
431.8K
Downloads
164
Episodes
Here at The VBAC Link, our mission is to improve birth after Cesarean by providing education, support, and a community of like-minded people. NO matter what way you choose to birth, we want to support you during your journey in helping you know your options for birth. Welcome to our circle; we are so glad you are here!
Here at The VBAC Link, our mission is to improve birth after Cesarean by providing education, support, and a community of like-minded people. NO matter what way you choose to birth, we want to support you during your journey in helping you know your options for birth. Welcome to our circle; we are so glad you are here!
Episodes
Wednesday Feb 03, 2021
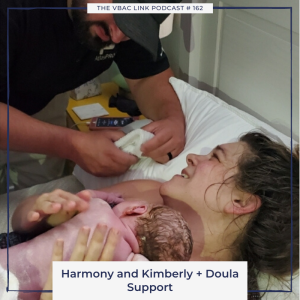
162 Harmony and Kimberly + Doula Support
Wednesday Feb 03, 2021
Wednesday Feb 03, 2021
In a VBAC Link podcast first, we are joined by both a parent and her doula to share an inspiring VBAC story with us. Harmony, a VBAC mom, talks about her journey to better health, trusting her intuition to feel confident with an out-of-hospital birth setting, and how crucial it was to have a rock-solid support system. Kimberly, one of our VBAC Certified Doulas, chimes in to share her unique perspective on Harmony’s birth.
Their sweet friendship shows us just how special the bond can become between you and your doula. Kimberly says to Harmony, “Stories like yours are exactly why I am passionate about VBAC. I was honored to get to be a part of your experience.”
Additional links
How to VBAC: The Ultimate Preparation Course for Parents
Advanced VBAC Doula Certification Program
Find a VBAC Link Certified Doula
Kimberly’s Website: Dulce Birthing Services
Episode sponsor
This episode is sponsored by our signature course, How to VBAC: The Ultimate Preparation Course for Parents. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course. Together, Meagan and Julie have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head over to thevbaclink.com to find out more and sign up today.
Sponsorship inquiries
Interested in sponsoring a The VBAC Link podcast? Find out more information here at advertisecast.com/TheVBACLink or email us at info@thevbaclink.com.
Full transcript
Note: All transcripts are edited to correct grammar and to eliminate false starts and filler words.
Meagan: Happy Wednesday, everybody. You are listening to The VBAC Link podcast and as always, we are excited to be with you today. Today, we have something special for you. We have actually never done this before. Today is going to be so fun to hear the stories from both sides. We have both a parent and her doula with you today. They are going to share a VBAC story.
We have Harmony and Kimberly. Harmony is the mom and Kimberly is the doula. She had a VBAC just six weeks ago, so we are so excited to hear her story. As always, we have a Review of the Week before we dive right in. I will turn the time over to Julie.
Review of the Week
Julie: I am really, really, really excited about the story too. Kimberly has been on our podcast a couple of times. She is on our Doulas Tell All episode, and she shared her VBAC after four C-sections story, so if you want, you can just go back to the search bar, search for Kimberly, and her story will come up as well.
I am really excited to have a doula-parent duo on as well. We are so grateful for them. Harmony and Kimberly are from Texas-- just outside of Austin, Texas it looks like.
I am going to read a Review of the Week. This review is from angelle.boyd on Apple Podcasts and the title of her review-- it’s really long but it’s cute. She says “Thank you, ladies! Best podcast to help prepare for a VBAC and an amazing birthing experience.”
She goes on to say, “First off, just had my successful unmedicated VBAC at the hospital in June all thanks to this podcast and you wonderful ladies. During my TOLAC, I continued to think of all the amazing stories I listened to on this podcast to get me through labor. Shouting out loud during labor, “I am a woman of strength and my body knows what it is doing,” was so empowering! I started listening to this podcast and could not stop. Each episode has something that can contribute and help women during their birth journey. I love how encouraging each episode is and that it goes through all types of scenarios that can happen during birth, regardless of trying for a VBAC.
This can help better prepare any woman for all types of outcomes because let’s face it, giving birth is unpredictable! So thankful for listening to all the suggested tips to having a VBAC. I actually did every single one of them and happily had an amazing VBAC. Can’t thank you, ladies, enough, and hope this continues to help change the way our society sees birth! Yes, to women of strength! We got this!”
Boom. I love that review. That was exciting. Congratulations, angelle.boyd on your VBAC. We are so happy for you. Now, without further ado, let’s get to the story because we have a VBAC Trained Doula and a parent who had a VBAC. We are ready to rock and roll.
Episode sponsor
Julie: Do you want a VBAC but don’t know where to start? It’s easy to feel like we need to figure it all out on our own. That’s what we used to do, and it was the loneliest and most ineffective thing we have ever done. That’s why Meagan and I created our signature course, How to VBAC: The Ultimate Preparation Course for Parents, which you can find at thevbaclink.com. It is the most comprehensive VBAC preparation course in the world, perfectly packaged in an online, self-paced, video course.
Together, Meagan and I have helped over 800 parents get the birth that they wanted, and we are ready to help you too. Head on over to thevbaclink.com to find out more and sign up today. That’s thevbaclink.com. See you there.
Harmony’s story
Meagan: Let’s get into the story. So, so excited. I am excited to see how this flows, and how you guys chime in, and your different perspectives. I am so excited. Let’s turn the time over to you fine ladies.
Kimberly: Hi, Harmony.
Harmony: Hey, Kim. We haven’t seen each other since the birth, but we are planning to this Friday actually. So, this is kind of cool. Yeah, the same goes for me that if you remember something that I don’t because it was a little blurry at points for me understandably, please, you can chime in whenever.
Well, I guess I will just start by saying that I got pregnant with my daughter in 2015. My husband and I had been married for a couple of years. Sometime during that first couple of years, I actually was diagnosed with PCOS by my doctor.
Meagan: Which is Polycystic Ovarian Syndrome.
Harmony: Yeah. Polycystic Ovarian Syndrome. I remember coming home and telling my husband because I was pretty upset. I really wanted to have a baby. I just was worried about the fertility issues with that. We waited. I think it was in 2015 that we started trying to get pregnant. We had actually moved to Tulsa temporarily-- didn’t know it was temporarily. We are back in Texas now.
