyzed everything about her births. Girl, I can totally relate to that. I am super analytical, as well. She has a lot of data around her birth like she can tell you the exact times certain things happened because she went back and looked at all of her phone records, texts, etc. and everything.
That’s really funny because I do that while I’m at births too. As a doula, I text my husband when certain things happen and that helps two things: First of all, I get timestamps, so I can make a timeline of the birth record for everybody. But also, it helps keep my husband updated so that he knows where we are at in the labor process, so he can plan his life taking care of children while I am taking care of a mom having a child.
Alright. Let’s see. We are going to talk about advocating for yourself and standing up for yourself after Alison shares her story with us. But before we do that, I’m going to read the Review of the Week because Meagan is letting a countertop guy into her house right now because we are moms, wives, doulas; we are doing kitchens, buying houses, all sorts of things right now. Life is a little bit crazy. So, I’m going to go ahead and read a review for us, and Meagan will hop on as soon as she is available.
Review of the Week
Julie: The review that I’m going to read is from erind39, and this one’s from Apple Podcasts. The title is “Essential Resource for any Woman Hoping for a VBAC.”
“I started listening to this podcast during my first trimester, in the very beginning phases of planning my VBAC. I was immediately hooked and binged all of the episodes. These amazing women gave me the confidence to find a supportive provider and reject my local hospital that has a VBAC ban.
“I felt so prepared for every barrier that I encountered because of Julie and Meagan. I felt empowered by the stories, facts, statistics, and mantras shared. Listening to these empowering stories made me confident in my ability to have the birth I hoped for. I am so happy to say that I was able to have my successful VBAC, and I feel that my ‘car doulas’ (where I always listened) were an integral part of my success. Thank you so much!!”
I’m pretty sure we’ve been called car doulas before. I really actually like that. Do you consider us your car doulas? Let us know. Go find the episode picture on our social media pages today. Let us know two things: First of all, are we your car doulas, and second of all, do you bust out the Fresh Prince of Bel-Air theme song every time you hear the word “Philadelphia” like I do?
Episode sponsor
Julie: Do you want a VBAC but don’t know where to start? It’s easy to feel like we need to figure it all out on our own. That’s what we used to do, and it was the loneliest and most ineffective thing we have ever done. That’s why Meagan and I created our signature course, How to VBAC: The Ultimate Preparation Course for Parents, that you can find at thevbaclink.com. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course.
Together, Meagan and I have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head on over to thevbaclink.com to find out more and sign up today. That’s thevbaclink.com. See you there.
Alison’s story
Julie: Alison, I want to turn the time over to you so that you have plenty of time to share your story about “birth in Philadelphia, born and raised. On the playground is where your kids spend most of their days.” I don’t know. I’m just going to stop right now. I am not a rapper. Alright. Go on. Go ahead, Alison.
Alison: Okay, yeah. So, I guess I’ll start out with my first pregnancy and birth. My first pregnancy was a pretty standard pregnancy, nothing really to highlight. I was working with a birth center. One of my biggest concerns with my first birth was that I was going to go past my due date. I knew that was pretty common. My mom went to 42 weeks with both of her kids-- me and my brother. My sister-in-law went to 41 weeks and ended up being induced, which ended up resulting in a C-section.
So, in my head, it was all about, “If labor can start on its own, I’m in a good position.” I really had a lot of my energy and focus on when labor would start and also not stressing. My assumption was, “I am going to go past 42 weeks,” or, “I’m going to go past 40 weeks,” so I didn’t expect anything to happen before then.
I really didn’t spend a lot of time and energy thinking about, “Well, once labor happens, what do I need to do? What happens then? How do I keep things moving? Because my whole focus was, “If it starts, I’ll be fine.”
I wasn’t expecting it to start when it did. My labor actually started on its due date. It was 2:00 a.m. on my due date. I woke up, and I just felt a little bit of discomfort, but I didn’t really think too much of it at the time because you’re at the end of your pregnancy. You’re just uncomfortable in general. After a couple of hours, it became clear to me that, “Okay. Maybe I’m actually having some contractions here.”
I had a prenatal appointment set up for that morning at 8:00 a.m. We pack everything up. We go to the birth center which-- by the way, on the way there, we took a Lyft to get there. The Lyft driver basically told me the story of her birth, which was a complete foreshadow of what my birth would end up being like.
Julie: Oh, my gosh!
Alison: She labored without an epidural for hours and hours and hours, had a sunny-side-up baby, and ended up with a C-section. I didn’t know at the time, but that was exactly what was going to be my birth story. We get to the birth center, and they don’t even take me for my appointment. They take me straight to a room. They checked me. I am 4-5 centimeters, but I am feeling good. I showed up not too early. I’m moving things along. I’m handling things pretty well. I spend some time in the bathtub, and really, contractions were tough. But basically, between every contraction, my husband and I are sitting there laughing and joking, so things are going really well.
Eventually, I get out of the bathtub. They check me, and I’m 9.5 centimeters. This is about nine, ten hours after I felt my first contraction, so things were moving pretty quickly for me. They offered to me— now things are also feeling a lot tougher because I’m in transition. I’m not in the bathtub anymore. They offered to me, “Do you want us to break your water? We can probably get you to 10 centimeters quicker and get started pushing.” I said, “Yes. Let’s do that.” Again, I didn’t really know what potential consequences there were around that or anything like that. So, I said, “Let’s do it. I just want to get this going.”
They break my water, and about 15 minutes later, come in and check me. I’m 10 centimeters. They said, “Let’s start pushing.” I didn’t know about fetal ejection reflex, or that I should feel an urge to push, or anything. I was just like, “Alright. They’re telling me it’s time. Let’s do it.” I had total faith in my providers to do what needed to be done. I trusted them.
So, we pull out the birthing stool, and I start trying to push. They’re telling me, “You’re pushing wrong.” Every time they check me, they tell me the baby’s not moving.
I’m severely dehydrated at this point because I haven’t drank a drop of water, basically since labor started at 2:00 a.m. I’m at a birth center, so I’m not hooked up to an IV or anything either. I’m just really dehydrated now because I was really nauseous. I couldn’t drink water. At this point, the nausea was so bad, and the contractions were so intense that I would basically push for three contractions, and then on the fourth one, there would be no pushing. I would just be throwing up.
I was so sick at this point. They gave me an IV. They get me a shot for the nausea. Things are starting to improve, but every time they checked me, they say the baby hasn’t moved at all. Still zero station. Still zero station. I’m just defeated at this point.
So, when they offered the option to me, “Let’s transfer to hospital and get you an epidural to calm down, to relax a little,” I’m like, “Yeah. Let’s do that. Please give me the epidural.” That’s all I want at this point.
I get to the hospital, and of course, you can’t get the epidural immediately. You have to get registered. The anesthesiologist has to be available, and I’m not urgent or anything. At this point in time, by the time they give me the epidural, I’ve been pushing for four hours. I’m exhausted. I’m still dehydrated, even though I’ve had three bags from the IV at this point. I’m not doing great. But as soon as I get the epidural, I really do relax. My midwife tells my husband, “You know what? Why don’t you step out of the room and get something to eat? She’s doing a lot better.”
This is where things start to get worse because while my husband is out of the room, the doctors decide to come in. There are two doctors because we’re at shift change at this point in time. They checked me, and they basically told me, “Your baby is not coming out. If your baby is going to come out, your baby is going to come out with a banana-shaped head,” which I’ve always known about coneheads—
Julie: Banana? What’s a banana head? Meagan, have you heard of that?
Meagan: Nope. I haven’t heard of a banana. I have heard of a cone-shaped head.
Julie: That’s interesting. I’m going to Google it right now.
Alison: To me, it’s like, “Oh my gosh, a banana-shaped head? That can’t be right. This is like, really not supposed to happen.” There’s apparently no way. If my baby’s going to come out, it’s wrong. That’s the message that I got from that.
I also heard my midwife and the doctor talking a little bit, and the midwife mentioned to the doctor, actually, that she thought my baby moved posterior at some point during the labor because I had no-- leading up into this, every prenatal appointment, “Your baby’s anterior. Your baby is in a great position.” But at some point during labor, my baby moved posterior, which, of course, now reflecting back, you’re like, “Okay. Well, was that when you broke my water? Did you know before you broke my water? Maybe we shouldn’t have broken my water if my baby wasn’t in a good position.” There’s a lot that I didn’t know at that point in time.
Then the doctor said to her, “Well, the baby is not posterior anymore.” The baby’s now transverse. Again, now I know. I can think back on this and be like, “Oh, my baby was rotating.” Maybe I just needed more time. My baby was on his way to being in the right position to be able to come out if, maybe, we gave it another 30 minutes. But, you have these doctors come to the room, and they’re these authority figures, and you just say, “Okay. They’re telling me this isn’t going to work. It’s not going to work. I guess I need to do a C-section.” And that’s it.
Again, this whole conversation is even happening with my husband out of the room. It just was not a good spot at all. Of course, now, I realize. It’s like-- my baby was fine. His heart rate was fine. I was doing much better. My stress levels decreased now that I had the epidural, but I just didn’t know to say, “Let’s wait,” or, “Let’s see if we can give it another 30 minutes and see what happens,” or, “Is there any other option? Can we try something else?”
I didn’t even know that once I had the epidural, I could be in other positions. I thought I was stuck lying there on my back. I just didn’t know things, so I didn’t know how to advocate for myself and how to get myself a better birth in that situation.
So, I ended up having that C-section. I’m pretty heartbroken after this because having a C-section-- not only was it the difficulty of having a C-section, but it also meant that I could no longer birth with this practice because they don’t do VBACs. I had this amazing prenatal care with these midwives, and I imagined having all of my children with them. Now, my first birth went like this, and I can never have a birth with them. I can never have that birth center birth. It was pretty upsetting for me.
When I got pregnant with my second, I’m sitting here like, “Alright. Well, where am I going to go?” So, I reach out to my local ICAN, and I ask people, “Where should I go for birth?” and they recommend to me this OBGYN/midwife practice where the midwives are supposed to be really great with VBACs, and there is an OBGYN at this practice who is really great if you decide on a repeat Cesarean for getting a family-centered Cesarean.
I’m like, “Alright. This sounds like a good practice.” They’re pretty close to me. I try them out, and I walk out of my first appointment just in tears. It was awful. The midwife basically started the appointment by telling me, “Well, a VBAC is really risky for your baby.” She’s like, “Let me pull out my phone and do the VBAC calculator.” She’s looking at the dating ultrasound and trying to push up my due date by four days, which I am like, “Okay. Wait a second. Four days is in the realm of error on a dating ultrasound.” I am someone who has gone through infertility.
I had infertility with my first and used a fertility doctor to get pregnant. With my second, I didn’t use the fertility doctor, but we were using basically every tracking method possible, so I was pretty positive about my due date. Four days on a due date maybe isn’t that much, but as you guys know, when you’re a VBAC, they are more likely to push interventions earlier on you, so four days could really matter. I just really wasn’t happy with that and immediately was again like, “Okay. Wait a second. If this is supposed to be the best practice, now where do I go? If they’re not willing to help me, who’s going to be the practice I can go with?”
So, I looked back at my ICAN group, and they did recommend another practice to me that was farther away, so I didn’t really want to go with it at first. But we went to them, and these midwives at this practice were phenomenal. Both my husband and I were like, “You know what? That first appointment was-- the whole point of that first appointment of getting that midwife who really did not treat me well was to get me out of that practice because I wasn’t meant to be there. I was meant to be with this other practice.”
How awful would it have been if every prenatal appointment was with the great midwives who were there because I’m sure there are plenty of wonderful midwives. There’s a reason that practice is recommended. But, what if I had every appointment with them and was feeling great, and then my birth is with this one? It would not have gone well. So it was meant to be, I feel like, that I had her for that very first appointment to just push me away from that practice and push me towards this other hospital that, while farther away, has really good statistics around C-sections and VBACs-- just really, a VBAC supportive hospital.
Again-- pretty standard pregnancy. Not a ton to note, really, throughout the pregnancy. I did have my focus on some different things. This time, I got a doula. I went to a chiropractor. I took a birthing class that was specific on movement and how to move a baby through your pelvis because I came in now with some prior knowledge. I didn’t have concerns about going into labor. I didn’t have concerns about dilating to 10 centimeters.
My concern was, “How am I going to push out a baby?” Because last time, I pushed for five hours. I tried tons of different positions because I didn’t have an epidural for the first four hours, and I never got the baby out. I had that messaging really in my head. Even my midwife said to me at my postpartum appointment, “You can try for a VBAC, but you couldn’t push out a 6 pound, 15-ounce baby, so you’re not really a good candidate. Because if you couldn’t push out that, what can you do?” was really just the messaging I had in my head.
Meagan: You’re like, “Yeah, but I also had a posterior baby, and there were a lot of other factors in on that. It made it harder. Not impossible, just harder.”
Alison: Exactly. Yes. You know, I was pushing before I even should have. You had me push the second I reached 10 centimeters because I was at 9.5, and 15 minutes later, I was at 10. You had me pushing the second I was at 10 centimeters. There was no time for my body to reach that point that I was ready to push. I think all that, “You’re pushing wrong,” was that my body wasn’t ready to push yet.
So, it just-- it was a lot of mental work. I did to really get myself prepared to believe in myself. But to be honest, I still had doubts coming back to me throughout the whole pregnancy and even while I was in labor. I still had doubts flooding me. When I talked to my doula after, we agreed that it was basically the last 20 minutes of labor when I realized, “Oh wait, I can actually do this.” It took me that long to really get my mind to believe in it because those doubts are there.
Like I said, it was a pretty standard pregnancy again. It was a little tough because this time, I went to 41 weeks. My first time, I literally never thought about going into labor until the moment it happened. There was no stressing about it or anxiety about it. Of course, this time, I am like, “I went earlier than I was expecting last time. Maybe I’ll be even earlier this time.” So now, I’m one of those moms who is every night thinking, “Is tonight the night? Am I going to wake up at 2:00 a.m.? I don’t know what’s happening.” There was a lot of stress around that, and of course though, I went to 41 weeks, so that went on and on.
The night that I did go into labor, same kind of thing. I just woke up to some discomfort. That was at 2:40 in the morning. My husband notices because I’m trying to relax, but nothing is really comfortable. The most comfortable thing for me was just to pace around the room. My husband notices, and I’m like, “Go back to sleep. We’re probably having a baby today, but you should just rest now. I can’t rest, but you might as well get some rest right now.” He just looked at me like I was crazy. Like, “Uh, no. I know this baby is coming. What do you need?”