We had been there for about a year, year and a half and started trying to get pregnant. I got pregnant right away. That in and of itself was huge for somebody with PCOS. I went through that pregnancy and had some blood pressure and blood sugar issues. The blood pressure issue was why I got induced. My doctor was wonderful. He basically just tried to get me to the very end before he did any type of intervention. I just wanted to say that up front, that I know my experience is a little bit different because my doctor-- his wife actually had a VBAC. He made a point to tell me that his C-section rate was really low. He was well-connected with the midwives in the area and so I knew I was in good hands with my pregnancy and that he wasn’t going to push me to be induced or have a C-section unless that was the option for us.
I reached the end of my pregnancy and my blood pressure just kept increasing. He said, “Well, I think what we should probably go ahead and do is induce you,” because he checked me. I had asked him to check me. I should probably say that as well. He didn’t do routine cervical checks. I asked him to check me that Friday and he said, “Okay.” I think I was dilated .5-1 centimeters, so not a ton.
He said, “Since your blood pressure is going up, I’d like to go ahead and induce you.” I shared with him that I was concerned about that because I didn’t want to have a C-section if I could help it. He said, “I totally understand that.” He said, “I just want to tell you that there’s nothing wrong with you if you end up in a C-section. I am still going to make sure she is on your chest immediately.” He really tried to encourage me. He said, “I don’t see it going that way, but if it does, I want you to know I will make sure that all of that bonding happens.”
I went to the induction feeling like, “Well, this is the option.” I think they used Cervidil. Is that a common thing that is used usually? The night before, they inserted that.
Meagan: Yeah, Cervidil. It’s a pill.
Harmony: Okay, yeah. That’s what it was, and then I had some cramping. My husband and I had been watching Lost on TV or on Netflix. So, we started watching that. He stayed there with me, but I couldn’t get comfortable. I was feeling crampy and I couldn’t sleep very well. By the next day, I did start to have some contractions after they gave me a little bit of Pitocin. My daughter’s heart rate immediately dropped after having the Pitocin. My doctor was in a delivery and I remember the nurses rushing in, turning me over on my side, putting oxygen on me. It was very scary.
Unfortunately, he wasn’t there at the moment, so I didn’t have that reassuring comfort from him that, “You are going to be okay. We are going to figure this out,” but he got there as soon as he could and explained to me what was going on, that she wasn’t really responding very well to the Pitocin. We talked about trying some other interventions and he said, “I can insert a Foley bulb, and take you off of the Pitocin, and see if we can manually get you to dilate that way.” That’s what I decided to do.
He was actually right in the middle of checking my cervix when we talked about that. I always tell this because it makes me laugh, looking back. He’s really funny. He said, “Okay. Well, I am going to go have them get the Foley bulb. I am just not going to take my hand out at this point,” because he knew it was really painful for me every time he had to do that. The nurses went to go get the Foley bulb and when they left he said to me, “So, how’s it going?” trying to make it not so awkward because he was literally just sitting there with his hand in my vagina.
But that’s part of what I loved about him, was that it wasn’t-- he really respected me and he was trying to make it as easy as he could for me. So, he inserted the Foley bulb and I think I dilated. I still was having contractions even after they dropped it down for me.
This is where it gets a little blurry for me because I don’t remember if I still had a little bit of Pitocin. Her heart rate dropped two more times after that and it was scary for me. That was probably, aside from-- the C-section wasn’t really that scary for me. It was hearing her heart rate slow down that really terrified me. So, after that third time that her heart rate dropped, he came in and sat down on the bed beside me and he said, “Look. I know neither one of us wanted it to go this way, but this is what is happening at this point.” He said, “I don’t really want to rush you in an emergency where we can’t control how she is born and have her there on your chest. So I think at this point, the best thing to do is go ahead and do the C-section.” I said to him, “Yes.” At that point, I was like, “Yes, please. I can’t hear her heart rate drop one more time.”
They wheeled me in there and they made sure I was all set up. They were very respectful. I know in the stories that I have heard since my C-section, I realize how fortunate and blessed I was to have the doctor that I had, and have the nurses, and have the anesthesiologist that I had because there are some pretty horrible C-section stories. They got me all set up and pretty soon, he had her out and put her on my chest.
It wasn’t what I saw for my birth, but it was our story and I was able to hold her. I was so exhausted at that point from all the medication and just the birth itself. With the hormones, I was shaking and everything like that. I was afraid I was going to drop her. I remember saying to the neonatal nurse, “I want to hold her, but I am afraid I’m going to drop her.” She was like, “You’re not going to drop her. We are right here. You can hold her.” Again, they were really supportive.
So, of course, a C-section recovery isn’t fun. I had to basically recover from a major surgery while learning to become a mom for the first time. She ended up having to go to the NICU the next day because she had tachypnea, which is rapid breathing directly caused from the C-section because she didn’t go through my birth canal. That wasn’t fun either because I had to be separated from my baby there in the hospital.
We eventually got home and moved on with life. I knew that-- I remember my doctor coming into the hospital room, I think it was the next day or day after, checking on me, and I immediately knew when I was there in the hospital that I was going to have a VBAC the next time I had a baby. I was already planning it. I said to him, “So, when can I get pregnant again?” I could tell in his face he was just like, “I can’t believe you are asking me that right now after having just had a C-section.” But I was already looking forward to the VBAC because I knew that we had wanted to have more kids.
I thought we would get pregnant sooner, but time passed quickly it feels like. My daughter was-- I think she had just turned four and we decided, “Okay, let’s go ahead and start trying for another baby.” We did. I think I got pregnant pretty much in the same amount of time that was with my daughter. I have been very blessed to get pregnant really fast, like I said, especially even with PCOS.
Oh sorry-- I should back up and say that the time in between that pregnancy, I really looked at why I had ended up in that C-section. Sometimes, there is not an explanation and sometimes it just happens. For me, I knew that it was my blood pressure that had caused me to have to be induced. I knew that for my own body, when I carry more weight, my blood pressure-- it doesn’t take long before my body goes, “Whoa, whoa. Danger,” and my blood pressure shoots up.
My body, I thought, just couldn’t handle that additional weight from the pregnancy. I decided to lose 50 pounds. That was actually my goal. I had already lost the 25 that I gained with my daughter.