We call the doula, and we agree, like, “You don’t need to come over yet, but today’s going to be the day. We just wanted to give you a heads up.” Then my husband goes and starts trying to get everything ready for going to the hospital. We did prepare more this time ahead of time, but there were still last-minute things that we had to get together and get everything into the car.
While he’s away, I call the midwife. This is at 3:30 a.m., so it hasn’t even been an hour since I woke up with discomfort. It wasn’t even timeable contractions, but it was discomfort. I let the midwife know that my contractions are every three minutes. They’re not incredibly strong, but they’re increasing rapidly in strength. They started every three minutes from the moment I woke up. They’ve been lasting a minute from the moment I woke up. My midwife was like, “Alright. You don’t sound like you’re in active labor, but you’ve been through this before. Let me know if you think you should come in.”
I felt like things were moving quickly, but I again trusted the midwife on this. I was like, “Alright. Well, you’re right. I’m not in active labor. Let’s wait a little bit.” Shortly after that, I called my doula back, and I was like, “Alright. Things are really, really getting intense really quickly for me. Can you please come over?”
Around 4:00 a.m., I realize my contractions are now two minutes apart. This is again, just slightly over an hour since I woke up, and they are already two minutes apart, lasting for a minute or more. I text my midwife again, “Things are getting faster.”
I decide to get in the shower, but it was kind of a bad idea because I had this strong desire with every contraction to just pull anything I saw with all my strength. I was really afraid that I was going to yank the spout off the tub, and then all of a sudden, my husband‘s going to be dealing with this water-spraying-everywhere problem in our house instead of getting me to the hospital. So, I’m like, “I’ve got to get out of the shower.”
I text the midwife again at 4:20, and I’m like, “We need to go.” Again, it still hasn’t even been two hours since everything started. My doula shows up at the house, and I ask my doula, “What are you thinking?” Because really in my head at this point in time, it hasn’t even been two hours, and I am losing it. These contractions are so intense at this point, and in my head, it’s like, “It’s only been two hours. I’m just really not handling this well.”
There was no way in my head that I thought that I could already be in transition at this point because it’s only two hours. I’m just thinking that I’m really not handling it. My doula ends up giving me some instructions about-- if I get the urge to push in the car, and things like that. I’m sitting here thinking, “What are you talking about? There’s no way I’m going to push in the car.” Which, of course, is what ends up happening.
My hospital is generally 45-50 minutes away. If you are in rush hour, like 75 minutes away, but thankfully, we’re going at like 5:00 a.m. on a Saturday, so we were able to get there in 35 minutes. At some point in the car ride, things really took a turn, and I just screamed, “Oh my god.”
Apparently, at that point in time, my husband stopped listening to me. He stopped hearing me completely, because the next thing I know, I said to him, “Call Nicole,” my doula, because she had said, “If things get tough in the car, let me know. You can call me. I’ll walk you through attractions.” The problem was, I didn’t have my cell phone. My husband had my cell phone, so I couldn’t call her. He stopped hearing me after I said, “Oh my god,” because, in his head, he was like, “Oh my god, what does that mean? Is the head coming out?” He literally heard nothing more that I said.
Then, I started pushing because this time, I felt the urge to push. I was like, “Oh my gosh. This is what people are talking about. This is what I didn’t feel for five hours of pushing with my first baby. I never felt this, and here I am with my second baby and three hours into labor, I am feeling this urge to push.”
We get to the hospital, and I meet my midwife. The first thing she asks is, “Okay, I want to check your cervix.” My doula immediately stepped in because my doula knew that one of my biggest things was, “I don’t want anyone to check my cervix until I’m ready to push,” because I really strongly felt last time where things went wrong is that idea of my midwife knowing I was at 10 centimeters, now it’s time to start pushing. Even if I’m not encouraged to push or even if I know mentally, “it’s not time to push,” you’re kind of already being put on a clock there. Even though I had good midwives who didn’t say, “You have to be done in two hours,” they weren’t really ready for me to be pushing for 10 hours, and then my current midwives weren’t either.
I didn’t want anyone to check me until I knew I felt that urge. Since I did, I said, “Alright. Let’s go ahead and check me.” Confirmed 10 centimeters, and then my midwife tells me I am at zero station. That’s where all these doubts come flooding back because that’s where my baby was stuck.
Julie: Oh, no!
Alison: Yeah. This doubt floods over me, and I don’t believe it’s possible. I immediately asked for the epidural because I just can’t handle this, but they kind of talked me out of the epidural. My midwife and my doula got me mentally back on track. At some point, my midwife suggested to me to push on my back, which I remember thinking, “Wait, why are we suggesting for me to be pushing on my back? Aren’t you supposed to know this isn’t a great position?” But I was like, “Alright, let’s try it.”
I think there was an idea of, because I had that strong urge to pull with my arms, that I could really pull my legs and curl with each push. That’s what we were trying to do, but I remember they asked me if I wanted a mirror. I’m like, “Yes. Yes. Please, bring a mirror. I want to see what’s going on.” They bring me this full-length mirror, and they have it, like, seven feet across the room for me. They were trying to position it, and they asked me, “Can you see? Is this the right spot? The right angle?” I just looked at them like super disappointed, and I’m like, “I’m not wearing my glasses. I can’t see anything.” Everyone in the room just cracked up, and they took the mirror away.
I ended up getting out of that on-my-back position pretty quickly because it just wasn’t working for me. I get back to the same position I had with my first, where I really wanted to be on my knees doing a squat. I remember getting to the point where the pain between the contractions was actually worse than the contractions itself because there was so much pressure on my sacrum and on my tailbone. I know they were telling me, “You’ve got to relax in between contractions,” but I didn’t want to stop pushing because every time I stopped pushing, I just felt all that pain.
Eventually, my midwife tells me to put my hand down, and I feel my baby’s head. All of a sudden, my energy shifts. That was the moment when I was like, “Oh my gosh, this is going to happen. This is real.” I started shouting to everyone, “I’m going to push a baby out of my vagina! I’m going to push a baby out of my vagina! I’m going to push a baby out of my vagina!” I was on cloud nine all of a sudden. It was great. My midwife looks at me, and she’s like, “Yeah. There’s no going back now. This is happening.”
Julie: I love that.
Alison: My doula later was like, “Yeah, that was your mantra for your birth-- I’m going to push a baby out of my vagina.” I get to a place where it’s really that moment. You’re feeling the ring of fire, and honestly, for me, the ring of fire wasn’t that bad. It was really that tailbone, sacral pain that was the worst for me.
Finally, they said, “Push.” That push where my baby’s head came out. It was just the most amazing feeling. All the pressure is gone, all this relief, like, “Oh my god, this just happened.” It was amazing. I felt the same way when I pushed out her shoulders-- just all this positive energy, and I felt so, so good.
My baby was born at 7:49 a.m., so this is basically five hours since I woke up with that discomfort. Basically, half of my labor was just pushing. Everything just happened so fast in the beginning. I’m sitting here thinking, “I am not handling things well. I should be able to handle these early contractions better,” but really, it was just-- everything moved so fast in my labor.
After my baby was born-- and again, I’m in the squatting position. I’m looking down between my legs, and I see my baby lying there. I don’t know if it was looking at my baby, or just the energy in the room shifted, but immediately knew everything was wrong. It was not right. They quickly cut the cord. They still let my husband do that; they just kind of rushed him a little bit on doing it and then took my baby over to the warmer.
They’re reassuring me. I am asking them, “What’s going on? What’s wrong with my baby? Did I do something wrong?” They’re like, “Your baby is in good hands. Let’s focus on getting your placenta out.” Eventually, a NICU doctor comes in the room and basically says, “We’re taking your baby to the NICU. She’s not breathing. We’ve been trying to give her breaths, but she’s still not breathing on her own.”
They immediately start taking my baby out of the room. The NICU doctor looks at me, and she’s like, “Wait a second, have you even seen your baby yet?” I’m like, “No, except for that quick little look between my legs before you took her off to the warmer, but I haven’t really seen her.” They actually wheel her back into the room. That made me feel so much better because I was like, “Alright. If you’re not rushing out with my baby, then it can’t be emergent, right?”
They’re taking the time to bring her back in, but it really was serious. Like I said, my baby wasn’t breathing on her own. She ended up going through-- she had what’s called hypoxic-ischemic encephalopathy or HIE. Basically, she wasn’t breathing on her own at birth. We don’t know how long, if she wasn’t getting oxygen during labor, or if it only really happened really at the very end. We don’t have a lot of information about it. I talked to my midwife a bunch after. Should I have done something differently? Was there something-- should I have just had a repeat C-section? What happened?
My midwife and the nurses all basically said, “Everything was normal in the labor. There was never a point where the fetal heart tones showed that there was a problem. Everything was normal. There just was never any indication.” Everyone in the room was shocked when this happened. It wasn’t anything. There wasn’t anyone in there all ready to take care of a baby because there was no expectation that something was going to go wrong.
What ended up happening is, my baby ended up getting what’s called a hypothermia treatment, where they basically reduced her temperature so that her body can basically focus on healing; This meant that-- not only with your C-section, where you might not get that golden hour of skin-to-skin, I wasn’t even able to pick up and hold my baby until she was five days old. I wasn’t able to breastfeed my baby until she was eight days old. I wasn’t able to take my baby home from the hospital until she was 15 days old.
It was just this crazy moment of all these dueling emotions because you’re sitting here-- I just did this really amazing thing, and I’m so excited. I’m feeling so empowered, and I did something that I never believed in myself being able to do, and then all of a sudden it’s like, but what happened to my baby? Is she okay? What are all these tests they are going to do going to say? What are the specialists going to say?
There’s all these things that they are throwing at you that, “Well, we don’t know if she can see. You’re going to have to go see an eye doctor. We don’t know what kind of delays she’s going to have. We are monitoring for seizures. We’re going to have to give her an MRI.” They are throwing all these things that you and it’s like-- I don’t have time to feel my emotions about my birth anymore.
I remember immediately after, before we knew all this information, we were just waiting to hear back. My doula, my husband, and I are sitting in the labor and delivery room just reliving everything. It was so great. We were talking about all these great moments, and all these funny moments, and then the NICU doctor comes in, and it all went away. There wasn’t any space for those emotions anymore. All I can do now is I have these questions running through my head of like, “Well, did I need to push her faster or harder? Should I not have had a VBAC?” This is one of the concerns of why a VBAC could be risky, right?
But at the same time, there was literally nothing even in my labor or pregnancy to indicate there was a problem. So, it’s a lot of work that I had to do post my birth to really accept the fact that I did what I could with the information I had in that moment. Obviously, if I knew going into it that-- if you have a C-section, this wouldn’t happen, and if you had a VBAC, this will, I would have obviously chosen a C-section for my child’s sake. But with the information I had, and even to this day, it’s still not something I know. I don’t know if we would’ve had different outcomes with a C-section because we don’t know what caused the issue. There’s just no information in her situation.
It was a really, really hard time to sit there with like, I want to feel this joy and yet I can’t, because how can I feel joy when your daughter is sitting there on morphine because the cooling treatment is bothering her so much, they have to sedate her so that she’s comfortable? How can you feel happy at that point? It was really hard. It’s been really hard to really feel those emotions of joy and happiness around this amazing birth that I did have. It really was amazing, in my opinion. So, that’s my story.
Meagan: Wow. What a crazy ride. That’s intense. I noticed something. Right after birth, you questioned what you did. You questioned your choice. I had a moment like that, too, because I had some weird blood loss stuff that really was unexplained. We really don’t even know where it went, and I was like, “Would it have been smarter, would I have been in better shape if I just would have scheduled a C-section?” I went through all of those things. I was like, “No. No. I did what I truly felt was right.”
I followed my intuition. I knew that was a birth that I needed, and yes, some things happened after, but I shouldn’t question. I feel bad because I think as VBAC birthers-- because so many people question us, if anything goes wonky, or different, and isn’t seamless-- which, let me just tell you, birth isn’t seamless. It’s very, very rare that birth happens from start to finish, and everything is perfect. I’ve been a doula for seven years, and I’ve never seen a perfect birth, right?
So, what makes me sad, though, is that as VBAC parents, we have a lot of people questioning and doubting anyway. If something happens, then it’s like, “Whoa. Whoa. Because I felt like I went through a stage where I didn’t want to tell anyone about my weird blood loss. Because I was like, “Oh, then they’re just going to tell me and be like, ‘yeah, but that wouldn’t have happened if you just would’ve had a C-section.’” You know what I mean? It makes me so frustrated that we have to go through that.
I love what you just said. Like, “Yeah. I did it, and it was okay, and this is what happened, and it was crazy, but I’m grateful, and now we’re here, and it’s awesome.” My message to a lot of people out there is, don’t let that get to you. If something weird happens, don’t put yourself down because things happen in birth.
Advocating for yourself
Meagan: We want to talk a little bit about advocating for ourselves and our rights in the birth space. This is a really touchy topic because there have been-- I mean, Julie and I have talked to tons of people over the years, even before we did this. I’ve had people say, “I feel like my rights were violated.” A long time ago, there was a colleague of ours that described her birth as that she was birth-raped, like, actually said those words. We are like “Whoa.” That is a heavy thing to feel to say that it happened to you.
So, we want to talk about the rights, because a lot of people-- I mean, not even during birth. Even during prenatal care, postpartum, and everything like that, people are having things happen to them. They are like, “Oh, I just assumed that was normal because my provider did that,” or, “I didn’t know what else to say,” or, “I was too scared to say anything,” or, “I didn’t know my place, and so I didn’t say anything,” right? I want to talk about that because really, we have a lot of rights. We really, really do. No one can make you do anything.
A birthing person can refuse any and all medical interventions regardless of the harm, even if that means it’s a life or death situation. Truly. That sounds crazy, but you really can say, “No.” They can say, “Well, you’re going to die,” and you can still say, “No.” Most people won’t say, “No,” maybe, but you literally have the ultimate choice to refuse.
Hospitals cannot force anyone to undergo any procedure or treatment without consent. Again, even if that means life or death. Depending on the stage of pregnancy, the hospital can refuse to treat a person who rejects care, which is hard because we know in the VBAC world, there are a ton of VBAC bans, so people are feeling left unsure of what to do.
We got a message this weekend saying, “I have no support. I feel like my only option is an unassisted birth,” which makes me just cringe inside. I wish that hospitals, birth centers, states in general, countries were understanding what they are making people feel forced to do. They would honestly rather turn down a parent who is wanting to have a vaginal birth and let them go-- and there are people-- this is not anything bad about unassisted. People who choose unassisted that is okay. That is their choice. We support people in their own choices. But they would rather turn them down and have them feel forced to have an unassisted birth.
Alison: I was just going to say-- now, I wasn’t turned down with my first provider I saw for my VBAC, but the way I walked out of that appointment-- that’s immediately what I was thinking. Do I need to go unassisted? Because this is supposed to be the best support out there, and I’m not feeling supported here.
Meagan: Yeah, and you’re not getting it. Exactly. It makes me cringe inside. It’s so not right.
We also have the right to ask questions about our care and inquire about all alternatives. There have been situations where I’ve seen that people had questions, and they’re like, “The provider literally said there’s no time for questions,” but then there was a half-hour of time before the C-section. It just didn’t even make sense to me.
We also have the right to get a second opinion and request different nurse care, doctor, or anything at any point. You could literally be pushing your baby out. Your baby’s crowning and something happened, and not be okay with that and say, “We are stopping. I need a new provider. You are excused.” We literally have that right. Consent forms can be signed during prenatal visits or at the hospital. Admissions do not count as ongoing consent to every procedure.
So, we’ve had-- we know people. I know Julie has known people. We’ve had people write us where they’re admitted, and they feel stuck because they’re admitted. But they don’t. They can refuse the right to any procedure done, and they can even leave.
It’s really important as Women of Strength to know that you have options and to not ever feel like you are trapped because that trapped feeling is never going to benefit you in any way. We had a podcast that she described, she felt like she was confined and in jail, and she actually felt like she was a schoolgirl letting everyone tell her what she could do. I just thought that was such an awesome way to explain it, honestly, because that is how a lot of people feel. Trapped, confined, and being told what to do in a moment where they are most vulnerable. Most vulnerable. We are so vulnerable when we are giving birth.
It’s important to know and stand up for yourself. It’s okay if it’s scary. It’s okay that it feels scary because it can be scary. But, be okay to stand up for yourself because it’s going to affect you and your future for sure. You want to be able to look back and say, “I’m glad I said something,” or, “I’m glad I asked that question.” Even if you decide to do that intervention, you don’t ever want to look back with regret.
Alison: Yeah, and I think that’s one of the big things from my first because I didn’t know to ask questions. I didn’t know to advocate for myself. I just trusted what the providers were saying and what to do. That’s why I am left with all these questions as well. Was that first C-section even necessary? Because now I’m like, my baby could have turned. I didn’t need to have my water broken. We didn’t need to rush things along. I didn’t need to push as soon as I was at 10 centimeters. There were no bad heart tones with me or my baby, nothing going wrong with us that would indicate that we needed to move to a C-section. It was just, “Well, you’ve been doing this for five hours and made no progress.” But there was progress being made. I didn’t know it was, but there was progress. My baby was rotating. That’s progress.
Meagan: Yeah, super big progress. And you know, they could have been like, “Okay, we’re going to turn to this site because your baby’s transverse to this side. Gravity will help the baby turn the rest of the way on this side.” There’s so many things that could be looked at.
You just don’t know what you don’t know sometimes. That’s where I feel like my message today is, don’t be scared to ask the questions. Even if you don’t know what the question is, be like, “Are there any other alternatives?” Do you know what I mean? You might not know about what alternatives there are specifically to say, “Well, can I try this alternative?” Ask, “What other alternatives are there? I would like to explore them. Can you break them down for me? Do you know?”
Well, thank you so much for sharing your story. We really appreciate it. We’re so glad things went well and that you have your baby to just snuggle with now.
Alison: Yeah, and I guess I didn’t necessarily conclude things for people. Luckily, my baby is doing wonderfully. There’s a lot of things that could have come as a result of this, and she is just proving everyone wrong. Things have turned around immensely, which I think has also been very healing for me.
Julie: Good.
Meagan: So good.
Julie: So glad. Alright. Well, we forgot to ask the questions on the last episode, but I wanted to ask you two questions. Let’s see. Where are we? Here we go.
What is a secret lesson or something no one really talks about that you wish you would have known ahead of time when preparing for birth?
Alison: You already touched on this a bit, but just that there is no such thing as a perfect birth. Things that sound really wonderful to you about someone else’s birth when they’re telling you their story can really, actually be very traumatic for them. To me, it might sound amazing that “Oh, you didn’t tear at all. You only pushed for 30 minutes,” because I tore, and I pushed for five hours, and then I pushed for 2.5 hours, but that doesn’t mean that their experience isn’t still hard and traumatic and it’s own way. Everyone’s experience is their own experience.
I guess that idea that you can’t really have a perfect birth. It’s really what we’ve already talked about. It’s being able to feel that you were in control as best as you could be in this crazy moment of your life.
Julie: Yeah, absolutely. I think that’s great advice. Next question:
What is your best tip for someone preparing for a VBAC?
Alison: I would say education. A lot of the ways that I had my C-section with the first was because I didn’t know to question anything, or I didn’t know that there could be risks to interventions that we get. So, education before if you can, but even in that moment of asking those questions.
Julie: Awesome. That’s great. Well, thank you so much for sharing your story with us today. We are so excited that your baby is doing well and that everyone is happy and healthy.
Closing
Would you like to be a guest on the podcast? Head over to thevbaclink.com/share and submit your story. For all things VBAC, including online and in-person VBAC classes, The VBAC Link blog, and Julie and Meagan’s bios, head over to thevbaclink.com. Congratulations on starting your journey of learning and discovery with The VBAC Link.
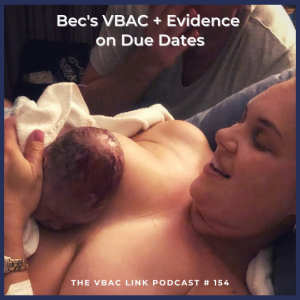
Wednesday Dec 09, 2020
154 Bec's VBAC + Evidence on Due Dates
Wednesday Dec 09, 2020
Wednesday Dec 09, 2020
Meet Bec from Sydney, Australia!
Though her first birth was very much dictated to her by hospital policies and unsupportive providers, Bec fought and researched relentlessly to make sure she was involved in every.single.decision. during her next birth. When hospital VBAC policies and outside opinions tried to prevail, Bec stayed steady and determined.
She built a birth dream team, and at the center of that team was the most important member of all—her baby.
Bec describes her journey from feeling inferior, inadequate, and controlled to becoming informed, empowered, and respected in every way. Her hard work paid off beautifully and she finally got the birth of her dreams.
We also discuss the most up-to-date evidence on due dates. Why do so many providers refuse to allow a VBAC past 39 weeks? Why do so many providers refuse to induce for a VBAC?
The most important piece of information that we want you to have during your search for a VBAC supportive provider is this:
There is no evidence to support the hard-stop deadline of giving birth at 39 weeks or 40 weeks for a VBAC.
Do not let an unsupportive provider dictate your birth. Keep fighting for that birth of your dreams, Women of Strength. You can do this!
Additional links
Evidence on: Inducing for Due Dates
VBAC After 40 Weeks: Is it Safe to Go Past Your Due Date?
How to VBAC: The Ultimate Preparation Course for Parents
Episode sponsor
This episode is sponsored by our signature course, How to VBAC: The Ultimate Preparation Course for Parents. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course. Together, Meagan and Julie have helped over 800 parents get the birth that they wanted and we are ready to help you too. Head over to thevbaclink.com to find out more and sign up today.
Full transcript
Julie: Good morning, Women of Strength. It is Wednesday, December 9th and it is a very special day for our guest today. It is her VBAC baby’s birthday, which is so exciting because-- I sent it out in an email a little while ago and I think we’ve talked about it a little bit before on the podcast, but Meagan gives me such a hard time. Not a hard time. She just teases me, or giggles, or whatever, because it always seems like whenever we air the podcast, the date has a special meaning.
Meagan: It’s without fail. It has never not happened when you are like, “Your episode will be airing on this day,” and they’re like, “Oh my gosh, it’s my anniversary!” “Oh my gosh, that’s my child’s birthday!”
Julie: “That’s my mother-in-law‘s birthday!”
Meagan: Yeah. It’s so funny how it happens.
Julie: So, Happy Birthday to VBAC baby. We’ll wait and let you decide if you want to share her name or not, but something even more exciting about our guest today is she is from Sydney, Australia.
We were chatting a little bit before the show and it’s been my dream since I was a kid, ever since I could learn to say the word “Australia”, it’s been my dream to go there. When I was growing up, I always dreamed I’d marry someone from Australia, so I could listen to their dreamy accent all day telling me that they love me. I had this huge fantasy and then I married Nick from Sandy, Utah. Don’t get me wrong. Nick has many, many, many other strengths, but he does not have an Australian accent.
So, I’m really excited to talk to Bec today. Bec is really, really just an amazing person. She lives in Sydney. She’s married to her husband, Phil. She works in PR for a motoring organization. Wait, what? Motoring?
Bec: Yeah. I think in America, you guys have the AA. It’s sort of the equivalent over here. Not Alcoholics Anonymous, the Automobile Association.
Julie: Oh, the AAA.
Bec: AAA. There we go.
Julie: Lost in translation, clear over my head. Alright. She has a hobby sewing business and makes baby stuff, like bibs and nappy wallets. She loves the beach and beers with her neighbors, “on the front steps of our homes while playing with the kids.”
And that sounds amazing. Except for me, instead of beer, it would be Red Bull or Pepsi.
Meagan: Yeah, I was going to say, Pepsi.
Review of the week
Julie: We are so excited to hear Bec’s story. But first, Meagan has a review of the week for us.
Meagan: Yes, I do. This is just a short and sweet one, but I love it. It is from Apple Podcasts and it’s from snrrrrr. Her title is, “Obsessed.”
It says, “Thank you for bringing facts to my ears as I prepare for my VBAC. I love hearing all the stories from my fellow women of strength. I feel so inspired and encouraged.”
I just love that. It’s short, sweet, and powerful. These types of reviews, as you all know, Julie and I just love. We love hearing your reviews. We love hearing what you think about it and we would love for you to tell us what you think about it, so head over to Apple Podcasts, Facebook, Google, wherever you listen to your podcast, or wherever find us, which is everywhere, and leave us a review. We would love to read it on the podcast.
Episode sponsor
Julie: Do you want a VBAC but don’t know where to start? It’s easy to feel like we need to figure it all out on our own. That’s what we used to do and it was the loneliest and most ineffective thing we have ever done. That’s why Meagan and I created our signature course, How to VBAC: The Ultimate Preparation Course for Parents, that you can find at thevbaclink.com. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course.
Together, Meagan and I have helped over 800 parents get the birth that they wanted and we are ready to help you too. Head on over to thevbaclink.com to find out more and sign up today. That’s thevbaclink.com. See you there.
Bec’s story
Julie: Alright. I am so excited for today. Bec deserves a special shout out because she is in Australia and in Utah, where we’re recording, it’s 9:30 in the morning, but in Australia, it’s 2:30 in the morning.
Meagan: We’re nice and fresh.
Julie: She literally woke up at 2:30 in the morning to come and record this session with us. I was just saying, nothing gets me out of bed at 2:30 in the morning, unless I’m getting called to a birth.
Meagan: That’s dedication.
Julie: My kids, no. My husband deals with the kids at 2:30 in the morning. Like, nothing. Earthquake-- I will stay in my house and let the ceiling fall on my head. Nothing gets me out of bed at 2:30 in the morning. So I was saying, she must really love us if she gets up so early to share her story with us.
I’m really, really excited. We’re going to talk after her story about due dates because she went to almost 42 weeks with her VBAC. I know that a lot of people have pressure from their providers to induce even before 40 weeks or to just schedule a Cesarean. We’re going to talk about that a little bit at the end.
But before we do, we are going to have Bec share her incredible story, and just sit here and swoon over her really fun Australian accent.
Meagan: I know. It’s so beautiful.
Bec: The pressure’s on. I feel like I should be a Hemsworth talking to you if you want the sweet nothings.
Julie: No, it’s beautiful. Well, we’ll channel our inner Thor vibes while we’re listening to you, but yes. You’re great.
Bec: Oh, very funny. So I guess I’ll start with my first birth. Jack was a breech baby. I found out he was breech at about 34 weeks. Everything had been quite smooth sailing up until that point.
I’m somebody who, as soon as I find out something’s going my way, I throw myself into the research. We joked that by the end of this pregnancy, I could have nearly been a breech expert. I could’ve stood up and given a lecture on the breech term trial papers, everything about the system, and why the system wants us to have a Cesarean for breech babies-- which is kind of bitterly ironic because he was a Cesarean.
I had three unsuccessful ECVs. I did handstands in the pool. I had all the smelly stuff that you’re supposed to do. I did absolutely everything I could possibly do to try to turn him. But he was, and still is-- he’s 3 1/2 now-- very stubborn, and wanted to stay wedged in my pelvis with his bum down.
My labor started pretty much on his due date and I went about a day. I went for a walk. I tried to move through contractions. It was a really uncomfortable day, but it was really manageable. That was on a Monday night. Tuesday was that manageable day.
By 6:00 p.m. on the Tuesday night, my midwife said, “Okay, I think it’s time to come into hospital. We’re just going to monitor you.” I thought, “Okay, no worries. That’s what you do.” I now know that I should’ve just stayed at home for a bit longer.
As soon as I was strapped to the bed, I felt like that was it. I wasn’t allowed to move. I had a particularly-- I don’t know how to put it politely, but a midwife on shift whose vibe just didn’t work with me. Every time I moved and tried to move through a contraction, she would say, “Get back on the bed. The monitors are going to fall off. What do you think you’re doing?” So, if the monitors did fall off, obviously, then the doctors would come in, “What’s wrong? What’s wrong?”
The silly thing was, everything was fine on the monitors. The baby was fine. I was fine. I just needed to move like a woman does in labor through those contractions to get everything going, but I felt like a caged animal. I was just being pushed back and trapped. I couldn’t do all of that. I remember saying to her, “This is just so hard. This is so hard,” after a contraction and she said, “Yeah. Well, you chose to do this.”
Words like that to a laboring woman who needs to feel very safe-- you know, for that labor to progress. No wonder it wasn’t progressing.
Meagan: Well, and feeling trapped and confined like you were. That is not going to bring a relaxed cervix. Like, a relaxed body to let the cervix open. Comments like that only makes it worse.
Bec: Exactly. I felt like a naughty, little schoolgirl. I felt like it was this flashback to sitting outside the principal’s office.
Julie: That’s so funny.
Bec: All I was trying to do was have my baby my way. My body was trying to do that, but I had these external forces pushing me, telling me, “No, no, no.”
You shouldn’t be doing what my body was trying to do. Which was really unnatural.
That was a long night. I remember my husband sleeping on the floor. I went to turn the music down and then I thought, “Wait, hang on. I am the one in labor here. Why am I turning the music down to make him comfortable?”