Meagan: Nice work. That’s awesome.
Harmony: Thanks. Yeah, that’s the most weight I have ever lost. I have a hard time losing it if it is just because I want to look better. It was more like-- it was the biggest motivator I ever had, was having a vaginal birth. I really felt like in my heart that if I could get to a better way that it would just be less pressure on my body. I walked and I actually just tried to let it come off easily. I didn’t do any crash dieting or anything like that. I think it took about a year. I had gone and seen the birth center that I was interested in.
So, I was planning all this stuff all along even though I wasn’t even pregnant yet. I wanted it all lined up so that when I got pregnant I would know what my plan was. During that time, I lost that weight and I would walk. While I was walking, I was listening to The VBAC Link podcast, actually, every single day that I would walk. I did that to normalize in my mind the VBAC experience. I wanted to feel like women are having this all the time. In the medical world, it’s talked about as being super risky and scary, but as I looked at the data and the information, I knew that wasn’t true. I tried to normalize all of this in my head and make it not so scary for myself.
It turned out that quite a few women in my life-- as I talked about that I was going to try for this VBAC-- had VBACs themselves. It was funny how-- I am a believer and a Christian. It was odd to me how in my life I found that around me there were about four or five women that were sprinkled around me that had VBACs and even more made me feel like, “Yes. This is okay for me. This is safe and women are doing it. It just encouraged me even more.”
I visited a birth center after I got pregnant here in Texas-- Central Texas Birth Center in Georgetown. It’s about 35 minutes from me. I went in with my mom originally and when I walked out, I said, “I feel like I’m going to give birth here.” I just felt really strongly. My mom said, “I feel the same way.” Neither one of us have had experience birthing out of the hospital. That feeling was just so strong that I knew in my gut that that was probably where I was going to have my baby.
I went back with my husband and he said, “Yeah.” He said, “I feel like if it were me and I was having this baby, I would do it in a hospital. But I feel like this is right for you and that you are going to be supported here.” He just wanted to know that if anything happened that they had a transfer protocol in place. And they did, but I definitely in my mind was like, “I am not even going to talk about that.” I didn’t want to scare myself or speak something over me that wasn’t going to happen.
But he was very supportive. My whole family has been very supportive. I know that Kim-- I don’t know if you want to talk about that Kim, but she said to me that the support that I had around me was really maybe a little bit unusual because it was my mother-in-law, my mom, and my husband. They were very 100% in with me which was great.
Kimberly: From a doula perspective, it was really fantastic to walk into a situation that all of your immediate family was super supportive of your plan because so often we play the go-between of “Mom is too nervous,” or “Dad is too nervous,” and they don’t want the birth plan to go-- They have different ideas of what they think is safe or normal and to see that your whole family was on board with this plan or birthing outside of the hospital with the provider that you had chosen. It made your job easier. It made my job easier and, I think, ultimately led to the best support you could possibly get in your birth. Not just in the pregnancy, but there was no wavering. There was no fear, no wavering of emotion in the moment when you needed everybody to be steadfast for you.
Harmony: Yeah, definitely. I know I jumped ahead a little bit with that, but I feel like that was just really important to say that it helped me make my decision to see my husband so calm and confident with it. It was new for me to even consider birthing out of the hospital. But I just felt like-- I had looked at providers through the ICAN Facebook page. I did some investigating and I just did not feel in my heart for me that I was going to be supported the way that I wanted to be for a VBAC.
I didn’t want to be under a time limit at my gestation where I was going to have to be induced. That was my own personal feeling, a decision that I wanted to be in the right place so that I could let my body do what I was going to do. I knew that there would be nothing more worrisome for me than feeling like I was on a deadline. I knew that that was going to make my blood pressure shoot up. I was like, “I’ve got to be able to relax here.”
I chose to go with that birth center. They were wonderful-- my midwife and all of the people there. At one of my appointments, I think I was about 10 weeks, I started taking my blood sugar. I started eating more lower carbs to try and head off any blood sugar issues. I also took some supplements to help with my blood pressure. I really went through that pregnancy with no complications this time. I had a lot more energy. I know it was probably taking the pressure off of my body.
I know that there are tons of women who have totally normal and totally healthy pregnancies with extra weight. I just want to be sure and say that too, that if you are plus size, that does not mean that you can’t have a VBAC. I did this for myself because of my own body. I knew that I needed to get some pressure off of my body. It was really important to me to say that because I don’t want anybody to hear that you are limited because you are more plus size or anything like that.
Meagan: Totally. Thank you for confirming that.
Harmony: Yeah. I didn’t want that to be misunderstood that I feel like you have to lose weight to have a VBAC because you do not, but I felt like my body did. I’m glad that I listened to my own body and did that because it turned out to be right for me. I didn’t have any complications.
I did also-- one of the things that I tried to do to set myself up for success was hire a doula, which is Kim, who you just heard earlier. We met on a Facebook video chat because COVID had just started happening. We had to set up a time and meet together. When I spoke to her, I knew that she had a lot of experience that I wanted. I can’t remember where I had read it, but I knew that you had had your own VBACs. That was important to me because I knew that you understood the mindset of feeling like it would be really easy for a woman that has had a C-section to feel like her body is broken. That, a lot of times gets pushed even further when a provider makes you feel that way.
So, I knew that she believed in them because she had them and I also knew that she had some experience in Spinning Babies®. I know we talked about that in our first video call. Spinning Babies®, and I asked her about the rebozo because I had read stories about how that has been helpful. You have a lot of other certifications. I can’t remember what they are in. Oh, I’m sorry. I should also say that I found her through Instagram. She came upon one of the stories for the Instagram on The VBAC Link and it said that she was a VBAC Link Certified Doula.
Julie: Yeah, when she first got her certification. We used to post those to our stories. We are not very good at that anymore. We should probably start doing that again, it sounds like.
Harmony: No, it was right after she had been certified, I think. I think you were the only one in Texas at the time. Is that right?
Kimberly: I was.
Harmony: Okay. It just so happened that she was only about 45 minutes away from me. That also worked out great. After I talked to her, I knew that she was somebody I wanted to go with. I wanted to also talk about how you have the added element of being pregnant during COVID during this time, and how I obviously didn’t expect that curveball. It scared me in the beginning because it was so new. We didn’t know anything about it.
Kimberly: I think when we-- after you interviewed me and hired me, there was the whole COVID thing and we had to meet over video. But shifting that direction because of COVID and doing the in-home visits was really important. I think it helped us bond better. When I showed up to your house the first time-- well, first of all, you had a different experience in that your Cesarean-- you didn’t necessarily have all of the negative associations that a lot of the women that I work with have with their Cesarean, that they feel like it was unnecessary.
So, it was great to get to walk into a situation where you were like, “That was my birth. It’s okay. I’m okay with that, but this is how my new birth is going to be. This is how this one is going to go.” It was great to get to not have to spend all of our time necessarily working through birth trauma, but really getting to focus on that prep for, “Okay, you had a hospital birth. Now, let’s prep you for an out-of-hospital birth and the differences, and really focus on comfort measures.” I think us being able to do it at your home-- I felt like it was a lot more of a comfortable environment. It really felt like just sitting down and chatting with a friend when we talked.
Harmony: Yeah, me too.
Kimberly: I couldn’t believe how fast time flew when we were there at your house just chatting, but I loved being able to have that moment and get your husband involved in a space where I knew he would feel more comfortable doing things and being active versus meeting somewhere in public. I think that really worked to our benefit.
Harmony: Yeah, I do too. I 100 percent feel the same way. I feel like I made a friend through this. It wasn’t just somebody that I hired to help me through my birth.
Kimberly: Absolutely.
Harmony: I definitely feel that way, too. I agree with all of that. I guess I will just start talking about the birth now. I wanted to spend some time on the other things because I felt like it was important to show that for me, this birth story started way back. It was all the footwork that I had to do ahead of time to make myself feel more comfortable going into the pregnancy that I wasn’t, hopefully, going to have the same complications. And then if I did, I would just feel like, “Okay. I did everything I could and that’s okay. I’m going to birth my baby the same way I birthed my other one and that’s okay.”
My due date was September 30th and I had an odd sensation that happened for me. I looked back, and on about 9/18, my in-laws were coming into town. They were coming in about two weeks ahead of time to try to be there for the birth. As I pulled up, I got out of the car. Around the same time I was pulling up and I got out to meet them, I felt this weird drop in my body. It was uncomfortable.
He had been really low. He was on my left side, head-down for most of the pregnancy. But this was painful, where I couldn’t straighten up my body. I was talking to my in-laws and I was like, “Sorry guys, I cannot walk right now. I can’t move.” I don’t know if that was him moving down even further. I’m not really sure. I think I texted both Kim and my midwife, Sally, at that point and said, “Okay, I don’t know what just happened, but I haven’t had this yet.”
So about 9/22, which was four days later or so, I started having consistent contractions as I was laying on the couch watching TV with my husband. I looked at the clock and they were coming about 10 minutes apart, but I didn’t say anything to my husband because I knew he was already kind of nervous about, “Okay, we need to make sure we are at the birth center because I don’t want to have the baby here at the house.” He was really afraid that he was going to have to end up delivering the baby.
Kimberly: I think that was his biggest fear the whole time.
Harmony: Yeah. Yeah, because we had some friends that told us that she had gone into labor. She was actually seeing my same midwife. She ended up delivering at home accidentally and her husband had to deliver the baby. He texted my husband the next day and my husband was like, “Whoa. that is not happening.” He was very freaked out by that.
He just wanted to make sure that we were really paying attention to the contractions. I was looking at the clock and they were coming about 10 minutes apart and I said, “Okay, these are coming 10 minutes apart.” I don’t know if that meant anything because I hadn’t gone into labor with my daughter naturally, so I just didn’t know. I texted-- I don’t know if I texted you or not, Kim. Do you remember?
Kimberly: I think you texted me the second day.
Harmony: Okay, I think maybe you are right. I know that I texted my midwife and she said, “Okay. That’s great. Go ahead and try to go to sleep and rest through them.” I mostly was able to sleep through them through the night. They would kind of wake me, but I was able to go back to sleep.
The next morning, I texted my midwife and she agreed that maybe this was just warming up to my labor, and I should focus on them and try not to track them. I know I didn’t do a very good job of that because I was very like, “Oh, these are happening. I need to start tracking these.” If I had to do it over again, I would have listened to my midwife. I would have tried to relax and not paid so much attention to them because they actually went on-- let’s see, until about 9/27.
I had prodromal labor for several days following this. Yeah, 9/24. It looks like that evening they were starting up again. They were still regular, so I tried to sleep through them, but they were getting stronger with each night. I started to get a dull ache in my lower abdomen, and my pelvis, and my back, and I just couldn’t get comfortable. I couldn’t sleep because they kept waking me up. They were strong enough where I found myself waking up moaning through them, but they were still very irregular.
I texted my midwife and she told me to still try to sleep through them. She was just telling me that sleep is so important. “You really need to try to rest,” but it was like I could not do it because they just kept waking me. I was feeling nauseous the next day because I hadn’t had any sleep. I was exhausted. When I would try to take naps and lay down, the contractions would start up again and they would be strong. When I would try to sleep, it was like I’d lay down and that was their cue to, “Okay, you’re going to rest now? Okay, now we are going to do what we need to do to try to get you into labor.”
On 9/25, I still had lots of aches, lots of pain in my pelvis. I went on a light walk because I was like, “I think I’m going to try to go on a little walk.” I live on my parents’ land out in the country. So, I walked down the street down their dirt road and back. When I got back, I felt like I needed to go to the bathroom. When I went to the bathroom, I noticed that I had a tiny brown-- I don’t know what you would even call it-- like, a piece of matter. I was like, “Well, that’s interesting.”
I texted Kim and my midwife at that point to let them know that I hadn’t seen that before, so I think some things may be starting to happen. After that, I tried to nap for a few more hours and the contractions just kept coming when I would try to go to sleep. The next day, I texted my midwife and said, “I’ve had contractions all night, but they are not coming closer together. They are getting harder as I sleep.”
The next day, I texted my midwife because I had had painful contractions through the night and they kept me up again. It was just prodromal labor, which I guess everybody talks about, and then, I didn’t know that was what I was experiencing. But I would have to get on my hands and knees, I would wake up from the contraction, get on my hands and knees to get comfortable. I would walk around the room. I’d have to lean over the bed. I just couldn’t lay down and contract.