By about 4:00 or 5:00 a.m., I said to the midwife, “Look. Can you just give me some guidance or direction? What’s happening here?” And she gave me the most excruciating internal in the middle of a contraction and I thought, “Oh gosh, you cruel woman.” She said, “You’re not even in labor. You’re not even in labor. You’re about 4 centimeters. That’s not labor.”
Julie: Oh my gosh. How defeating. I would feel like Meagan said, “Cervix closed.”
Bec: Exactly. Exactly, and I just felt like I totally failed. I’m like, “Wow. I’ve been through all of this. It’s now been more than 24 hours and you’re telling me I’m not even in labor.” I just felt sort of stupid that I had been there and if that wasn’t labor, what was the labor? But I now know, I was in labor.
By the time the day started and the obstetrician came in-- who is the head of department who I was seeing. I was under the care of the midwives, but if anything sort of falls out of the norm, they bring in one of the obstetricians. This particular obstetrician is a really big vaginal breech birth fan. He even speaks at international conferences. He’s amazing. He’s Mr. Breech Birth, but because he was being given the information from that particular midwife-- and I don’t really know what that information was. I’d love to know.
I’d love to go back and get her out of the room, but I didn’t know you could say, “I don’t want you.” I felt like it was all being dictated to me, which is really sad looking back. So he came in and said, “Look. I’m going to recommend a Cesarean. How do you feel about that?”
I burst into tears. My husband burst into tears. He knew that my number one fear of anything happening in birth was a Cesarean. I wasn’t scared of dying, but I was scared of Cesarean, which is the gravity of the fear I had for that because I was just so determined that this was not going to be a Cesarean.
I was wheeled into the theater absolutely bawling and when I was lying there, they checked me and they said, the obstetrician said, “Oh wow, good. You’ve made it to about 6 centimeters. Well done, that’s really good.” And so I thought, again, I felt like it was the principal said that I did a good job. It was that whole sort of-- they were telling me how I was going with it, which played on me a little bit later on.
Anyway, so Jack was born. I specifically said to one of my midwives in an appointment, “I want to find out the gender first,” but nothing was written down. I said that I wanted immediate skin-to-skin, but that wasn’t written down.
When they pulled him out, a random voice said, “Here he comes. It’s a boy!” I thought, “Oh, that’s not my husband‘s voice.” But anyway, then a little baby was sort of-- a crying baby was shown to me and then taken away. I remember lying there feeling like, “Oh my god, all of this is happening to me. There’s a baby in this room. It just is a baby.”
There was no connect that that was my baby. They wiped him down, wrapped him up, and brought him over to me. I remember holding him and shaking so much from all the drugs, which a lot of people do, but just feeling a real disconnect like they just handed me a baby. I didn’t really have that immediate rush, and that bond, and everything that— I think a lot of unplanned Cesarean moms probably feel that way.
Julie: Yeah, I felt like that too. A lot of my clients do. The most important thing is just getting to hold their baby right away, first thing.
Bec: Yeah. But I wanted that slimy skin-to-skin. I wanted my baby on me, with me. As soon as they took him away, wiped him down, and started doing all the weighs and checks and measurements, that was taken away from me. You can never give a woman that back. It’s gone. To some women that’s fine, they don’t really want that, or it doesn’t matter. But for me, it was something that I really yearned for. I told them that. And it was still taken away from me. That was hard for me to get over for the years afterward, always reliving that baby over in the corner of the room.
Anyway, we had a beautiful, very healthy baby boy. Because he was breech, I had to get his hips tested at about six weeks. I took him back to the hospital and actually ran into the supervising obstetrician in a corridor and I said, “Hi. I’ve been thinking, remember in theater, you said I was about 6 centimeters? If you knew that before you gave me the spinal, would you have let me continue to labor?” And he said, “You know, we probably would have.”
Julie: Oh my goodness.
Bec: And I felt like-- yeah. I felt like my world just fell out from under me. He must have seen the look on my face and he said, “But you were very exhausted.” To try and make up for what had happened. So I lived with that for a few more years, trying to understand that, feeling so much resentment and a massive lack of control over what had happened to me.
I was determined to have a VBAC the next time. I did end up bonding very beautifully with Jack. We had a lovely breastfeeding journey. Everything‘s been wonderful.
By the time the second pregnancy came around, I was just so determined. I had started my chiro appointments really early to make sure my pelvis was in great shape, to make sure positioning would be good, to try and avoid having another breech baby if we could.
I practiced all of my HypnoBirthing breathing from the start of the pregnancy. I did a lot of yoga and Spinning Babies® exercises, meditation— I just tried to do everything to get myself in the right position and mindset for a really good, smooth pregnancy and to have a successful VBAC.
I found my hospital’s VBAC policy, staff procedures, and guidelines online. I went through all of this paperwork with a fine-tooth comb. My approach to this birth was that these are the recommendations, and I have the choice to make informed decisions based on these recommendations. I am the customer in the hospital. It’s not something that’s going to be dictated to me this time and I was very, very determined.
In the policy and guidelines for the hospital-- I did hire a doula, and she laughed because I printed it out and I wrote next to almost every single line, “No thanks. No thanks. Not for me.”
I went to the Evidence-Based Birth® website and that was such a good resource for me. I found an answer to almost every one of those guidelines that worked for me. That helped me write out my birth preferences. I took those back to that obstetrician and it took three rounds of edits before he and I were both happy with what was to be the final birth plan. He said to me, “Look, I’m okay with all of this. It’s my hypervigilant colleagues who won’t be, and I don’t know who’s going to be on shift when you come in.”
Julie: Oh my gosh.
Bec: I really respected that. I respected that he was on my side and that he was being honest about the system, but it also made me angry, because why should it take a really bad birth to become so aware, that you have to be so educated to fight the system to get what you deserve? Every woman deserves the birth that is right for them.
You shouldn’t have to have a bad birth to have a good birth.
Julie: Yes. Exactly. I agree, 100%.
Bec: Yeah. It makes me so sad that there are so many women-- you stand at the playground and every mom in the playground says, “Oh, my birth was this,” or they’ve got negative stories. You might find a very rare mom who says, “My first birth was amazing.”
It’s because we have to go through the system where it’s dictated to us, and it’s so sad, and it’s so wrong. But it’s why education is so important as well, and things like your podcast, so that we know that these are choices and that we should be making those informed decisions.
So anyway, the pregnancy was quite straightforward. My doula, Erica, who was quite amazing-- she told me the most important tool for me was my mind, and that the best way to achieve this VBAC was to labor for as long as possible at home.
At 20 weeks, I did test positive to GBS. Under the hospital policy, that meant antibiotics through a cannula on admission in labor. After my first experience, I didn’t want any cords and cables. I didn’t want the monitors. I didn’t want to be strapped like a zoo animal again.
I went and read the most recent Cochran Review, which found that no evidence exists to prove that antibiotics on admission really protects the baby from infection. I discussed that with the hospital and again, the doctor was like, “Yes, that is the most recent research and I agree with it, but hospital policy isn’t yet up-to-date with that research.” Which is, you know. It’s just another little bit of frustration.
Anyway, he took a look at my veins and he said, “Look. You’ve got big veins. They’re pretty easy to find. I think if something happens and we really need to insert a cannula, we can do it at the time.” He signed off on me not having cannulas. But again, it was only because I went and found that research to then present back to the hospital. I’m not a health professional. I am a mom. It’s not my area, whereas they should be the ones saying to me, “Hey, this is the latest research. But they don’t.”
Julie: I agree. Do you know what? I went off the other day. On our Instagram page, it was like, why does the burden of proof lie on the parents? Why is it that when you disagree with your provider that you have to be the one to show the current research and evidence-based practices? Why don’t providers have this information? And why aren’t they the ones looking it up to make sure that they are providing the right level of care? I mean, I’m sure there’s a complex answer to that. But like, it really frustrates me that the burden of proof lies on the birthing person. It’s frustrating.
Bec: Absolutely. And do you think that applies to like-- if you’ve got cancer and you go to your oncologist, you’re not going to be presenting them with the latest research. You’d feel really silly doing that. That’s why I think a lot of women would feel the same in pregnancy. Like, you’re telling the experts how to do their job and it’s a really uncomfortable thing to do. But if they can discuss it with you like this amazing obstetrician--
Anyway, my doula said, “Soak in a bath of diluted apple cider vinegar for a few days and you’ll test negative to GBS,” and I did. So that was good. I got to avoid fighting the system anyway.
Meagan: How much did you put in the bath?
Bec: I put 2 cups, or I think it was 2 cups. Maybe one cup of apple cider vinegar in a bath that was up to my belly button. So, quite diluted.
Meagan: Nice. That’s awesome.
Bec: I have no idea if it was a coincidence but hey, we got the results.
Meagan: It worked!
Bec: Exactly. Through this pregnancy, I did start to feel-- I’ve never had any mental health issues and I did start to feel-- I think the trauma from my first birth was manifesting itself in a lot of anxiety and it was really, an odd thing for me. That made it scary.
I’d be waiting on the train platform to get the train home from work and I’d have really shocking images of my son on the-- I know it’s a bit brutal. You might want to edit that out. My son wouldn’t even be with me, but I’d see him lying on the train tracks when the train would come, and things like that. It was so graphic and horrible. I would have panic attacks and break down and cry, and have to leave the train station, and think, “Oh my god, how am I going to get home?”
But things that were never going to happen, because my son wasn’t even with me. I’ve since learned they’re called intrusive thoughts and they’re really, really, really common, especially with moms. I was too scared to-- even when the baby was born, I was too scared to cross the road, because I was certain that cars were going to hit all of us and that the kids would be taken. They were unreasonable because there weren’t even cars on the road when I would be crossing. I think that all of these overwhelming thoughts in my mind and this trauma was manifesting itself in this new form of mental health that I hadn’t dealt with before.
I started seeing a psychologist who specializes in perinatal mental health and it was wonderful. She helped me so much. She gave me so many tools, but it’s something that I’m still-- to this day, I’m learning how to deal with that.
It’s something that I think is important to talk about because we don’t realize just how common mental health issues are. Again, we don’t talk about it enough, I don’t think. Women think they’re alone and they suffer alone, but really we just need to talk. Talking it out is amazing. Having a cuppo with your neighbors, having a chat with girlfriends can help so much with that. But that was a big part of this pregnancy because it was just unexpected. I’ve never had anything like that happen before.
So probably about 33 weeks, I had an unexpected bleed. I went to the toilet and went, “I’ve got my period.” And then I went, “Oh, hang on. I’m pregnant. I’m not supposed to have my period. Oh, wow.”
Meagan: You’re like, “Wait a second.”
Bec: I rang my midwife and she’s like, “Yeah. You need to come straight in.” I just bawled because I had worked so hard to have this VBAC. My mind was on one path and then all of a sudden, I got thrown this curveball.
We went in the hospital. We monitored. I stayed for a while. I stayed overnight, but they couldn’t find anything. They couldn’t find a cause. I actually think I was burning the candle at both ends. I was stressing myself out a little bit. My head had told my body to chill and I ignored it, so then my body overrode that, and then I just needed to rest. So at 33 weeks, I finished work and I went to the beach every day. It was so lovely.
This was November, December in Sydney. It was just before the bushfires started that you guys would have seen in the news last year. The beach every day was quite spooky. The sky was getting darker.
Julie: Yes. That was scary.
Bec: Yeah, it was. The day after my baby was born, I walked down into the hospital corridor and the whole corridor was like out of a movie. It was like someone had turned a smoke machine on from a party. The whole corridor was just thick smoke. It had come through the hospital air conditioning and everything. We thought that was a scary time to give birth. Little did we know, COVID was to hit a few months later.
So I would go to the beach every day, and every day I would put a little story up on Instagram. My friends would say, “Oh, you’re still pregnant.” Yep, still pregnant. I got to 37, 38, 39, 40 weeks. Yep, still pregnant. 41 weeks. Yep, still pregnant. I had people say things to me, “But why are they letting you go so long? Why haven’t they induced you yet?”
I’d say, “I don’t want to be. I feel fine. The baby will come when the baby is ready.”
“But how are they allowing you to do that?” Even my mum would say things like that. My mum would say, “What are the doctors saying? Isn’t this-- the baby’s going to be like a shriveled up little raisin. We can’t have this happen.” And I’m like, “Oh no, Mum. The baby’s fine. The baby doesn’t know the date on the calendar. The baby is okay.” But as much as I was okay with going “late”, it was the pressure around me. As much as you might say, “I’m okay with this,” it’s those little comments every single day.
“Oh, are you sick of it? Oh, that baby must be so big. Are you sure that baby is okay?” I went in for a scan at 41 weeks just to check everything was okay and the sonographer said to me, “You do realize you are seriously increasing your risk of having a stillborn by choosing to go over your dates with this pregnancy.”
Julie: I hate it when they use that. Like the statistics are there, yes. It does increase. But it increases— I mean technically you could say it doubles, but it goes from .02% to .04%, so it’s still a really, really small percent risk. But when you say it like that, “Oh, your risk of stillbirth doubles,” then it’s way scary sounding.
Bec: And also, is that a sonographer’s job? Or is that a midwife’s job to tell me that?
Julie: For real.
Bec: Yeah. I did tell my midwife. I said, “I’d like to complain about a sonographer,” because I’m going in there with all the education. I know the stats because I research everything, but a lot of women don’t. If she’s going and saying things like that to women, they’re probably leaving there petrified that the baby is not okay. It’s totally not her job to do that. To her, that was just a flippant comment and off she goes and has a cup of tea or lunch break. It doesn’t-- you know, there’s no consequences to her.
People in these jobs have to be so careful with the language that they use. Even like in my first labor, “Oh, you’re not even in labor.” Or, “You chose to do it this way.” All of those little comments can stick with you and keep niggling in your head for years.
Meagan: Oh yeah. Totally. I had that happen with my birth when my doctor was like, “Oh, I’m so glad you didn’t VBAC. You for sure would have ruptured.” So then what happened when I was going to VBAC after my two C-sections? I’m in labor and in my head, I’m hearing that. You know? It’s just, Ugh. Like you said, they say things and they probably never think about it again ever, but it sticks with us.
Bec: It’s something that keeps turning over in your mind. At about 40 weeks-- we already know that I went towards the end, but at about 40 weeks, I did go and have some Chinese foot reflexology. I said, “Could you hit all of the trigger points? I want this baby out.”
That night, I woke up to contractions and I was like, “This is it.” They were about 8 to 10 minutes apart. They were really full-on. I was listening to my HypnoBirthing tracks. I was trying to rest. I was trying to breathe. I couldn’t-- I thought, “Oh, yep. We are on.”
And then of course, by 9:00 a.m., they were gone. I thought, “What was that?”
Julie: Prodromal labor is the worst.