I think it was the following day on 9/27 that I was in the bathtub trying to get some relief and I decided to call Kim. I felt bad because I could tell I woke you up. I think it was early that morning and I just--
Kimberly: It was early, but I live that life. I expect it.
Harmony: I know. I was like, “She’s probably okay.” I was always like, “I hate inconveniencing people,” so I was like, “No. I don’t want to call her, but man these contractions.” I don’t know if this is labor that I am in. If it is time to do something, or you just don’t know.
Julie: I think it’s so funny when people say that. They have said that to me too like, “Oh, I am so sorry I had to call you at 3 o’clock in the morning because I was having a baby,” and I’m like, “No. You are literally paying me to wake me up at 3 o’clock in the morning.”
Kimberly: This is what you hired me for.
Meagan: I tell people if I had a problem with waking up at 3 o’clock in the morning, I clearly chose the wrong career.
Julie: I wouldn’t be a doula.
Harmony: Yeah, exactly. But when you were in it, you were just like, “Is it just me making this a big deal? Do I really need to call somebody?” I was afraid that I was like, “Okay, I just need to hang in here,” because I was still just trying to rest, but I couldn’t do it and they were getting worse. Kim told me to do some inversions. Maybe you want to talk about that part, that you felt like he was just trying to get in a good position and that’s why I was having them.
Kimberly: Yeah, sometimes prodromal labor can be caused just by something minor and baby’s position. Not always the case, but it was worth a shot. The inversion helps dislodge baby just enough so that they can make enough of a rotation with their head or their body and correct themselves. Sometimes that can cause things to pick up once they start again and turn into active labor.
Meagan: I was just going to say, and it’s actually stopped labor to allow moms to totally go to sleep because it fixed the baby’s position and helped the baby, right?
Kimberly: Absolutely.
Harmony: Yeah. From my own perspective, I think that I just could not get comfortable laying down because he was probably in an awkward position. When I would have those contractions, getting up on my hands and knees or walking around the room, that seemed to be the only thing that would give him a little bit of room.
So, I went into the living room and I did some inversions. I called my mom and she came down to support me. At that point, I was in tears because I was just so tired and they were hurting. I wasn’t sure what was happening, but I did a couple of those inversions. I cried through them. But pretty soon, they got more bearable. I didn’t feel the same, like he was large, which was what I kind of felt like. My mom actually did do some belly sifting with the rebozo that Kim had left for me. There were lots of tears. I was tired, but I was feeling like, “Okay, something is starting to happen, I hope. I hope it doesn’t go on like this forever.” I tried to take a nap that day, but I couldn’t. I couldn’t rest. I didn’t go into this with a lot of rest as you’re probably gathering.
That night, it was September 27th. I talked to both Kim and my midwife, Sally. Sally really encouraged me, “You really need to rest if you can at all. Why don’t you go ahead and try to take some Benadryl or have a glass of wine and just see if you can go to sleep?” I had some Benadryl on hand so I did take a couple of pills. I got in the recliner because-- I talked to Kim about that too, that I could not lay down and feel comfortable.
I know it’s not preferred to recline, but when we talked, we decided if that was the only way that I could get rest, then that was probably what I should do. My husband and my mom-- my mom came down to be with me from her house. My husband, mom, and I watched TV. They turned the TV on and I decided not to track my contractions because my midwife told me to do that to focus on trying to get rest. My husband said, “Okay. I am going to track them because I want you to rest, but I want to make sure that if we get close enough, that we have enough time to contact Kim to come because she told me to call her when they were about 5 to 6 minutes apart.” I think that was because of his positioning. Right, Kim? That he was head down, and he was low and on my left side.
Kimberly: I know we talked about intensity too, and monitoring for changes from what I had been. If something’s shifted from what you have been experiencing, then that was probably things ramping up. Then, I would want to be heading your way.
Harmony: Yeah, definitely. I had given my husband my midwife‘s number and Kim’s number just so that he would have it in case I wasn’t able to contact them. I had dozed off and on in the chair, but I kept having the contractions. I didn’t know how far apart they were. They would wake me up. I would look over at my husband and he would time them as I was having them. At one point, he paused the TV show and said, “Okay. These are about 5 to 6 minutes apart. It’s been that way for a little while, so I think we need to call Kim.”
In that moment, I think because I had had so much prodromal labor leading up to that I just was like, “No.” Again, I didn’t want to bother her because I felt like they were going to slow down again. I was like, “I don’t want to have her come all the way over here. She lives about 45 minutes away. I don’t want to have her drive here and them just stop again.”
We argued about that for a little while and he’s like, “I’m calling her.” So, he called her. I don’t know if you want to say anything about the phone call or anything, Kim, because I can’t remember the conversation very much at all.
Kimberly: Yeah, he made it very clear on the phone. He was like, “So, Harmony didn’t want me to call. But I think things are picking up. I would like for you to head this way.” I was like, “Okay. I’m coming.”
Harmony: After he got off the phone, I was like, “No, they are going to slow down.” My mom was like, “Harmony, she made a decision to come. You need to just be okay with that.” I was like, “Okay.” They tried to make it less like I was twisting your arm into coming. This is when I realized that as far as labor goes, time doesn’t exist. When you got there, it felt like it had been five minutes, but you are about 45 minutes away. I remember when you walked in feeling like, “Oh my gosh, she is already here. That was really fast.”
You came over and started immediately putting counterpressure on my hips because I was laying on the couch. It was just so good to know that you were there because I didn’t know what to expect. I had never had a natural birth before and I didn’t know when I needed to go. I would say, that’s so helpful to have a doula there really that knows because they have experienced it, and then I could relax, and have my contractions, and trust you to go, “Okay. I think we probably need to start thinking about heading over.”
From what I remember, there was a lot of rushing around by my mother-in-law, and my mom, and my husband making sure that we had everything in the bags that we needed. My dad came down to watch my four-year-old daughter, who was asleep when we left at about 1:00 a.m., and started to head over. My husband called my midwife and said, “Okay, we are headed over.” I know that we talked about not leaving too early because I wanted to make sure that I was really in active labor before I got in the car.