Bec: I just went into labor and I stopped. What the hell? Another week went past. I knew the pressure was coming from the hospital. Depending on who I saw, some of them were okay with me, but some of them were like, “You know, once you hit 40 weeks-- even though we are signed off on you going to 42, once we hit 40,” And I’m like, “Well, you’re not doing what you just signed off on by saying that are you? You’re putting that pressure on.”
So I said to my midwife, “Alright. Let’s have a talk about having a sweep,” because it’s the only type of intervention I was comfortable with, especially if that was going to help me avoid more induction pressure closer to 42 weeks. I know if I was going to be induced, then I was going down that slippery path of heading more towards another Cesarean and I was just so scared of touching anything that would go down that path. So we did a sweep, didn’t really do anything. Three days later, we did another one. It didn’t really do anything.
Then on a Saturday afternoon, I had a bit more foot reflexology. I’m like, “Well, it triggered something last time. Let’s give it another go,” and then I went for a sweep. I don’t know which one it was, but in the car on the way home, I started to feel that heavy period pain come back and it was fading in and out.
That was Saturday afternoon. By midnight, I could not sleep anymore. I was timing the contractions. They were about five minutes apart lasting about 50 seconds, so I thought, “Yep. We are on here.”
In the morning, I said to Phil, “Can you take our son to my parents’ house?” He got halfway there and realized he forgot something. He rang me in a panic, “Have you got time? Have I got time? I’ve got to turn around. I’ve got to get his bag that I forgot.” I’m like, “Oh, I think you’ve got time, I guess. I don’t know. Just hurry up and do it.”
Anyway, we did not know that the day was going to go on and on. We spent all day trying to help me move. The contractions were really paralyzing, so we thought, “We need to get it going.” But, we went for a walk. Every few steps, I’d have to stop and just hold onto a tree, hold onto my husband, hold onto people’s fences. So, this is Sunday afternoon. This has been going on now for about 24 hours.
That night, it just continued and I thought it was ramping up. I got in the shower. We had the TENS machine going. I got in the shower. Our bathroom wall is a shared wall with the neighbors and it’s the side of neighbors that we don’t know very well. I’ll never forget that night at about 10:00 p.m. bellowing like a cow, just roaring. It was a full-on zoo. There was a zoo happening in our house. And thinking, “These poor neighbors next-door must think something really freaky is going on.”
I got out of the shower and I went, “Call Erica. We’ve got to call the doula. And of course, she came over and she made me feel calm and safe.” They sort of subsided a little bit. She came over at midnight on Sunday night. She was still there the next morning. We knew that the midwives clocked on at 7:00 a.m., so we waited until 7 and called the midwives. One of them came and did a home check, and she’s like, “Yeah, you’re about 5 or 6 centimeters,” which is great because I knew I was already still at home at the point that I was lying on the operating theater table a few years earlier.
That was good, but as the day went on, they were still about five minutes apart, but they weren’t getting any closer. So by Monday afternoon, Erica said, “Okay. Let’s call in some other people. Let’s see if we can get maybe some acupuncture or-- what can you think of?” And I went, “My chiro. I remember listening to a VBAC Link podcast where a chiro did an adjustment in labor. Let’s give it a go.”
I texted my chiro. She came over and she didn’t do a lot. She did a little-- a few feels around my hips and adjustments and she said, “I think you should do some side-lying releases, the Spinning Babies® exercise.” So we did that. We laid down, and as soon as I sat up, I went, “Whoa.” This gush. My waters had broken. It was so incredible that just a little bit of feeling around recognized that there was tension in my right hip. Once we released it, labor kickstarted.
This is still Monday afternoon now and it started on Saturday afternoon. So I had been going for a long time. There was a lot of vomiting. There was a lot of—yeah. Everything else coming out of my body.
I went into hospital, and it was the most excruciating car ride-- like I know everybody says, but we got into hospital and Erica was behind us in the lift. She said she knew it was happening because she said I was just shaking. She said that involuntary shaking means you’re there which was really cool.
So we got in. My midwife said, “Would you mind? Do you want a check?” All of her language was really good, which was cool. She wasn’t telling me, “I’m going to check you.” She was, “Would you like me to?” And I said, “Yeah. I want to see how far along I am.” And she said, “Wow. You’re a good 8 centimeters.”
I had done all of that on my own at home, which I was really pleased with. So she then put some monitors on. She said, “I know you don’t want these, but we just have to see.” And I had, of course, envisioned this beautiful water birth like everyone wants, but she said, “Look. Baby’s heart rate is decelerating after contractions. If you don’t want to be hooked up to the machines, the wireless monitors are a thing that we can do, but it means you can only get into the shower and not in the bath.” I thought, “You know what? I just need that water. If I can move and if I’ve got this amazing circle of really cool supporters around me, then I don’t really care. I could be in the corridor. I don’t really care where I am. I felt so safe in this circle.”
Erica had told me, “Every time someone comes in, even in appointments before labor-- if someone comes in and makes you feel like they’ve got the wrong vibe, just stretch. Pretend you’re stretching, but put your hands up and do a circle. That’s your forcefield.”
It’s so funny because it worked and I imagined that every time. I imagined this little bubble around me and I had those protectors around me and my God, that was so different to the first time. It was so powerful to have these people around me that I loved and trusted. It was my midwife, my favorite student-midwife, my doula, and my husband. It was our team. It was the A-Team and at the center of that team was my baby. We were all there for her, which was really cool.
I was on the floor in the shower and contracting. The baby was crowning and my midwife said, “The registrar-- the doctor on duty wants to come in and make herself known to you.” I’m like, “What? What do you mean?” She said, “You can say no, but if you do, they’re going to be knocking and knocking and knocking. So, up to you.” I went, “Fine. Just let her in. Say hello, but she’s not doing anything to me, and then she can go.”
So, I’ll never forget. I’m on the floor in my zone. I look over and I see this little clicky pair of plastic heels. I look up and there’s this doctor wearing scrubs and she bent down and looked at me and she said, “I need to tell you about the risks of what you’re trying to do. A VBAC is very dangerous.”
And I kind of, I wasn’t laughing because I was in the middle of a contraction probably, but I thought, “You’re so pathetic.” She didn’t even penetrate my little forcefield that I’d visualized around me. She just-- it was like a little fly coming in that we could just shoo off and Phil said, “Not now,” really loud and really firmly. I was so proud of him because he’s not that kind of-- this was all not his zone, so it was really cool that he did that. She just sort of backed off and she went.
Meagan: That’s awesome.
Bec: It was so good. And I, I felt-- I was on the floor and I knew something was happening but I didn’t know what was happening, but I needed to get in the corner. I wanted it to be dark. I didn’t know what was going on, so I said, “Can you lower the bed onto the floor?” My midwife was like, “Okay, why?” What do you think? I don’t know? I needed to be somewhere safe that wasn’t that hard shell floor. We moved over and she’s like, “Yeah. You are ready.”
I pushed for a half an hour. I didn’t want coached pushing but I did want whatever help I could get to not tear. And so the girls would help teach me how to breathe down through each contraction and then to hold off a little bit. It was a little bit funny because every time a song changed, my midwife would say, “This is a good song to be born to.” I go, “Okay,” and the song would change and she’d go, “This is a good song to be born to.” And about the fifth time, I went, “You just say that to every song!” She goes, “Okay, yeah. I do.”
Meagan: You’re like, “Any song is a good song for this baby to be born to!”
Bec: But I knew that when my husband’s favorite songs came on, he’d squeeze my shoulder and say, “This is a good song to be born to.” And I’m like, “Not you, too!”
Anyway, Tilly was-- she did come out. She was born at a quarter to midnight on the eve of 42 weeks. She was fine. She was a beautiful little girl. Her head was out and the midwife said, “Do you want to feel her head?” which was so cool as before the head came out, putting my hand down there and feeling this little, slimy, hairy head was just such an amazing feeling because we had made it. I knew by that point we had made it and we had done it all together. We didn’t need anybody or anything else. It was really hard and it was really tough, and I went for a really long time, but I just trusted that bubble of safe people around me and we did it.
She came out. I did want to lift her out myself, but she was-- the girls said something about my cord not quite being long enough maybe, so I picked her up but they handed her to me. She was straight on me. I got my skin-to-skin and I got my slimy baby girl that I really wanted. I had requested to wait, to have that golden hour, to have all of that skin-to-skin to wait for my placenta.
We waited for the cord to stop pulsing and then after a half an hour, my midwife came back in and she said, “Hospital clock says we have to get placenta out. How do you feel about giving it a tug yourself before we give you the injection?”
I was like, “Yes.” It was so cool. So with one hand on my baby, the other hand down between my legs, I gently pulled on the tug and it was like a giant tampon string. I just pulled in and my placenta flopped out. It was so cool and it wasn’t painful. It was just-- I mean a baby had just come out. For me, the placenta was just, and I was scared of-- you know, women say, “Oh, they don’t tell you how painful it is when the placenta comes out.” It wasn’t actually. I think because I had just left it and let my body do its thing and I only just assisted a little bit with a little tug. So that was really cool.
And then I clamped the cord and I cut it myself. That was important to me.
Meagan: Oh my gosh. That’s awesome.
Bec: Yeah. It was so beautiful because to me, it signified the end of our internal connection and the start of our external connection. It was all about her and I doing that together.
We didn’t know we were having a girl. I hoped, of course, that we were having a girl because we had a boy, but she was on me for a little while and then someone said, “What is it? Have a look.” And seeing that it was a girl-- it was just so beautiful. Everything was just so lovely.
So we got there, and we got there without the system dictating it to me. It was so wonderful, but it still makes me so angry that people have to fight the system to get what they deserve.
The notes on my discharge form after Jack’s birth said that the Cesarean was due to a failure to progress. It had nothing to do with his breech positioning, but failure to progress. That labor was half the length of time as the second labor and the notes on the second labor’s discharge form say, “No complications.”
So what does that tell us about hospital clocks? Hospital policies dictating what Mother Nature can take care of herself? If we are educated and determined, then we can get what we deserve. But I know I keep saying, “You shouldn’t have to have a bad birth to get a good birth.” We know that my body just labors for a really long time. Some people are like, “Why did they let you labor for so long? Why did you want that to happen?”
Julie: Oh my gosh. Why did they let you? What do you mean let you? Oh my goodness.
Bec: Who’s they? I said, “There’s nothing wrong with that. That’s my body and that’s the way my body labors. It’s not fun. It’s pretty ordinary, but that’s the way my body does it.”
Failure to progress, for me, is something that infuriates me when women tell me, “Oh, I had to have a Cesarean because ‘failure to progress,’” I just feel sad. And I, yeah. My whole journey was very draining, but it was very much full of growth as well. I’m really passionate about people knowing that they can have that birth, not the birth that a policy or an opinion tells them that they should be having. They should be having the birth that they deserve.
So yeah, that’s my story. The VBAC rates in Australia-- they’re 12%. I was just looking this up. People use that as a reason for not having a vaginal birth, but I think of those who attempt a VBAC, 87% are successful. So when you say only 12% of women will have a VBAC, that’s not because they’re failing. It’s because it’s dictated to them that they have to. We really need to change that. That success rate of attempt at 87% is really high. That’s a really cool figure. We need to be working with that, not the 12%. So, yeah. I just feel so passionate now after going through that, that we are all so cool, aren’t we? Mother Nature‘s got it. Our bodies have got it.
Julie: Yep. That is so true. The rates are similar here in the United States actually. The VBAC rate is anywhere from 10 to 12% every year, but the studies show that only 60 to 80% of women who attempt a VBAC will be successful at that attempt. But I say that more would be successful if they had a provider that was truly supportive instead of just saying, “Okay well, we’ll have a VBAC as long as you go into labor by 40 weeks and as long as it is spontaneous because we don’t induce VBAC, and as long as—" You know, all of this list of criteria.
So I think we have probably a lot more providers in the United States that are not supportive when women make that choice, but also, just like in Australia their providers just aren’t giving them the option which is why only 10% of women will have a VBAC.
Bec: Exactly.
Evidence on due dates
Julie: So it’s just super frustrating and very can be very confusing to a parent after having a Cesarean. But what I want to do really fast before we get off the phone, is talk about due dates for VBAC.
Now, Evidence-Based Birth®, we love them. They are incredible. You can go onto evidencebasedbirth.com and find anything about anything. They have a really, really lengthy blog about due dates and induction. They talk about the ARRIVE study and several other studies that have come up about induction at 39 weeks versus spontaneous labor or inducing later on in the pregnancy.
They have a section specifically about people planning a VBAC and I’m just going to go ahead and read what she wrote here. It’s not too long, but I love it because Rebecca Decker, the owner of Evidence-Based Birth®-- her and her research team are so good at digging deeply into the studies and unveiling what the studies really say and what they mean.
I’m just going to go ahead and read this. We’re going to link to the article in the show notes, so if you are wondering how to find this article, you can just click on our show notes or you can Google “Evidence on Due Dates” and it’s just right there-- the first response to show up in Google.
And so, I’m just going to read this. She says:
“What about people who are planning a VBAC?
“Many people who are planning a vaginal birth after Cesarean (VBAC) are told they must go into labor by 39, 40, or 41 weeks or they will be required to have a repeat Cesarean or induction.
“Research has shown that only about 10% of people who reach term will spontaneously give birth by 39 weeks (Smith, 2001; Jukic et al., 2013). So, if a hospital or physician mandates repeat Cesareans for people who have not gone into labor by 39 weeks, this means that 90% of people planning a VBAC with that hospital or physician will be disqualified from having a spontaneous VBAC. Also, some hospitals and providers will not provide inductions with VBACs, which means some people who reach the required deadline will only have one option– repeat Cesarean.
“There is actually no evidence supporting hard-stop ‘must-give-birth-by-39-weeks’ or ‘give-birth-by-40-weeks’ rules for people planning a VBAC.
“In 2015, researchers looked at 12,676 people who were electively induced at 39 weeks for a VBAC, or had expectant management for a VBAC (Palatnik & Grobman, 2015).”
Expectant management, just a little side note here, means either spontaneous labor or inducing if there is a medical reason, or electively beyond the arbitrary deadline which, in this case, is 39 weeks.
“Elective induction at 39 weeks was associated with a higher chance of VBAC compared to expectant management (73.8% versus 60-62%). But there was also a higher rate of uterine rupture in the elective induction group (1.4% versus 0.4-0.6%).”
So it’s almost three times more likely a uterine rupture at 39 weeks elective induction than the expectant management group.
“For people who chose not to be induced, the risk of uterine rupture was fairly steady at 39 weeks (0.5% uterine rupture rate), to 40 weeks (0.6%), to 41 weeks (0.4%).”