Kimberly: I think you were in good, active labor. I saw that you were in a good pattern and your husband being nervous-- I didn’t want that to affect you. I know that his worry was having a baby at home, so I didn’t want that nervousness to affect your labor. I felt like for everyone, the situation was better if we just went ahead and went, even though we still had a little bit of time that we could have waited. I think it allowed him the peace of mind so that he could relax and just focus on helping you.
Harmony: Yeah, exactly. I do remember you saying that now-- that you were like, “I think it would be a good idea. Let’s go ahead and go.”
We got in the car. You followed us in your car. I remember thinking that the contractions were going to stop when I got in the car because we had talked about how that could happen between the house and the birth center. But I didn’t. They kept coming. I remember feeling so encouraged. It was at that point-- and I know that sounds really weird, that it was that far into my labor. I was like, “I am in labor.” It was like it took that much for me to go, “Okay.”
Meagan: It clicked.
Harmony: I know. It sounds really weird because I had been laboring for a long time, but I think prodromal labor really makes you doubt when you are actually in labor.
Meagan: Totally.
Julie: Oh, it totally does. It totally does.
Harmony: Somehow, I remember saying to you, “Kim, I feel like I’m going to disappoint people”. Do you remember me saying that?
Kimberly: I do.
Harmony: I remember saying, “I feel like it’s going to slow down again. Here is everybody doing this for me and it’s going to stop.” But when I got in the car and they kept coming, I was like, “Oh my gosh. I’m going to have a baby.”
Kimberly: You were worried about that false alarm and I’m like, “Nope, this is what we do. Sometimes it happens and it’s okay, but I don’t think that’s happening.”
Harmony: Yeah, exactly. I remember asking you, “Are these going to stop?” when I was laying on the couch. You said, “I don’t think so. I think this is it.”
We got to the birth center and I remember having another really big contraction when I got out of the car. My midwife met us there and she did what you would consider a regular check-in. She checked my blood pressure, and took my temperature, and all those things, and then left me to labor which I think is great. That’s exactly what I wanted. And I had Kim there the whole time. We walked around the hallway. I labored on the couch and on the bed.
Something I wanted to say was how helpful the counterpressure was for me and that you did that even when I was sitting on the couch. She would push on my knees to create counterpressure. That would help me through those.
Kimberly: Your husband did a great job of helping with that too.
Harmony: Yeah, he did. He did great. He was very supportive the whole time, trying to be there for me.
So, let’s see. On the next morning-- it actually ended up being into the morning. I labored all night, and then my midwife came in. I was laying down on the bed trying to sleep through some of the contractions. I don’t remember everything word for word, but I remember her saying, “I think we should go ahead and check you,” because I don’t think I looked necessarily like-- and this is where you can tell me, Kim-- I don’t know that I looked like I was as far into labor as I was.
Kimberly: You were handling your contractions very well. Your face and your demeanor was very calm the way you were breathing through them, so I’m not sure if maybe she expected that you weren’t going to be as far along as you were, but you were laboring beautifully.
Harmony: Yeah, and later I said to her, “Did you think it was too soon?” She said, “I thought that it was a little soon, but it wasn’t. It was totally right.” She’s wonderful too, very supportive. Like I said, the whole birth center-- and I had a wonderful midwife that was very hands-off as far as my labor.
So when she checked me, I remember thinking, “What if I am not as far as I think I am?” But when she checked me, she said, “Well, you’re definitely in labor. You are at a 7.” I couldn’t believe it.
I couldn’t believe that I was at a 7 and that I had been laboring active labor that long, and been able to do it without saying, “I can’t do this,” or, “This is too painful,” because my experience with my daughter with the Pitocin was-- those contractions were horrible. They were right on top of each other. There was just no break at all. I think I dilated to maybe a 5 or 6 with her, maybe a 4 or a 5. I’m not positive. But after she checked me and said that I was a 7, I laid there for a little while. My husband was like, “You need to rest. Let’s try to rest for a little bit.” She said, “Yeah. Let’s close the blinds.”
It had become light outside and so my midwife said, “Let’s close the blinds and have you try to rest a little bit, then in a little bit, get you up and walking around.” I think we did that and then I got into the tub at one point, which I really wanted to do. I knew that would be very comforting to me. I stayed in there for a little while.
Again, I had Kim too. I remember getting in the tub being worried that my contractions were going to slow down, but you were tracking them. You were like, “Nope. They’re still coming. They’re still coming at that regular interval for you.” At that point, my midwife did check me and I was still at 7, but she could feel his head and my waters were intact. She said, “Do you want me to break your waters?” I was not sure what I wanted to do at that point, because I really wanted to not have any type of intervention at all. But Kim and I talked about it, and I talked about it with my husband, and we decided, I was at a seven. It probably was okay to go ahead and do that.
We did that and it didn’t take long before the contractions started to feel a little bit more like what I would describe just as-- I don’t know if I can do this. That started to come into my mind. I was like, “This is getting scary for me,” because I felt like-- when you know that you are about to make a decision by breaking your water that you can’t take back, and you can’t escape those contractions at that point, so you just have to go, “Well, this is going to be hard, but I have to see it through.”
I do remember getting out of the tub at one point, because I just felt like, “I can’t be in this tub by myself.” I started to feel like, “I feel really alone in this tub. I can’t be in the tub by myself. I have to get out.” So, everybody helped me out of the tub. At that point, I remember feeling a sharp, searing pain around my hips and abdomen. That scared me because I just didn’t know if that was my incision or not. Although the percentage of that happening-- isn’t it less than 1%? It still scared me.
My midwife came in at that point. I remember saying, “I am scared.” She said, “Well, what are you scared of?” I said, “I’m afraid that this is my incision.” I’m afraid that the pain that I’m feeling is my incision. She said, “Okay. Do you think that’s what is happening?” I remember before I could even think about it any further, I had another huge contraction that brought me to my knees. I remember my mom holding me against her and trying to support me. It was really hard for my husband and my mom to see me in so much pain. Although they were really supportive, I know that took a lot out of them as well. So, I remember that. I remember my mom holding me.
That obviously was not what was happening. As far as the incision rupturing, that wasn’t what was happening, but that fear is still there, even though it’s a small percentage. You have to choose to believe that it is okay and that the percentage of that happening is very small, and so that’s probably not going to be what happens.