So, right around there. Not a statistically significant difference in the rupture rates no matter how far you go gestationally as far as labor is spontaneous or expectant management.
“The first large meta-analysis to specifically look at the link between weeks of pregnancy and likelihood of VBAC was published in 2019 (Wu et al. 2019).”
Which is really exciting, because it’s very recent.
“It included 94 observational studies with nearly 240,000 people attempting labor for a VBAC. Interestingly, they found that gestational week at birth was not linked to having a VBAC— whether someone gave birth at 37 weeks, 39 weeks, or 41 weeks—it didn’t make a difference to whether someone had a VBAC or a Cesarean birth after Cesarean.”
Basically, what that is saying is that this huge comprehensive study shows that there’s no change in your chances of having a VBAC related to what week gestation you are, but there’s this other study that shows-- a much smaller study with a lot less people if you compare 240,000 people to 12,676 people. Significantly fewer people. It shows that elective induction at 39 weeks triples your chance of having a uterine rupture. The expectant management of labor in that group showed that there was a higher chance of VBAC success at the 39-week induction group.
But this much larger study shows that there is no difference. So I would definitely go with the larger study, just because you have 20 times the amount of people in that study, which gives you a more definitive look. It doesn’t talk about the risk of uterine rupture, though, in that larger group. So, we have those two.
Apparently, Meagan is writing a blog right now on this.
Meagan: I am writing a blog. So, by the time this enters, we too will have a blog and it will be titled “The Success Rate After 40 weeks for a VBAC”. Check it out on our blog.
Julie: Meagan, there’s a study right there.
Meagan: I know.
Julie: Go ahead and Google “Evidence on Due Dates” and scroll down. There are several studies linked. Go back and look through our blogs, go back and look on the Evidence-Based Birth® website. But this is the thing that I just want to highlight. Really important— double emphasis, bold, underline, exclamation points:
There is no evidence to support the hard-stop deadline of giving birth at 39 weeks or 40 weeks for a VBAC.
There is no evidence to support that. And, your likelihood of having a successful VBAC at 37, 38, 39, 40, 41, or even 42 weeks does not change. Your odds of having one does not change, no matter what week gestation you give, if you go into this expectant management protocol, which again, is either waiting for spontaneous labor or waiting for a medical need for induction.
So, yeah. Any questions?
Meagan: No.
Julie: We should do a live podcast one day. I wonder how we could do that, or people could just ask questions while we were recording. That would be super fun.
Meagan: That would be amazing. Yeah.
Julie: Alright. Well, Bec. We are so grateful for you and Happy Birthday to Tilly today.
Bec: As I was saying to you guys earlier, the name Matilda means “strength in battle”. So, she is a woman of strength from day one. Happy Birthday to her today.
Julie: Happy Birthday today. Alright well, we are going to let you go and snuggle your sweet little baby of strength. Although, it’s 2:30 in the morning, so you should probably just go back to bed.
Bec: It’s 3:30 now. I’m going back to bed.
Meagan: I was going to say-- it’s 3:30 now.
Closing
Would you like to be a guest on the podcast? Head over to thevbaclink.com/share and submit your story. For all things VBAC, including online and in-person VBAC classes, The VBAC Link blog, and Julie and Meagan’s bios, head over to thevbaclink.com. Congratulations on starting your journey of learning and discovery with The VBAC Link.

Wednesday Dec 02, 2020
153 Marilys' VBAC + The untold CBAC and VBAC stories
Wednesday Dec 02, 2020
Wednesday Dec 02, 2020
Calling all listeners! Whether you’re preparing for a VBAC, have already had your VBAC, had a planned or unplanned CBAC, or are a birth worker, this episode is for YOU.
Mari Vega is a powerful force in the birth world. Through her VBAC experience, Mari found her voice. Not only did she find it, but she realized that it is loud, it is confident, and it is beautiful. Mari is now on a mission to help all moms with any birth outcome feel heard, valued, and loved.
To the woman who has faced obstetric mistreatment during any birth, we see you. To the woman who is struggling with finding a VBAC supportive provider, we see you. To the woman who fought so hard for her VBAC and did everything right, yet got an unwanted CBAC, we see you. We see you, women of strength, and we love you. We are proud of you.
Also joining us this episode is one of our VBAC trained doulas, Allie Mennie, who has a true gift with words.
We have a special assignment for all of our listeners at the end of this truly impactfull episode. Tune in to find out what it is. We cannot WAIT to hear from each of you!
Topics today include:
- How to get your VBAC everything is working against you
- The importance of reporting obstetric mistreatment
- Finding the strength to share your CBAC story
- Releasing sorrow from any birth outcome to find greater joy
Additional links
Mari Vega’s website, Instagram, and Facebook pages
Alli Mennie’s website, Instagram, and Facebook pages
Email your letters to info@thevbaclink.com
Episode sponsor
This episode is sponsored by our very own Advanced VBAC Doula Certification Program. It is the most comprehensive VBAC doula training in the world perfectly packaged in an online, self-paced video course. Head over to thevbaclink.com to find out more information and sign up today.
Full transcript
Note: All transcripts are edited to eliminate false starts and filler words.
Julie: Alright, Women of Strength. It is Women of Strength Wednesday and we are here for you with a podcast with one of our newest, most favorite people in the world. Her name is Mari Vega and she’s doing a lot of really amazing things.
But before I try and talk about four things at once like I tend to do, I am going to let you guys know that Meagan is out doing some very important things right now. Lots of very important things and she could not make it on the podcast today, unfortunately. But I am very, very lucky because we have one of our VBAC trained doulas with us and her name is Allie Mennie. Is that how you say your last name?
Allie: Yep, Mennie.
Julie: Mennie. Allie Mennie. I love it. Allie Mennie with North Shore Doula in North Vancouver, British Columbia, Canada. Now let me tell you, when I first saw that she was North Shore Doula, I was thinking about North Shore Doulas in Louisiana in the United States, where we were supposed to go travel to before the coronavirus turned the world upside down. So, completely other country, completely other end of the continent. Well kind of, not really the end of the continent. You’re midway through the continent I suppose.
But guess what, Allie is really cool because she used to be an alpaca wrangler at a kids’ petting zoo in Los Angeles when she was in high school. I’ve got to tell you, I was not expecting her to say the most valuable lesson that wrangling alpacas taught her for birth work. So, I want her to share that with you. Allie, tell us about wrangling alpacas and birth work.
Allie: Yeah, I find little things that have helped me all throughout my life. I can attribute everything to something. But specifically, wrangling alpacas as a teenager was very stressful for celebrity kids’ parties in Los Angeles. Before every single event that we would put on, I’d have to walk up and bow to the alpacas, so they understood that there was no power struggle. I would bow down so my head was well under theirs and they would give me this look. I’d be like, “Alright. Don’t take a kid’s finger off today. We are on the same page. Here we go.”
But I say that it gave me very good insight into working with anesthesiologists. “I understand. You are the king in the room. I will bow to you. There is no power struggle here.”
Julie: Yes. Be submissive. That’s awesome. I grew up training horses. Very opposite-- you have to be the dominant one. You face them directly head-on and then they know that they are not supposed to approach you, because that’s a horse’s nature-- the dominant male in the group. If he stands up straight to you, then you’re not supposed to approach him until he turns his shoulder to the side.
So that’s what we would do. In part of my training, I would face forward, slowly turn my shoulder towards the horse, then have it come up to me and all of those things. It’s funny how opposite that is. That explains maybe why I have a power struggle sometimes in the birth room. Not a power struggle anyone can see, but an internal one.
Allie: You’re like, “Turn your shoulder.”
Julie: Yes. I’ll be like, “I am standing, facing you. Don’t you dare move.” Oh, just kidding. Okay well, kind of.
Anyways. I am really excited to talk to Mari Vega. Meagan and her have been working together to pick the perfect topic. I’m really sad that Meagan can’t be here today, but I’m really excited that Allie can.
Review of the week
Julie: Before we get to Mari, we are going to have Allie read a review of the week for us.
Allie: Sure thing. This one comes from Mandym826 from Apple Podcasts reviews. She says, “I am preparing for my VBAC in a few weeks and this podcast has taught me so much! I have had many fears and worries about it and the research and birth stories covered in this podcast have helped me stay focused on my goals. I hope to be contacting you, ladies, with my successful VBAC story one day soon! Thanks for all that you do!”
Julie: Oh, I love that. Okay, now my mind is going into stalker mode. That review was left in January and it is now October. What was the name of the reviewer?
Allie: MandyM826.
Julie: Okay. While Mari is talking, I am going to go look for Mandy M. in our Facebook community, see if she’s in our Facebook community, and I can stalk her to see if she had her birth, because it’s fun. I can’t have these types of things without the closure. You can’t just say you want to share your story on the podcast without me wondering if you had your VBAC, or how your birth went.
Allie: We are coming for you, Mandy.
Julie: I love it.
Episode sponsor
Julie: Birth workers, listen up. Do you want to increase your knowledge of birth after a Cesarean? We created our Advanced VBAC Doula Certification Program just for you. It is the most comprehensive VBAC doula training in the world perfectly packaged in an online, self-paced video course. This course is designed for birth workers who want to take their VBAC education to the next level so you can support parents who have had a Cesarean in the most effective ways. We have created a complete system, a step-by-step road map that shows exactly what you need to know in order to support parents birthing after a Cesarean. Head over to thevbaclink.com to find out more information and sign up today. That’s thevbaclink.com. See you there.
Mari’s story
Julie: Well, we are here today and so excited. This has been a long time coming. Mari Vega is an incredible woman. She is on a mission to support women in tapping into their intuition so that they can nurture their entire selves and experience motherhood with confidence. Her personal and professional experiences evoke a deep sense of advocacy to voice the vulnerabilities of womanhood and parenthood. As an author, coach, speaker, and podcaster, Marilys-- is that how you say it?
Mari: You’ve got it so right. Yes, go girl.
Julie: I’m practicing my accent. Marilys gives voice to the raw, vulnerable truths of motherhood and offers coaching and support for breastfeeding and VBAC mamas. Mari has a lot of resources for you on social media. On Instagram, she’s @mari_vega and on Facebook, she is Mari Vega Motherhood.
We’re going to link all of her resources in our show notes. So if you want to find her, just go ahead and scroll to the notes on this podcast episode and click on the links that you find there.
My goodness, we have had such a fun time finding a topic to talk about today on the podcast. I don’t even kind of know what this podcast episode is going to be titled yet. I’m going to name it when we’re done.
After Mari briefly shares her VBAC story with us, we are going to talk about how we handle VBAC when we feel like everybody’s working against us or everybody’s doubting us, how to cope when we don’t get a VBAC or when we have an unplanned Cesarean and why people kind of shy away from sharing that story. We are going to talk about doulas— being a doula and how to cope when your client doesn’t get her VBAC because we are so emotionally invested and want that VBAC birth for these parents almost as much as they do, and it can be really hard to process through all of those things. So, look forward to all of those things in this episode.
I’m just really excited because these are some things that I don’t necessarily have answers to myself. I’m glad that we’re going to have a discussion about all of these things. So before I keep on rambling-- I’m really hard at making the transition. I feel like I have to have a hard stop and then the other person starts talking, or else I keep on talking because silence is awkward for me. Anyways, Mari, why don’t you go ahead and share with us a little bit about your VBAC birth.
Mari: Yes, so thank you for that wonderful introduction, and Allie, I’m so excited to also get your perspective on this call. Just to quickly add to the introduction, I recently also became certified to be a chapter lead for Northern New Jersey’s ICAN organization. I share that because I’m new to that role and holding space for CBAC mamas has quickly become a big topic for me. So I’m happy that we get to have this conversation today. It feels very timely.
I guess to set the stage, I had my daughter, my first child, in 2016. I had thought it would take longer to get pregnant, so I don’t think I was emotionally ready. I was 27 years old. I had a lot of friends in their 30’s having trouble getting pregnant and so I thought it would take us a long time. I was in love. I asked my partner, “I want a baby. I don’t want to go through the whole, ‘get engaged to get married, buy a house, have a baby.’ I love you. Are you down for this or not?” And after a few months of thinking, he said, “You know what? I get why you want to try so that we’re not in a position where you’re really upset every month that you don’t get pregnant.”
I wanted it to be a surprise. I remember still being like, “Wow. I didn’t think I’d get pregnant in two months.” That was a big shocker. I don’t know why, but I just went on YouTube or the Internet and I saw a video of one woman having a natural birth and screaming in pain, a video of someone having a Cesarean-- I’ve never had surgery so that looked scary, then I saw a woman look peaceful with medication in a bed, having a baby with an epidural, and I was like, “Well, that looks like a great medium. That’s what I’ll go for.” That was honestly the extent to which I thought through what my labor and delivery could look like. I just assumed that I would have medication to not feel pain and that my baby would flow out of me, and everything would go great.
I get to the day that I’m going to give birth. My water breaks in the middle of the night and I’m having contractions every two minutes. I’m having back labor-- not that I knew any of this vocabulary at the time. I gave birth in New York City, so I was just so happy to go into labor in the middle of the night because traffic jams are just an absolute nightmare in the city. I was like, “Great. We’ll get to the hospital in no time and everything.”
I get to the hospital. They’re like, “Yeah, you’ve got your water broke. Go ahead. We’re going to admit you.” I’m like, “Give me the epidural. Give me the epidural. Can I get the epidural? I just don’t want to feel pain. I don’t like this pain. It’s too much. It’s too much.”
I get an epidural. I go to sleep. I push for two, two and a half hours and then I’m told I need a Cesarean because my daughter is not coming down, and it will take another eight hours of me pushing for her to come down.
Julie: Oh my gosh. They said that to you?
Mari: Yeah. I was pretty devastated because I had my asthma acting up. I couldn’t even get through-- you know how they ask you to push ten times? I think around breath seven I couldn’t even breathe anymore, so I couldn’t even breathe through my contractions. I was hyperventilating.
No one offered me oxygen. I look at mom videos sometimes, or their photos and they’re holding the oxygen mask and I’m like, “How is it possible that nobody offered me oxygen in a hospital?”
Like, what? I also delivered at an educational hospital. I have a lot of friends who are studying to be in the medical field and so I thought, “Well, let me be kind and let me agree that I can have students.” I had millions of students coming in, checking me. I had no idea what I was getting into and I had absolutely no privacy. I was full of fear. I was full of anxiety.
I couldn’t breathe and I was in excruciating pain because the epidural was off. I was 10 centimeters and pushing, from having had full medication to now no medication. I started crying my eyes out and I signed a waiver of release for a Cesarean and I was rolled into the operating room. I had the joy of listening to the OB teach my Cesarean birth to a bunch of students on the other side of the curtain.
Julie: Oh my gosh.
Mari: I remember it was horrific. I just remember thinking, “I’m going to die.” I remember I was-- at this point, I had vomited everything I had before getting my epidural and resting. I had probably not eaten for about almost 24 hours. I’d only had water. I was so exhausted. I was so thirsty. I vividly remember looking at my husband and saying at the time, not even having the energy to articulate to him like, “Will you spit in my mouth?” That is how thirsty I was and how low my energy was, where I generally kept thinking, “I’m not going to make it.”
I was shaking. I was cold and my arms were tied down. I kept having a very chipper, cheery college student in my ear saying, “Honey, your vitals are great. You’re not going to die.”
Fast forward to 2020, and the rate of Cesarean and the maternal mortality rate, how it keeps rising in the US. We’re a First World country and we’re number 52 or 53 in the list of countries for maternal mortality. That is absolutely irresponsible.
We are a first-world country. Why are women dying as a result of birth or pregnancy-related—or in their first year of being a mother. That’s just unacceptable. Actually, knowing the statistics and looking back at that feeling, no wonder that was so hard for me to let go of the feeling that I was going to lose my life. In that moment, that’s what it felt like.
So I share all that just to say that obstetric violence aside and obstetric bullying aside, I also just generally had that fear that I wasn’t going to make it, and so I know that this can’t be life. This is absolutely not what I want in the future.
This is a small detail that I sometimes skip over, but I think it’s important to note. I was asked in front of my two support family members that I brought-- my stepmom was with me and my husband. I was asked in front of them, “Are you being abused at home?” If that was my only opportunity to get help, they just blew it for me.
Allie: Wow.
Julie: Oh, yeah. You know what? I ended up in the ER in the middle of the night a few nights ago for a really, really horrible migraine. I went and got what they call a “migraine cocktail”. That’s the only thing that could save me at that time, but my husband was there, like two feet away from me, answering all my questions. The doctor looked at me-- you know the admittance questions, and he’s like, “Do you feel safe at home?” And I’m like, “Yeah.”
Even in my painful, migraine state, I could know that “Yeah, nobody’s going to say ‘no’ when their husband is two feet in front of them.” I mean, I do feel safe at home for the record, but I just-- yeah.
Mari: For the record, me too. Exactly. But you know, I encourage you to go back and report that because I did at my six-week post-op. I did report that back to the OB and actually, on the spot, he called the hospital teacher and said, “Immediately pull all the students and tell them what I just heard, and that they better not make that mistake again.”
Julie: Wow.
Mari: It did feel good to know that this kind of feedback is important.
Julie: Because who knows who you saved by having that educational moment.
Mari: Yeah, and there’s something about us getting to give the feedback back to the doctors, which I know is kind of what we were thinking we’ll talk about on this episode. But you know, there’s something about giving our feedback to providers whether it’s positive or constructive. These doctors need to be well-informed of how let down we are with the way that they didn’t hold space for us on our ways to VBACs.
That’s, I think, the big thing for me. I had all this rage during my pregnancy and I truly wonder looking back, how much of it was because all these doctors didn’t believe in me. Nobody wants to feel like that from their medical provider. I almost feel like if we can create a campaign to write a letter to your-- you know how they say to write a letter. You don’t need to mail it. You just release your pain. Write a letter to the OB with what they said to you because maybe they will forget the words, but people never forget the feeling-- the way you made them feel. These doctors, they need to get this feedback, and that’s how they are hopefully going to try to turn it around.
Quickly then, just a highlight of my second birth, I ended up getting pregnant two and a half years later. I had, at that time, researched ICAN. I knew the statistics and had found The VBAC Link and The Birth Hour and listened to all the stories. I knew what to do.
When I went to interview midwives, I really wanted to go with them. Financially, it wasn’t wasn’t going to work out because I have pretty awesome insurance, so it was really hard for me to try and go out of pocket and pay thousands when my insurance was going to cover basically everything. I struggled to find in their in-network providers that were supportive. I ended up going with providers that were near my house-- literally a three-minute drive. I was just like, “You know what? I’ll just stay comfortable. I have to see them so often. I’ll just stay nearby.”
From the get, I was told that I had clearly a small pelvis and that if the baby didn’t descend the first time, that my second baby would probably be bigger and probably also not descend. My first child was 8 lbs. 8 oz. and failure to descend when you’re at stage -2-- it was pretty condescending to say it was due to a small pelvis because baby wasn’t even in the birth canal. Ready to pop out-- I do know that for some women when you say for a fact, it’s because you saw it. You know what I mean?
How dare you say something like that, but anyways. He was really VBAC tolerant, not friendly. He was like, “Well, if you go into labor by your due date-- because we can’t induce you. If you go into labor by your due date and if everything goes the way. The best bet for you, I’ll let you push for one hour and then you have to get a C-section.” I was like, “What are you talking about?” So I’m like, “Alright, let me just wish for the best.”
It was Christmas Eve and I was coming for my 22 or 20-week appointment and a new provider-- because they have like, five providers. One of them, she came to me and she’s like, “Well, let’s read through your paperwork.” And so she’s like, “Is this your name?” Yes. “Is this your date of birth?” Yeah. “I see here it says you’ve elected a Cesarean.”
And I flipped out. I’m like, “I’ve literally talked about VBAC—"
Julie: Oh my gosh!
Mari: Yeah. I’m like, “Who wrote that? Did the doctor write that?” And she’s like, “Ma’am, sometimes we make mistakes. That’s the purpose of reviewing the paperwork with you.” And I was like, “Yeah, but I have said VBAC till I’m blue in the face, so for anyone to write the words ‘elective Cesarean’ in my paperwork is just plain disrespectful. I need to leave this practice. Please check my baby and get out of my face. Like I can’t. I can’t. Like I remember—"
Julie: Good for you. You know, one of my friends that’s a fellow doula-- sorry to interrupt.
Mari: Go ahead.
Julie: For her first birth, she was wheeled into the operating room, screaming that she did not want a Cesarean. Her doctor wrote on her op report that it was an elective Cesarean, that she chose it. Does that not just light your fire?
Mari: These are the types of things. These are the kinds of things. We have to go back. We have to go back and advocate for ourselves, even after the fact.
Yeah, so that made me switch providers. I spent all Christmas and New Year’s looking for a new provider. I find a new provider and I switched to that office. They’re like, “Yep. We are super VBAC friendly. We’ve got you. We’ve got you.” And I go, “Okay.”
At my 30 week appointment, they want to book my C-section, “just in case”. I said, “You know, I can understand that. I can understand that, however, I’m not booking it.” A lady still calls me and I said, “Okay, you know what? I’m comfortable with this particular date that’s six days after my due date, just because if I’m going to end up with a Cesarean, then I at least want the date to mean something to me.” That date meant something to me. It was my great grandma‘s birthday. She had passed many years ago. But I was like, “You know what? If I have to have a Cesarean, then give me until—" and it was almost 41 weeks. I was comfortable with this particular date.
Well, she has a vacation. “She’s not going to be around, so I can’t give you that date. We have to go sooner.” I was like, “Okay, sure.” I set up the appointment. I hung up. I went to an ICAN meeting and said, “When you start to assume that you’re just not going to show up to your Cesarean appointment, should I switch doctors?”
They’re like, “Yeah. You really shouldn’t just not show up. That’s a sign that you probably should switch again.” I’m like, “Yeah, but I’m 30 something weeks pregnant. My husband‘s going to think I’m crazy because my husband-- he just lets me do my thing, but his family is very much pro-Cesarean. In fact, on Christmas day, they decided to remind me that I should be selfless and get a Cesarean to not make this about myself. That was really a wonderful Christmas present. Oh gosh, they’re going to hear this and be like, “That’s not what we said.”
But anyway, ultimately at the end of the day, they had a natural birth with their first child and things didn’t go as planned. She has lived a certain life because of that with certain limitations. They’re just saying, “Why would you even risk having something go wrong in the birth canal? A C-section is clearly much easier. You can ensure your baby won’t have any trauma.”
I don’t blame them. People just assume that a baby having to go through the birth canal is traumatic. Meanwhile, that entire time your body is letting them know that something is going to happen. You don’t think it’s traumatic that you’re chilling there and then somebody just rips you out of your warmth?
Julie: Yes, yes!
Mari: You’re in mommy’s belly and you’re like, “What is going on?!”
I mean, it’s also how things are marketed. I think we’re all-- if you’re listening to this and if you’re tuning into the VBAC link if you’re a doula if you’re in the birth world, you know the marketing tactics that have gone into why people think this way. So I can’t even blame them because they have been conditioned to think this way.
Julie: Well, and that’s the thing too that I think sometimes we forget. Our family members, they love us and they want the best for us. They want the best for our babies. They think that they are coming at you from a place of love and concern, and they are. They probably are coming at you from a place of love and concern. They’re just not educated about the things that you are.
Mari: Exactly. This process alone, going for a VBAC is such an amazing process because regardless of VBAC or not, at the end of the day you advocated for yourself. You educated yourself. You did all the things. You left your comfort zone. You fought a doctor. You discussed it with family members.
All these things help you grow and help you become resilient. At the end of the day the process in itself-- I wish I didn’t have to be this way. I think we’re all in our own ways working to change that, but it is a process that did help me grow a lot in my life and it’s probably one of the most resilient stories I could ever tell.
I guess just to wrap that up, I did go to an ICAN meeting. It happened to be a very popular meeting that day. We had like 10 or 12 women and usually, we only had like 3 or 4. It was all of us in the room. Some of them were on their second VBAC, third baby, fourth baby. It was so empowering. I left and the next day, I called the best provider in the area known for taking women-- allowing them to switch super late in their pregnancies. It was a midwife. Something had changed, where it was later in the year so I had met my deductible and they could take me without charging me more. Everything just worked out.
I let them call the provider and break up with them for me. The provider called me and said, “Oh my gosh, are you leaving us because we scheduled you your Cesarean?” And I’m like, “Yeah.” They’re like, “Well, we can just cancel it.” And I was like, “That’s not the point.”
Allie: That’s not the point. Exactly.
Mari: “You showed your colors. That’s not the point.” Are you serious? They tried to keep me, you guys. How crazy is that?
Julie: People don’t realize that they don’t have to have that conversation with their provider. Their new provider can just call and get the records from them. They don’t even have to talk to them.
Mari: FYI, exactly. All you’ve got to do is sign a release form. They send that release form and it shows right there in black ink, “Send me my forms. I’m breaking up with you.” So that was nice.
I ended up going into labor the same way as my first labor. In the middle of the night, my water broke. I Immediately started having back labor again— back labor meaning, I didn’t have contractions in my belly. It was all in my back as if someone was breaking an ax on my back. But this time I still went in the shower. I was doing goddess pose with the shower hot water on my back. I had essential oils. I had my HypnoBirthing music.
I brought the yoga ball into the shower. Yeah, that was not a good idea, I actually fell off of it. It was very painful. I was bouncing on it, the water shifted, and I bounced down, which, I can’t even believe I did that and survived. I’m in there the whole time. I call my doula. She comes. My husband takes my daughter to someone who is going to watch her for us. I’m begging to go to the hospital because I am like, “I’m not going to make it. I’m going to the epidural. Sorry guys, I’m going to need the epidural. This back labor is crazy. Let’s go to the hospital.”
We go to the hospital around 8:00 a.m. When we get to the hospital, I’m about 4 centimeters and I wanted to be 5. Last time I was 3 centimeters. I was like, “Okay well, at least I know that I am progressing, so I’m proud of myself.”
I know the epidural will take time, so at least I know that the epidural is coming because my contractions are too much right now. I’m in the hospital. It takes two hours to get the epidural. When they come to give me the epidural, I’m 7 centimeters and I’m like, “Oh my god. I am progressing. Thank goodness.”
So I’m 7 centimeters. I take the epidural. Of course, it slows things down, but I’m using a peanut ball. I’m taking a nap and I’m switching-- I am in goddess pose on the bed, and all this stuff.
When it’s time to push, I make a fear-based decision. I want to highlight that fear-based decisions have no place in your birth. You need to leave the fear at the door. You need to process the fear during your pregnancy and face it all, because right when it was time to push and I felt all the pressure, I hit the epidural button. It hit me so much medicine that it paused my birth for three hours. I couldn’t feel anything. I couldn’t feel anything, so I couldn’t push.
They talked to me and we hung out until I got the urge to push and felt something again. Then, for three hours, my son was in my pelvis. While I could touch his hair, I couldn’t push him out. For three hours. Luckily, I learned later on, that when you touch a baby’s head, it calms their heartbeat. It can help keep them calm. So, I was touching his head to motivate myself to push harder, but thank goodness for three hours, he was my little champ. His heart was just perfect. It never decelerated. They were calm letting me keep trying.
I had a full, women staff. It just happened to be that everybody was a woman that day. The woman OB on the clock comes in and she’s like, “I’m giving her 15 minutes, and then she needs to get a Cesarean.” I’ve never met this woman and I’m like, “Oh my god.”
My midwives have been texting the back-up doctor. She’s somewhere else trying to rush over to me because she’s willing to assist me. Because the midwives can’t step in and do-- what they wanted to do to me, was an episiotomy and a vacuum-assist.
People feel very different ways. There are different, varying opinions about that. I was comfortable with the research that I did that if I needed to do that, I’d be comfortable with it. Ultimately, she flew in, literally five minutes before they were going to pull me into the OR. She was like, “Alright mama. Do you consent?”
I want to say this very clearly. She asked for my consent.
I said, “Yes. I consent to an episiotomy and a vacuum-assist.” Five pushes later, my son was here.
When I pulled my son up-- by the way there was meconium. They knew that there might be meconium. But when I pulled my son up-- so many women talk about that moment. I cry every single birth story I listen to. I listened to like, every VBAC Link story and every Birth Hour story. I always cried when they’re like, “I pulled my baby,” and I thought, “To this day, I don’t remember that moment.” I just remember, “I did it. I effing did it. I effing did it. F all those doctors who said I couldn’t do it.” That’s all I was saying in the hospital room. That’s all I was thinking.
They take my baby and they’re checking him. I asked somebody, probably my doula, “Can I get my phone?” And I decide-- this is 15 minutes after. I’m delivering my placenta and they’re stitching me up. I decide to take a video because I never wanted to forget that moment in my life. I decided to take a video. It’s a 15-second video and it’s basically just me, cursing at the doctors the whole time being like, “I told you, I could I effing do it. I am so effing proud of myself.”
Julie: Did you put that on Instagram in your stories? I am pretty sure we’ve heard it. I have seen that video. Is that how we met?
Mari: That is how we met. So, yes.
Julie: Oh, I love it.
Allie: I love that.