At that point, I got on the bed because my midwife said, “Would you like to start trying to push?” I’m like, “Yes,” because what I had been told up to that point by a lot of women was, “It feels so much better to push because it’s like you were able to do something with that pain.” I was like, “Yes. Yes. I want to get on the bed and do that.”
I got up on the bed and that’s when it got really crazy for me. This is where, Kim, I could probably use some of your perspective because being in transition-- people can tell you how intense it is, but until you are in it, I don’t think you can really understand what that feels like. I remember saying, “I can’t do this.” I said, “I can’t.”
Kimberly: I think a lot of your pain too, just from my observation-- it does feel good for a lot of women to push, but if I remember correctly, you had a bit of a cervical lip that they were trying to get you to push past and that can definitely be pretty painful to try to be pushing past a cervical lip. So, I think that’s why yours maybe felt a little different, and of course, is going to give a different sensation that you weren’t expecting.
Harmony: Yeah. I know that my hips were in constant pain, which I guess was just them spreading. My midwife would say, “That’s your baby. Your baby is trying to come down,” because I was like, “Oh, my hips. I can’t do this. I need somebody to push on my hips.” I felt like I was out of control. It felt like there was a lot of noise in my head, which I realized was in my head later as I watched some video back. It was pretty quiet and calm, but in my head, it was like everybody was talking. I was screaming. It was like my perspective was off.
When you are in transition, it’s like you are in your own world. That was what was scary for me was when I started going, “I need you guys to take me to the hospital. I can’t do this.” I remember people saying, “No. No, you’ve got this. You can do this. Harmony, he is almost here. His head is right here. You can push him out.” That is so, so important to have a team of people that believe in you.
Kimberly: I think your husband reminding you, “Nope. This is what you told me you wanted. You told me if you said you wanted to go to the hospital that you didn’t really mean it.” I think him reminding you of that was really pivotal.
Harmony: Yeah, I did. I said to him, “I need you to understand how important this is to me. Right now, I know I can do it, but when I am in labor, I probably won’t feel like I can do it. So, I need you to say to me, ‘No. You can do this and I am going to help you get through this.’” He said exactly that. He said, “I remember saying to you that you may be mad at me right now, but I am just doing what you told me to do, and so, I need you to reach inside you and push him out.”
Kimberly: When you first said that you wanted to go to the hospital because you didn’t feel like you could do it anymore, from the other side, we could see his head when you were pushing so we knew how close you were.
Harmony: That’s the thing was like, I couldn’t see anything, obviously. One of the midwives actually offered to put a mirror. She said, “Look. Sometimes this helps.” I was like, “No, no. I don’t want to see it,” because I think there was part of me that felt like if I saw the baby’s head coming out-- I was already so overstimulated with what was happening, I was afraid it was going to send me over the edge on what was happening.
She was like, “Okay, okay. No problem. You don’t have to look.” I felt bad because I felt like-- maybe I didn’t yell, but I talked very strongly during the labor to some people. I said to her, “No, I don’t want to see it.” She was like, “Okay, no problem. You don’t have to look.” Then, at one point, people were saying, “Push, Harmony. You need to push.” I was like, “Stop telling me to push. I am pushing.” I wouldn’t normally talk to people that way. I said that to Kim. I felt so bad because I was talking to people that I barely knew that way and being very forceful, but you just don’t have it in you to think about your wording or your tone of voice.
At one point, they told me to reach down and feel his head because it was coming out. I reached down, but it did not feel like a head. I know that sounds really weird, but it didn’t feel very round, and so I guess that’s because he was trying to come through. The midwife assistant and I laughed about it because she said, “Yeah, you reached down and you went, ‘what is that?’” They were like, “It’s his head. It’s his head. He is trying to come out.” I think there was part of me that felt like he was never going to come out. I kept trying to push, but I was like, “Man. Why is this taking so long?”
At one point, my mom had to leave the room because I was in so much pain. She just said, “I had to leave for a second.” She actually got sick in the bathroom because it was so intense. Again, I don’t know what it was like from your perspective, Kim, but that may have just been--
Kimberly: Your mom was definitely struggling, but she was fantastic. I had one hip laying on the bed across the bed shoving on one hip and she was in there shoving on the other. You could tell she was ready for it to be over for you and you could tell how strong she was feeling your emotions.
Harmony: Yeah. I mean, totally supportive, but just trying to hang in there, I think. It’s just hard to see your child in pain. I even felt my husband at one point while I was pushing, I felt him start to shake. I looked up and he was crying. I thought that was because, “Oh, the baby’s head. He’s crying because the baby’s head is out.” But he told me later that he was crying-- he was like, “No. You were just in so much pain. It was really hard for me to see that.”
What’s cool about that too is, I feel like it bonded us even more in our marriage for him to see what I was doing to try to get the baby here. At one point I reached down again. That’s when I started to feel what is described as the ring of fire. I felt sharp, sharp, sharp, sharp pain in my vagina. I reached down and then I felt, “Oh, that is his head for sure. His head is almost out.”
That was what gave me the strength that I needed to feel that we were almost there. I pushed and I pushed.
Really quickly, I remember somebody saying, “Okay. Get on your hands and knees.” I did that as best I could. I felt a bunch of people help put me over on my hands and knees on the bed. And then, I was told to push some more and then all of a sudden, I felt the pressure go away and I knew. I remember in the video I said, “Is he here? He came out?” and he had. He had come out. I turned around and saw him.
I’m sorry. I am getting emotional. That moment was probably one of the best moments of my life to see him there and know that I had done it, that I had my VBAC, and that first of all, I was out of that pain that felt like I was just in this pain spiral that I couldn’t get out of. But that now, I had actually done it and he was here. That was one of the best moments of my life-- just being able to hold him and know that I had this accomplishment and that he was here, and safe. My husband was very emotional about it. Everybody’s crying in the video.
My mother-in-law and my mother were both there and got to witness that. My mom has said to me later, “I never had really seen a baby coming out of a vagina.” That was interesting to be able to know that was a new experience for her too. It was just a really wonderful moment. Afterwards, my daughter got to come in and get in the bed with us and see him. All of that, I have a video.