Mari: I think we will definitely share this video.
Julie: Yeah. I’m pretty sure we need to re-post or upload to our IGTV, or your IGTV. It’s probably on yours. Oh gosh, yes.
Mari: Oh my god, I know. It was amazing. A few months postpartum I decided to post just 5 seconds of me cursing instead of 15 seconds of me cursing, but I posted it. It blew up. I got so much support from women all over. January Harshe was in the comments defending me. Women, who are like, “Ew, why she cursing?” She was like, “That’s what you feel like!”
Julie: Exactly!
Mari: I was like, “Oh my gosh! I literally feel so good right now.” She’s a goddess! I was fangirling. You guys were shouting me out. Birth Hour was shouting me out. I was like, “Oh my god, I made it. I made it in the birth world! People know my VBAC story.” To this day, I still get DM‘s from having that full story on The Birth Hour.
That’s my story. Honestly, I think a lot about that moment. I’ve deemed myself a VBAC unicorn, so I created #VBACUnicorns to help us unite as women of strength who got through such a difficult experience. I want to celebrate being the unicorn that the doctors told us we couldn’t be.
Julie: I love it. I love it so much. I love the VBAC unicorn but also, it makes me feel sad. Let me explain though because it’s sad that it has to be such a rare thing. Such a thing that people don’t believe in, and such a thing that you’re looked at like some special creature after you have your VBAC. It’s amazing. It’s such a good feeling. You triumph and you have this victory over these providers, the naysayers, and your family or friends maybe who didn’t support you, and that’s a really powerful feeling, but it’s sad that it has to be that way. I don’t know. I just—does that make sense?
The unheard CBAC mom
Mari: Oh, absolutely. It makes sense. It’s even sadder when you are advocating and helping women on their way to their VBAC and then when they end up having a Cesarean for one reason or another, it creates this distance between women who were on a journey together and suddenly, “my journey veered right and yours veered left.” There are all of these unsaid feelings and emotions around that.
I want it to be made very clear that if you’re listening to this and you end up having a CBAC or you’re listening to this because you had a CBAC, I want you to know, when you don’t get your VBAC, a Cesarean is not a reflection of how hard you worked, or whether you did the right thing or the wrong thing. You don’t need to have done anything wrong to have a Cesarean. Your body did not fail you. Use your “best friend voice” with yourself. You wouldn’t tell your best friend, “Your body is a failure. You failed.” So don’t use that terminology with yourself.
Julie: I think that’s really important. When I first became a doula, I thought I knew everything. Just like when, with my first pregnancy, going into my first birth. I thought I knew everything. I was so confident and I was like, “Yes. I am here to rule the world. I was made to do this.”
The more births I’ve been to, the more I realize that I am never done learning. Every birth that I go to teaches me something. One thing that I have learned is that a lot of birth is preparation and intuition, but a lot of it is also luck. Sometimes luck is not on your side and something happens. Sometimes it’s easy to see and we have answers. We can say, “Oh my gosh, yes. That’s what happened and that’s why I needed a Cesarean.”
Sometimes there are no answers. Sometimes it’s just bad luck and you have zero control over that. It’s really, really a hard place to be in when you did everything you possibly could or everything you even knew to do, and still end up with a repeat Cesarean.
I really want to segue into all of the things right now, but I’m not quite sure where I want to take this. Let’s talk about the CBAC mom and the unheard CBAC mom. What have you seen with that? I remember you told me a story before we started recording about one of your ICAN parents about after they had their CBAC.
Mari: Yeah. I facilitated a conversation between two CBAC mamas. One mama who-- around 37 weeks pregnant, due to her blood pressure, had to actually just get a C-section right away. She didn’t even get that opportunity to go through labor and she also didn’t get to labor with her first birth.
She cried out all of her feelings and she went for her CBAC and it was what it was, right? But she articulated feeling confident in her decision knowing this time around, having asked all the questions, understanding the benefits, risks, and alternatives. She felt empowered going into her CBAC. The mindset really helps in the process.
Versus another mother who was 42 weeks pregnant and had done all the things, and on her 42nd week, was walking into the hospital to have her Cesarean. She really tried until the bitter end. It was two months postpartum and she still hadn’t told anyone. She hadn’t talked about her birth. Obviously, we knew, because usually, like you were saying before, we start stalking them to see if they had their baby or not.
Julie: Yeah, we need closure.
Mari: We need closure.
Julie: Not to make it about us, because it’s not about us, but we wonder and are concerned.
Mari: Not at all about us, but because we want to hold space for them, right? Not so much because we’re like, “Did you get your VBAC? Let’s check the box.” But more so because we want to hold space for them. We know it’s a very delicate time and it’s something that you can’t hide. You know, everything else that happens to you is something you can hide, but a baby is something that is physically, outwardly-- it appears. You have people in your face and you’re also still processing, and you can’t hide anywhere. We all know. Your baby can’t be in there for 12 months, so we know you had your baby.
So I said, “Cara, listen. Are you going to come to the next ICAN meeting? I’m going to make it all about CBAC because I want everybody to be able to also process their CBAC.” A lot of our conversations in ICAN are about VBAC only because we are serving that kind of community and that’s the women coming in the door. It doesn’t mean that we don’t do education and support for a Cesarean birth and talk about birth trauma, but predominantly a lot of VBAC mamas come to our meeting.
And so, she genuinely thought that she wasn’t welcome back because she didn’t have a VBAC. I said, “Of course, you are welcome. We are first and foremost education and support for Cesarean birth. We are not first and foremost only for VBAC.”
But it really got me thinking that if that’s the impression that she got, how many other women who got their CBAC and therefore didn’t return to these spaces that before that were circles of strength for them and support?
We’re still all the same. We’re still mamas just wanting to advocate for our wants and desires for our bodies. But ultimately, every baby makes a decision of how they’re going to enter this Earth. And so, I think that’s what we all wanted to talk about.
Now I’m curious, I know Allie has been an active listener--
Julie: Yeah, I know. I was just going to ask her.
Processing a CBAC as a doula
Mari: Yeah. As a doula, Allie, how have you held space or how do you process throughout that when you’re dealing with your clients who have CBACs?
Allie: I think one of the biggest things that I took out of my VBAC Link training was sort of separating-- even just the acronym, VBAC, is full of outcomes. We are immediately defining outcomes. I think one of the most amazing things I got out of my training through VBAC Link was really breaking it down from that and understanding that there’s empowerment in any birth outcome. Any birth outcome can be a positive birth.
And so, when I’m working with clients and it’s becoming a CBAC, we do a lot of positive affirmations, and a lot of slowing things down, and bringing it all back to, “This isn’t a rush. We have time to process this stuff.”
Julie was saying earlier something about how when you started out as a doula and you had all these thoughts. It was like the same-- when I first started out as a doula, one of the first births I ever attended was a Cesarean. I was so nervous. We had labored for 40 hours and it was this whole thing. When the OB came in to consult with the midwife and with my client, I asked for everybody to clear the room. I turned out the lights and played their worship music, and just left the room and let them have their conversation.
She went for her Cesarean. Her epidural was garbage and they didn’t do a spinal, so she ended up under general. She didn’t see baby for five hours. I was with dad that whole time. She finally came out and I was just like, “This is the worst thing in the world.” And she was like, “This was the most beautiful experience. This was amazing.”
It was really just one of those times where it flipped something in my head to stop obsessing over outcomes and start obsessing over people’s feelings in the moment.
Like you said, you made a fear-based decision. I want to be supporting people in the moment to not be in that place in their mind that they’re going to that kind of decision making. I want to go back to your story though, Mari. One of the things that I really took away was the fact that you said, “I didn’t know anything my first time. I didn’t know anything. I watched these three YouTube videos and tried to compare at all,” but you did!
You knew so much because you knew when you felt like you were dying. And you knew what was not okay when they asked you, “Is there abuse at home?” with family members in the room. You knew so much. We know so much instinctually. And so, I think you need to give yourself some credit there. For sure.
Mari: Oh my god, Allie. You’re going to make me cry. You’re so nice, thank you.
Allie: I loved that part though when you said that, because I feel like as doulas and as birth workers, we don’t know a lot of stuff. I just peruse through The Birth Partner when I’ve got nothing else to do and I’m drinking my coffee in the morning, but there are also things that you can’t read in any book that are just instinctual to us. You had so much of that in your first birth.
Even though you had more, maybe “knowledge” behind you in your second, and you switched providers, and you knew how to advocate for yourself, and kept trying to find the person that was going to work for you, in the first you knew so much. You knew so much to actually take it to the next level and report people. I honestly-- I am in such awe of you. You’re such an inspiration. It was so wonderful to hear your story. Thank you for sharing.
“Everything Left Unsaid” project
Mari: Thank you for having me. This conversation needs to continue. I don’t know how you guys feel about this, because The VBAC Link is your platform, but you know to the mama hearing this and resonating with this story, I think we should all write that letter to either the birth we wished we had, or that letter to the unsaid things that weren’t said to that doctor, or throughout that experience so that we can release all that shame that we carry, and sometimes all that sorrow that comes with the outcome that wasn’t what you desired.
That way, it can allow us to focus on what we did know and what we did experience. I always try to remember, “Sorrow prepares you for joy.” We have to feel the sorrow and release it. I am personally going to write a letter that I’m probably never going to mail. But I’m going to write a letter to all those doctors who said I couldn’t do it. I do encourage women to do that. If we get a bunch of letters, I would love to read them all. It could be so healing.
Julie: We should do an episode where we just read letters that these women write to their doctors, but obviously don’t include their personal information or whatever. Oh my gosh, let’s do it. Let’s get back together.
Allie: I’m literally having a letdown thinking about this right now.
Julie: Obviously, we’re going to have to kick Meagan off the episode because she was not here for the decision. No, we’ll have you back Allie. We’ll have Mari back and we’ll have Meagan. Let’s spread across our platforms. Allie, you too, and Mari. Let’s ask women to email us their letters. They don’t have to include details. They don’t have to go through their personal information. They can even make up their own Gmail address that’s completely anonymous and send it to us. And we can read that letter.
So if you know me at all, then you know I love giving homework to my clients. I am giving homework to every single person listening to this episode right now and your homework is:
Write a letter of the things you wish you would have said, or wish you could say, to your provider’s face about how-- anything about your feelings about how your birth went.
About how the things that they said hurt you, or about how-- Meagan, after her birth, the first words out of her mouth after her VBA2C was, “Screw you, Dr. Blank,” because I’m not going to throw anybody under the bus, even as much as we would want to. She said, “Screw you, Dr. Blank,” who told her, “Good luck out there. Nobody’s going to want you.”
She just said, “Screw you.” Even if it’s just that short, then email it to us at info@thevbaclink.com or you can send it to us on Facebook or Instagram, or Mari-- any of her connections that we are linking down below. Get us the letters and we are going to do an episode where we read these letters. We’ll probably talk a lot about them too, to be honest.
Mari: Absolutely, absolutely. I see that being such a healing process because at the end of the day, everything left unsaid is going to keep festering inside of you. And you know, I just want women to live motherhood with joy, but there are so many things that keep us from our joy, so I love this. Thank you for collaborating with me on it.
Julie: Yes. “Everything Left Unsaid.” That’s all we’re going to call the episode. Not this one. This one is going to be called something else, but our episode where we read all the letters-- it’s going to be called “Everything Left Unsaid.” I’ll write my letter. Mari, you write your letter. Allie, are you a VBAC mom, or do you want to write a letter to anybody? Any provider? Your provider or providers maybe you’ve seen because there are a couple providers of births that I have attended that I would really like to write letters to. Do it.
Allie: Oh, I’ve definitely got ideas.
Julie: Done. Okay. Let’s ready, break. And then we will meet back-- let’s see. I’m trying to plan this out so that everyone listening now can know when this is going to be coming. Let’s see if I can actually block it out right now. It’s kind of far because we are recording, so we don’t have to record anything through the holidays. It would probably be the end of January, like January 20th. I’m putting it in my spreadsheet now.
It is officially known that January 20th, the episode that will air then shall be called “Everything Left Unsaid.” We will read all of the letters. Send them to Mari. Send them to me. Send them to Allie. Send them to Meagan. Get them to us anyway, however ways you want and we are going to hash it out.
Allie: I’ll make a box on my contact on my website and link it in my bio so you don’t even have to put an email address in.
Julie: Perfect. I’m going to figure out some way to do that on our end as well. (Inaudible) does our website right now. I don’t have to do it anymore and it makes me happy, but then I’m like, “Wait, how would I do that now?” Oh, “Everything Left Unsaid.” I love it. Oh my gosh, yes. This is going to be really powerful.
I’ve got a couple of things I’ve got to do to wrap up the episode. First of all, Allie, thank you so much for being my co-host. I’m so glad to have you on here and your insight, and we are going to be welcoming you back. Block it out, January 20th everybody and then Allie, people in Canada. Vancouver. North Vancouver, right?
Allie: Yep.
Julie: How do they contact you?
Allie: Yes. So, I am on Instagram @nsdoula and nsdoula.com if you want to get in touch with me. Thanks so much for having me on. This was really amazing and Mari, again, thank you so much for sharing your story. It was just so wonderful and beautiful to listen to. I’m not lying when I say I think my bra is soaked. (Inaudible) no, I’m like, “Oxytocin!”
Mari: That’s hilarious. Thank you so much.
Julie: I love it. Again, echoing what Allie said. Mari, you are amazing. Oh my gosh, I am so, so glad that you made that video because that video has brought so many good things to the birth space and it’s even still doing good right now, and on January 20th, and whenever we record in January, and it’s powerful.
You are powerful and I hope that you, and every other person who has given birth by unplanned Cesarean, can look back and see that there is strength and find some strength in their story even if they don’t feel anything but miserable about it right now, because no matter how your babies are brought into this world, you are an incredible woman of strength and you did some really, really amazing work. We are all proud of you for that. So, Mari. How can people find you? Again, we are going to link everything to both of you guys in the show notes.
Mari: Absolutely. Well, thank you both so much for having me and for your kind words, both of you. I could be reached on my website, which is www.marivega.me, or on Instagram @mari_vega. And again, Facebook was Mari Vega Motherhood. Thank you so much for having me.
Julie: Perfect, and thank you. Again, guys, you can find that information in the show notes, and stay tuned. January 20th is the day. Send us your letters to any three of us or email them to info@thevbaclink.com.
Closing
Would you like to be a guest on the podcast? Head over to thevbaclink.com/share and submit your story. For all things VBAC, including online and in-person VBAC classes, The VBAC Link blog, and Julie and Meagan’s bios, head over to thevbaclink.com. Congratulations on starting your journey of learning and discovery with The VBAC Link.