It was really wonderful to feel like I could have let fear dictate that moment. I could have tried to play it safe, which, for me-- and I am just speaking for me. For me, it would have been playing it safe to choose to birth someplace else because I was scared. But I chose to birth where I birthed because I wanted to have an untouched VBAC that could just allow my body to do it. I didn’t know how hard it was going to be if I’m being honest with you. I did not know that it was going to be as hard as it was. I still can’t believe that I did it, but I did.
I’m really glad that I didn’t just let fear take that away from me, that I got to have that wonderful moment when I pushed him out, and I got to have my daughter there, and see my husband see his baby for the first time on his chest in an environment that wasn’t medical, which-- for me, it was just a different experience than my previous birth, which is okay. Like I said, that was our story. The C-section with my daughter was still wonderful to have her on my chest and everything like that, but that was just a different experience that I got to have with my son.
So, yeah. I mean, I guess the number one thing that I would say is how important it is to build a team of people that believe in you and believe in VBAC 100%. That was part of why I was able to go through this pregnancy completely and not be rushed into a deadline going into labor or feeling like it needed to be controlled. It just was. It was what it was.
It was like I hadn’t even had a C-section before in how I was treated if that makes sense. It was just like, “Yeah. We are going to let you go through this pregnancy.” At the birth center, they believed that I could do it and my midwife like I said, was wonderful. I never felt along the way from anybody that they thought that it was going to go south. They all just believed that I could do it.
And when it came time for me to go into transition, and pushing, and I didn’t think I could do it anymore, it was really important that I had the people in that room. Everybody in that room was like, “No. You can do this.” It’s so important because you can’t necessarily see the finish line when you are in a lot of pain and it’s really intense. All you can think about is that and it’s our natural inclination to just be like, “How can I make this stop? I need an epidural,” but that wasn’t an option for me because I was at a birth center and that’s part of why I chose to birth in the birth center because I wanted to try to avoid interventions.
So, that’s pretty much my story. I don’t know if Kim wants to say anything else. I was interested to hear what her perspective was when they told me to get on my hands and knees because you could see things, probably, that I couldn’t see in that moment.
Kimberly: Yeah, so I was down by your hip pushing and I could see. You had birthed his head and he had a bit of shoulder dystocia. That’s when Sally started to move and I told you to flip over to your hands and knees because I knew that’s what it was going to take to get baby’s shoulder dislodged. And you were great. A lot of moms are like, “What? There is a baby’s head between my legs. How am I supposed to move?”
You did fantastic and that’s exactly what it took. It was quick. Stories like yours are exactly why I am passionate about VBAC. I was honored to get to be a part of your experience and I have a new friend, just simply.
Harmony: Thank you. Yeah, me too. I couldn’t have done it without you. I couldn’t have done it without anybody there because I needed that extra push when it came-- no pun intended. But I did need that extra push. I did need that from everybody else to tell me they could see the perspective and go, “No. You’ve got this. His head is almost out. I know that you feel like you can’t, but you can do this.”
I’m just so thankful. I’m so thankful for everybody in the room and so thankful for Kim. I’m so thankful for the birth center and I’m so thankful for my midwife and the assistant. There was another midwife there. And my mom, and my mother-in-law, and my husband, and how they were in it with me. They didn’t say, “Okay, yeah. We probably need to go to the hospital at this point,” because I was in pain. My husband said, “I wanted to do that, but when we would take your blood pressure, it was fine. When we would take his heart rate, he was fine. And so, I was like, this is what she told me to do and so I am just going to keep pushing her through it.”
That’s pretty much the story. I’m sorry if it was too long.
Julie: No, it was great.
Meagan: No, you are awesome. I loved that you two were able to bounce off. Where you couldn’t remember, she-- it was really cool.
Julie: Super fun.
Harmony: Yeah. I do remember trying to move and feeling like, “Oh, it feels like there’s something really big stuck down there.” And there was.
Julie: There was.
Meagan: Oh, a baby’s head. No big deal.
Harmony: I feel like I can’t move, but I did move. I got over on my hands and knees somehow. Yeah, I didn’t know that his shoulder was stuck. But, they got him out.
Julie: That’s awesome.
Harmony: He was 8 pounds, 2 ounces, so a full pound heavier than my daughter.
Meagan: Isn’t it crazy how that works?
Harmony: I know. My mom and I were talking about it and she was like, “Yeah, I don’t know.” With me, she had me vaginally. My brothers too, but with me, it was during the time when-- now, I think they can give you an epidural basically right before you push, but the way it used to be was like-- she was too far along. So when she got to the hospital, they were like, “Sorry. It’s too late.”
She just looked at my dad and said, “I can’t do this.” You know, because she had-- she was like, “I can’t do this. I can’t.” But she had had me vaginally and naturally, and she said, “I don’t remember feeling that pain in my hips, but that’s because you were my last baby.” So, I don’t know if for me it was because it was literally my first vaginal birth and he was pretty big. I think his head was 14.75 inches, and his shoulders were big, and his abdomen was almost as big around as his head, but I don’t know if that’s why I felt so much pain centralized in my hips.
Julie: Definitely could be.
Meagan: Could have been.
Julie: bigger babies, a little more pressure down there.
Harmony: Yeah, a little bit more.
Julie: Well, thank you so much for sharing your story with us. It was definitely a lot of fun to have both of you on.
If you are interested in becoming a VBAC Doula yourself, then go ahead and check out our courses at thevbaclink.com/shop and if you are interested, we also have a parent’s course that will make you and your doula the perfect powerhouse team-- confident and educated going into the birth space in order for you to have the very best, empowering birth experience that you possibly can.
Meagan: And if you are looking for a doula, go to our website, thevbaclink.com/findadoula, and find your state or your country because we have doulas in lots of other countries as well. Check it out and see if there is a doula near you. I promise you, these guys are amazing. These doulas are absolutely phenomenal.
Closing
Would you like to be a guest on the podcast? Head over to thevbaclink.com/share and submit your story. For all things VBAC, including online and in-person VBAC classes, The VBAC Link blog, and Julie and Meagan’s bios, head over to thevbaclink.com. Congratulations on starting your journey of learning and discovery with The VBAC Link.

No comments yet. Be the first to say something!